Summary: Researchers report the retina may provide clues as to those at risk of developing Alzheimer’s disease. A new study reports amyloid plaques have been discovered in peripheral areas of the retina in Alzheimer’s patients. The amount of retinal plaques correlated with the amount of amyoid plaques in specific brain areas.
Source: Cedars Sinai Medical Center.
Cedars-Sinai neuroscience investigators have found that Alzheimer’s disease affects the retina — the back of the eye — similarly to the way it affects the brain. The study also revealed that an investigational, noninvasive eye scan could detect the key signs of Alzheimer’s disease years before patients experience symptoms.
Using a high-definition eye scan developed especially for the study, researchers detected the crucial warning signs of Alzheimer’s disease: amyloid-beta deposits, a buildup of toxic proteins. The findings represent a major advancement toward identifying people at high risk for the debilitating condition years sooner.
The study, published today in JCI Insight, comes amid a sharp rise in the number of people affected by the disease. Today, more than 5 million Americans have Alzheimer’s disease. That number is expected to triple by 2050, according to the Alzheimer’s Association.
“The findings suggest that the retina may serve as a reliable source for Alzheimer’s disease diagnosis,” said the study’s senior lead author, Maya Koronyo-Hamaoui, PhD, a principal investigator and associate professor in the departments of Neurosurgery and Biomedical Sciences at Cedars-Sinai. “One of the major advantages of analyzing the retina is the repeatability, which allows us to monitor patients and potentially the progression of their disease.”
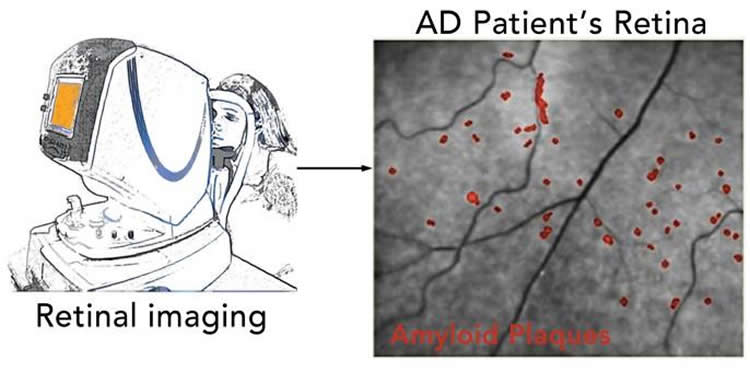
Yosef Koronyo, MSc, a research associate in the Department of Neurosurgery and first author on the study, said another key finding from the new study was the discovery of amyloid plaques in previously overlooked peripheral regions of the retina. He noted that the plaque amount in the retina correlated with plaque amount in specific areas of the brain.
“Now we know exactly where to look to find the signs of Alzheimer’s disease as early as possible,” said Koronyo.
Keith L. Black, MD, chair of Cedars-Sinai’s Department of Neurosurgery and director of the Maxine Dunitz Neurosurgical Institute, who co-led the study, said the findings offer hope for early detection when intervention could be most effective.
“Our hope is that eventually the investigational eye scan will be used as a screening device to detect the disease early enough to intervene and change the course of the disorder with medications and lifestyle changes,” said Black.
For decades, the only way to officially diagnose the debilitating condition was to survey and analyze a patient’s brain after the patient died. In recent years, physicians have relied on positron emission tomography (PET) scans of the brains of living people to provide evidence of the disease but the technology is expensive and invasive, requiring the patient to be injected with radioactive tracers.
In an effort to find a more cost-effective and less invasive technique, the Cedars-Sinai research team collaborated with investigators at NeuroVision Imaging, Commonwealth Scientific and Industrial Research Organisation, University of Southern California, and UCLA to translate their noninvasive eye screening approach to humans.
The published results are based on a clinical trial conducted on 16 Alzheimer’s disease patients who drank a solution that includes curcumin, a natural component of the spice turmeric. The curcumin causes amyloid plaque in the retina to “light up” and be detected by the scan. The patients were then compared to a group of younger, cognitively normal individuals.
Investigators who contributed to the study include David Biggs, Ernesto Barron, David S. Boyer, Joel A. Pearlman, William J. Au, Shawn J. Kile, Austin Blanco, Dieu-Trang Fuchs, Adeel Ashfaq, Sally Frautschy, Gregory M. Cole, Carol A. Miller, David R. Hinton and Steven R. Verdooner.
