Reduced grey matter volume and enlargement of ventricular space appear to be early and progressive.
A study from Massachusetts General Hospital (MGH) Cancer Center researchers – the first to examine the effects of combined radiation and chemotherapy on the healthy brain tissue of glioblastoma patients – reveals not only specific structural changes within patients’ brains but also that the effect of cancer therapy on the normal brain appears to be progressive and continues even after radiation therapy has ceased. The report has been issued online and will appear in the August 25 issue of Neurology.
“It is well known that whole brain radiation can have adverse, neurotoxic effects and causes loss of brain volume in some individuals,” says Jorg Dietrich, MD, PhD, of the Pappas Center for Neuro-Oncology at MGH, senior author of the Neurology paper. “This is the first prospective and longitudinal study to characterize structural brain changes resulting from standard radiation and chemotherapy in patients with malignant brain tumors. Further studies with neuropsychological evaluation will be needed to characterize the functional consequences of these structural changes.”
The study enrolled 14 glioblastoma patients who were scheduled to receive chemotherapy and radiation after surgical tumor removal. Before and during the 35-week standard treatment protocol – which was not altered for the current study – MR images were taken with the high-power 3T scanner at the MGH-based Martinos Center for Biomedical Imaging. In the 8 participants for whom an adequate number of imaging studies were completed, whole brain volume – the overall amount of brain tissue – decreased significantly throughout the study period. The reduced volume was apparent within a few weeks after initiation of treatment and was primarily seen in grey matter. The size of the brain’s ventricles – cerebrospinal fluid-filled spaces deep within the brain – became progressively larger during the course of treatment, and changes were also seen within the subventricular zone, one of two structures in which new brain cells are generated in adults.
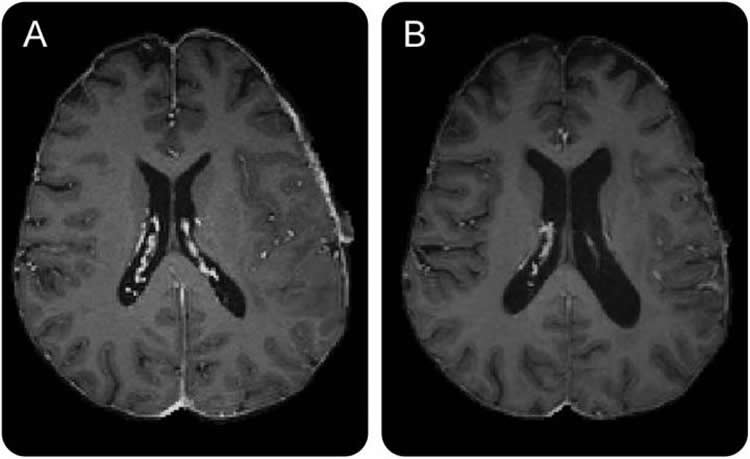
“We were surprised to see that these changes – reduced grey matter volume and ventricular enlargement – occurred after just a few weeks of treatment and continued to progress even after radiation therapy was completed,” says Dietrich. “While this was a small study, these changes affected every patient at least to some degree. Now we need to investigate whether these structural changes correlate with reduced cognitive function and whether neuroprotective strategies might be able to stop the progression of brain volume loss. Establishing novel imaging biomarkers of treatment-associated neurotoxicity – such as ventricular enlargement, which can be tracked with any MR scanner – will be a critical step towards developing more selective therapies that are targeted to the tumor and spare normal brain tissue.”
Dietrich is an assistant professor of Neurology at Harvard Medical School. Morgan Prust, MD, Martinos Center for Biomedical Imaging, is lead author of the Neurology paper. Additional co-authors are Kourosh Jafari-Khouzani, PhD, Jayashree Kalpathy-Cramer, PhD, and Pavlina Polaskova, MD, Martinos Center; and Tracy Batchelor, MD, and Elizabeth Gerstner, MD, Pappas Center for Neuro-Oncology – all at the MGH Cancer Center.
Funding: Support for the study includes National Cancer Institute grants R01-CA129371 and K24-CA125440A and the American Cancer Society.
Source: Katie Marquedant – Mass General
Image Source: The image is credited to NIH and is in the public domain
Original Research: Abstract for “Standard chemoradiation for glioblastoma results in progressive brain volume loss” by Morgan J. Prust, Kourosh Jafari-Khouzani, Jayashree Kalpathy-Cramer, Pavlina Polaskova, Tracy T. Batchelor, Elizabeth R. Gerstner, and Jorg Dietrich in Neurology. Published online July 24 2015 doi:10.1212/WNL.0000000000001861
Abstract
Standard chemoradiation for glioblastoma results in progressive brain volume loss
Objective: To investigate the effects of chemotherapy and cranial irradiation on normal brain tissue using in vivo neuroimaging in patients with glioblastoma.
Methods: We used longitudinal MRI to monitor structural brain changes during standard treatment in patients newly diagnosed with glioblastoma. We assessed volumetric and diffusion tensor imaging measures in 14 patients receiving 6 weeks of chemoradiation, followed by up to 6 months of temozolomide chemotherapy alone. We examined changes in whole brain, gray matter (GM), white matter (WM), anterior lateral ventricle, and hippocampal volumes. Normal-appearing GM, WM, and hippocampal analyses were conducted within the hemisphere of lowest/absent tumor burden. We examined diffusion tensor imaging measures within the subventricular zone.
Results: Whole brain (F = 2.41; p = 0.016) and GM (F = 2.13; p = 0.036) volume decreased during treatment, without significant WM volume change. Anterior lateral ventricle volume increased significantly (F = 65.51; p < 0.001). In participants analyzed beyond 23 weeks, mean ventricular volume increased by 42.2% (SE: 8.8%; t = 4.94; p < 0.005). Apparent diffusion coefficient increased within the subventricular zone (F = 7.028; p < 0.001). No significant changes were identified in hippocampal volume. Conclusions: We present evidence of significant and progressive treatment-associated structural brain changes in patients with glioblastoma treated with standard chemoradiation. Future studies using longitudinal neuropsychological evaluation are needed to characterize the functional consequences of these structural changes.
“Standard chemoradiation for glioblastoma results in progressive brain volume loss” by Morgan J. Prust, Kourosh Jafari-Khouzani, Jayashree Kalpathy-Cramer, Pavlina Polaskova, Tracy T. Batchelor, Elizabeth R. Gerstner, and Jorg Dietrich in Neurology. Published online July 24 2015 doi:10.1212/WNL.0000000000001861






