Summary: Neuroimaging study reveals those suffering from Gulf War Syndrome who experience chronic pain have increased volume in brain areas associated with pain processing and smaller volume in areas associated with pain regulation.
Source: SfN
The brains of Gulf War Veterans with chronic pain possess larger pain processing regions and smaller pain regulation regions compared to their healthy peers, according to new research published in Journal of Neuroscience.
Over one third of Gulf War Veterans experience widespread, chronic pain linked to a condition called Gulf War Illness. The underlying cause of the pain is poorly understood, preventing the development of effective treatments.
Ninneman et al. analyzed the brains of Gulf War Veterans with and without pain using MRI. The participants also completed questionaries about their pain symptoms, fatigue, and mood.
Those with chronic pain displayed smaller left and right insular cortices, two brain areas involved in regulating pain. They also had larger areas of the frontal cortex, specifically in regions involved in pain sensitivity and emotional regulation.
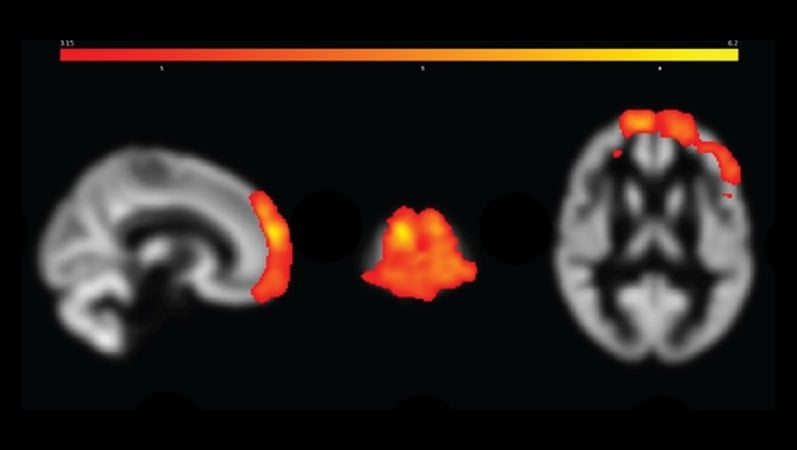
The structural changes were more pronounced in people with worse pain, but there was no relationship with fatigue or mood.
These results indicate the chronic pain from Gulf War Illness may stem from changes in how the central nervous system processes pain, rather than with issues with nerves or pain receptors.
About this pain research news
Author: Calli McMurray
Source: SfN
Contact: Calli McMurray – SfN
Image: The image is credited to Ninneman et al., JNeurosci 2022
Original Research: Closed access.
“Pain, but not Physical Activity, is Associated with Gray Matter Volume Differences in Gulf War Veterans with Chronic Pain” by Ninneman et al. Journal of Neuroscience
Abstract
Pain, but not Physical Activity, is Associated with Gray Matter Volume Differences in Gulf War Veterans with Chronic Pain
Chronic musculoskeletal pain (CMP) is a significant burden for Persian Gulf War Veterans (GWV), yet the causes are poorly understood. Brain structure abnormalities are observed in GWV, however relationships with modifiable lifestyle factors such as physical activity (PA) are unknown.
We evaluated gray matter volumes and associations with symptoms, PA, and sedentary time in GWV with and without CMP. Ninety-eight GWV (10 females) with CMP and 56 GWV (7 females) controls completed T1 weighted magnetic resonance imaging, pain and fatigue symptom questionnaires, and PA measurement via actigraphy.
Regional gray matter volumes were analyzed using voxel-based morphometry and were compared across groups using analysis of covariance. Separate multiple linear regression models were used to test associations between PA intensities, sedentary time, symptoms, and gray matter volumes.
Family-wise cluster error rates were used to control for multiple comparisons (α=0.05). GWV with CMP reported greater pain and fatigue symptoms, worse mood, and engaged in less moderate-to-vigorous PA and more sedentary time than healthy GWV (all p<0.05). GWV with CMP had smaller gray matter volumes in the bilateral insula and larger volumes in the frontal pole (p<0.05adjusted). Gray matter volumes in the left insula were associated with pain symptoms (rpartial=0.26, -0.29; p<0.05adjusted). No significant associations were observed for either PA or sedentary time (p>0.05adjusted).
GWV with CMP had smaller gray matter volumes within a critical brain region of the descending pain processing network and larger volumes within brain regions associated with pain sensation and affective processing which may reflect pain chronification.
Significance Statement:
The pathophysiology of chronic pain in Gulf War Veterans is understudied and not well understood.
In a large sample of Gulf War Veterans, we report Veterans with chronic musculoskeletal pain have smaller gray matter volumes in brain regions associated with pain regulation and larger volumes in regions associated with pain sensitivity compared to otherwise healthy Gulf War Veterans. Gray matter volumes in regions of pain regulation were significantly associated with pain symptoms and encompassed the observed group brain volume differences.
These results are suggestive of deficient pain modulation that may contribute to pain chronification.