Funding: The study was funded by the National Institutes of Health/National Institute on Aging, The Marciano Family Foundation and The Saban Family Foundation.
Source: Anasia Obioha – Cedars Sinai Medical Center
Image Source: NeuroscienceNews.com image is credited to Cedars-Sinai.
Original Research: Full open access research for “Retinal amyloid pathology and proof-of-concept imaging trial in Alzheimer’s disease” by Yosef Koronyo, David Biggs, Ernesto Barron, David S. Boyer, Joel A. Pearlman, William J. Au, Shawn J. Kile, Austin Blanco, Dieu-Trang Fuchs, Adeel Ashfaq, Sally Frautschy, Gregory M. Cole, Carol A. Miller, David R. Hinton, Steven R. Verdooner, Keith L. Black, and aya Koronyo-Hamaoui in JCI Insight. Published online August 17 2017 doi:10.1172/jci.insight.93621
[cbtabs][cbtab title=”MLA”]Cedars Sinai Medical Center “Eye Test Could Predict Alzheimer’s Years Before Symptoms Appear.” NeuroscienceNews. NeuroscienceNews, 18 August 2017.
<https://neurosciencenews.com/alzheimers-eye-test-7330/>.[/cbtab][cbtab title=”APA”]Cedars Sinai Medical Center (2017, August 18). Eye Test Could Predict Alzheimer’s Years Before Symptoms Appear. NeuroscienceNew. Retrieved August 18, 2017 from https://neurosciencenews.com/alzheimers-eye-test-7330/[/cbtab][cbtab title=”Chicago”]Cedars Sinai Medical Center “Eye Test Could Predict Alzheimer’s Years Before Symptoms Appear.” https://neurosciencenews.com/alzheimers-eye-test-7330/ (accessed August 18, 2017).[/cbtab][/cbtabs]
Abstract
Retinal amyloid pathology and proof-of-concept imaging trial in Alzheimer’s disease
BACKGROUND. Noninvasive detection of Alzheimer’s disease (AD) with high specificity and sensitivity can greatly facilitate identification of at-risk populations for earlier, more effective intervention. AD patients exhibit a myriad of retinal pathologies, including hallmark amyloid β-protein (Aβ) deposits.
METHODS. Burden, distribution, cellular layer, and structure of retinal Aβ plaques were analyzed in flat mounts and cross sections of definite AD patients and controls (n = 37). In a proof-of-concept retinal imaging trial (n = 16), amyloid probe curcumin formulation was determined and protocol was established for retinal amyloid imaging in live patients.
RESULTS. Histological examination uncovered classical and neuritic-like Aβ deposits with increased retinal Aβ42 plaques (4.7-fold; P = 0.0063) and neuronal loss (P = 0.0023) in AD patients versus matched controls. Retinal Aβ plaque mirrored brain pathology, especially in the primary visual cortex (P = 0.0097 to P = 0.0018; Pearson’s r = 0.84–0.91). Retinal deposits often associated with blood vessels and occurred in hot spot peripheral regions of the superior quadrant and innermost retinal layers. Transmission electron microscopy revealed retinal Aβ assembled into protofibrils and fibrils. Moreover, the ability to image retinal amyloid deposits with solid-lipid curcumin and a modified scanning laser ophthalmoscope was demonstrated in live patients. A fully automated calculation of the retinal amyloid index (RAI), a quantitative measure of increased curcumin fluorescence, was constructed. Analysis of RAI scores showed a 2.1-fold increase in AD patients versus controls (P = 0.0031).
CONCLUSION. The geometric distribution and increased burden of retinal amyloid pathology in AD, together with the feasibility to noninvasively detect discrete retinal amyloid deposits in living patients, may lead to a practical approach for large-scale AD diagnosis and monitoring.
FUNDING. National Institute on Aging award (AG044897) and The Saban and The Marciano Family Foundations.
“Retinal amyloid pathology and proof-of-concept imaging trial in Alzheimer’s disease” by Yosef Koronyo, David Biggs, Ernesto Barron, David S. Boyer, Joel A. Pearlman, William J. Au, Shawn J. Kile, Austin Blanco, Dieu-Trang Fuchs, Adeel Ashfaq, Sally Frautschy, Gregory M. Cole, Carol A. Miller, David R. Hinton, Steven R. Verdooner, Keith L. Black, and aya Koronyo-Hamaoui in JCI Insight. Published online August 17 2017 doi:10.1172/jci.insight.93621