Summary: Ischemic preconditioning may help to prevent stroke, a new study reports. Restricting blood flow by wearing inflatable blood pressure cuffs on the arms and legs allows for more controlled blood flow to the brain.
Source: AAN
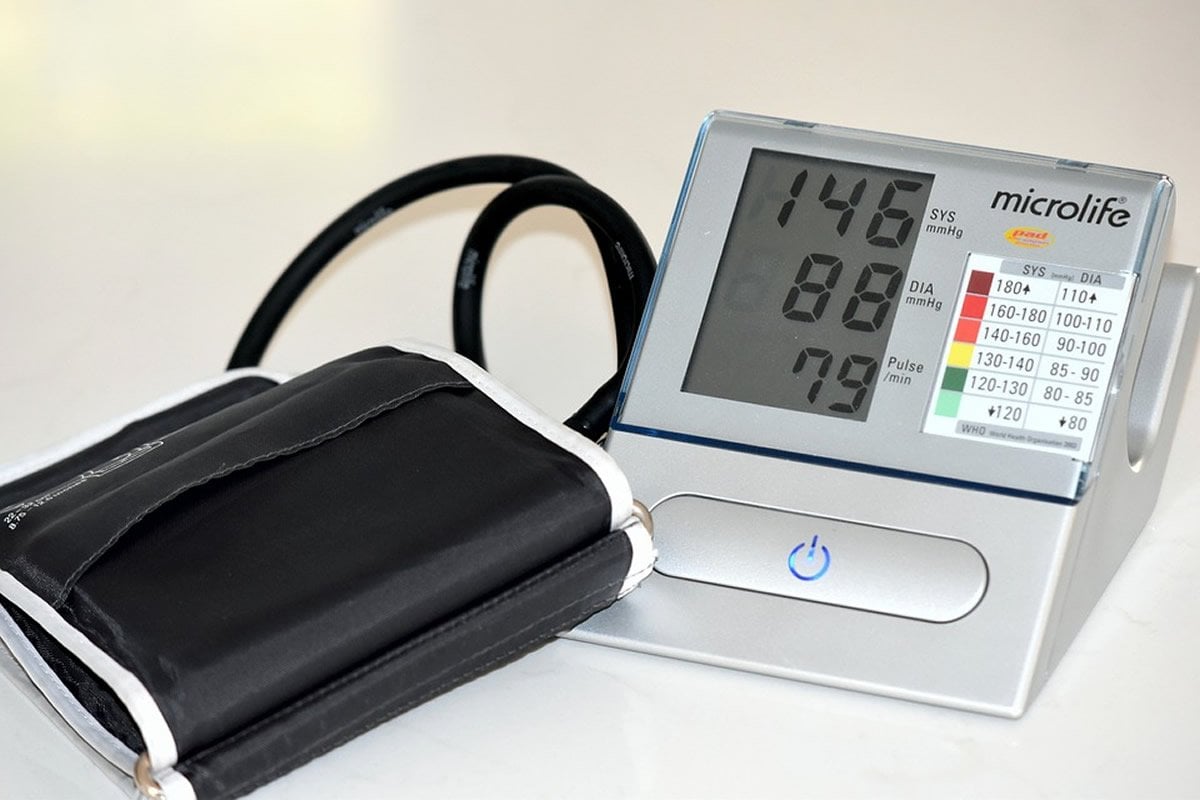
What if wearing a blood pressure cuff could help prevent stroke? In a new study, people who restricted their blood flow by wearing inflated blood pressure cuffs on an arm and leg showed signs of more controlled blood flow to their brain, a process that could be protective if blood flow is more severely restricted in the event of a stroke, according to a study published in the May 29, 2019, online issue of Neurology.
The process is called remote ischemic preconditioning. Previous studies have shown that remote ischemic preconditioning, using compression on the extremities to repeatedly restrict blood flow and the oxygen it carries, is beneficial to internal organs like the heart, making them more resilient and resistant to changes in blood flow and the serious damage that can occur during a heart attack when tissue is first deprived of oxygen and then damaged when oxygen is restored.
“Since previous studies have shown benefits to the heart, we wanted to determine if remote ischemic preconditioning could also be beneficial to the brain,” said study author Yi Yang, MD, PhD, of the First Hospital of Jilin University in Changchun, China. “Our study found such preconditioning temporarily improved dynamic cerebral autoregulation, which is the brain’s ability to regulate and ensure adequate blood flow to the brain despite blood pressure changes. We also found an increase in biomarkers in the blood that can be protective to the nervous system and brain.”
The study involved 50 people with an average age of 35 who were all in good health. Each person was monitored twice, for 24 hours each time, first without preconditioning and then with preconditioning.
Each participant went through the preconditioning process once, with blood pressure cuffs placed on one upper arm and one thigh. The cuffs were inflated for five minutes and then deflated for five minutes. This process to reduce blood flow was repeated four times.
Researchers measured each participant’s brain blood flow regulation by measuring blood pressure and also using ultrasound to measure blood flow within two main arteries in the brain. Measurements were taken at the start of each day and then at six additional time points throughout each 24-hour time period.
They found that after preconditioning, participants had improved brain blood flow regulation starting six hours after preconditioning that was sustained for at least 24 hours.
Researchers also measured biomarkers in the blood one hour after preconditioning and found that after preconditioning, participants had an increase in two biomarkers known to protect the nervous system, as well as an increase in four biomarkers involved in the inflammatory process in the immune system. They also found lower levels of a biomarker that responds to inflammation.
“Our results showed an increase in one biomarker called glial cell line-derived neurotrophic factor that has been previously shown to provide protection not only against diseases such as stroke, but also against other nerve-related diseases like Parkinson’s disease and epilepsy,” said Yang.
“Therefore, our results suggest that remote ischemic preconditioning may increase such protective biomarkers and may be beneficial in preventing a number of neurological diseases.”
Glial cell line-derived neurotrophic factor increased from an average of 0.289 picograms per milliliter (pg/ml) to an average of 0.789 pg/ml one hour after preconditioning.
Yang said, “While our results are exciting, obviously we can’t know when someone will have a stroke and when this could be beneficial. We hope to use these results to help develop a new medication or treatment that will help all people better resist stroke or other neurological diseases. It’s important to emphasize that people should not try to restrict blood flow on their own because, unless, under the care of a physician, they could cause themselves harm. In addition, our study was small and much more research needs to be done to confirm our findings before recommendations can be made to physicians to use such preconditioning as a therapy.”
One limitation of the study is that blood samples were taken only once. Another limitation is that participants were healthy, so the results may be different in people who have risk factors for stroke or other diseases.
Funding: The study was supported by the National Key Research and Development Program of China and the Jilin University Science and Technology Innovative Research Team.
Funding:The research is supported by Innovation Fund Denmark.
Source:
AAN
Media Contacts:
Renee Tessman – AAN
Image Source:
The image is in the public domain.
Original Research: Open access
“Changes in cerebral autoregulation and blood biomarkers after remote ischemic preconditioning”. Zhen-Ni Guo, Wei-Tong Guo, Jia Liu, Junlei Chang, Hongyin Ma, Peng Zhang, Fu-Liang Zhang, Ke Han, Han-Hwa Hu, Hang Jin, Xin Sun, David Martin Simpson, Yi YangM.
Neurology. doi:10.1212/WNL.0000000000007732
Abstract
Changes in cerebral autoregulation and blood biomarkers after remote ischemic preconditioning
Objective
To determine the effect of remote ischemic preconditioning (RIPC) on dynamic cerebral autoregulation (dCA) and various blood biomarkers in healthy adults.
Methods
A self-controlled interventional study was conducted. Serial measurements of dCA were performed at 7 time points (7, 9, and 11 AM; 2, 5, and 8 PM, and 8 AM on the next day) without or with RIPC, carried out at 7:20 to 8 AM. Venous blood samples were collected at baseline (7 AM) and 1 hour after RIPC, and blood biomarkers, including 5 neuroprotective factors and 25 inflammation-related biomarkers, were measured with a quantitative protein chip.
Results
Fifty participants were enrolled (age 34.54 ± 12.01 years, 22 men). Compared with the results on the day without RIPC, dCA was significantly increased at 6 hours after RIPC, and the increase was sustained for at least 24 hours. After RIPC, 2 neuroprotective factors (glial cell-derived neurotrophic factor and vascular endothelial growth factor-A) and 4 inflammation-related biomarkers (transforming growth factor-β1, leukemia inhibitory factor, matrix metallopeptidase-9, and tissue inhibitor of metalloproteinase-1) were significantly elevated compared with their baseline levels. Conversely, monocyte chemoattractant protein-1 was significantly lower compared with its baseline level.
Conclusions
RIPC induces a sustained increase of dCA from 6 to at least 24 hours after treatment in healthy adults. In addition, several neuroprotective and inflammation-related blood biomarkers were differentially regulated shortly after RIPC. The increased dCA and altered blood biomarkers may collectively contribute to the beneficial effects of RIPC on cerebrovascular function.
ClinicalTrials.gov identifier: NCT02965547.






