Summary: Microscopic alterations in white matter may affect how patients with neurological conditions respond to non-invasive electrical brain stimulation.
Source: Imperial College London
Tiny changes in the microscopic structure of the human brain may affect how patients respond to an emerging therapy for neurological problems.
The technique, called non-invasive electrical brain stimulation, involves applying an electrical current to the surface of a patient’s head to stimulate brain cells, altering the patient’s brain activity. It is being trialled for a range of neurological problems including recovery from stroke, traumatic brain injury, dementia, and depression, but research to date has found the effects to be inconsistent
Now, a team led by researchers at Imperial College London has shed more light on why these inconsistencies occur and may provide physical evidence for why some patients respond better than others – because of the fine structure of their brain tissue. The new research suggests it may be possible to target the therapy to those patients most likely to benefit.
They found that differences in the makeup of the brain’s white matter – the tissue deep in the brain and rich in the branching ‘tails’ of nerve cells – were key. The research revealed that those who had more connectivity in the regions being stimulated were more likely to respond better to the treatment.
According to the team, the findings, published in the journal Brain, could help to personalise the non-invasive electrical brain stimulation, targeting the treatment to patients who are most likely to gain clinical benefits.
Dr Lucia Li, a clinical lecturer in neurology in the Department of Brain Sciences at Imperial College London, and lead author of the study, said: “With all the current buzz around brain stimulation for altering brain activity, it’s important to understand who will benefit most from this technique in the clinic.
“Problems with white matter structure are a feature of a range of different neurological conditions. Our study is a step towards more personalised use of brain stimulation, which will improve the outcomes using this technique, as well as reduce the number of people treated un-necessarily.”
In the study, researchers looked at 24 healthy patients and 35 patients recovering from a moderate or severe traumatic brain injury (TBI). Participants performed a task inside an MRI scanner (see ‘The Stop Signal Task’ in notes to editors) while receiving small amounts of electrical current through electrodes on the surface of the scalp or a placebo. They were unable to tell whether they were receiving brain stimulation or not.
They found that healthy participants who received brain stimulation performed better in the task than when they didn’t receive the treatment. For patient with TBI, task performance in response to stimulation varied widely.
However, when they analysed MRI scans, they found that those participants with highly-connected white matter in the brain region being stimulated responded best to the treatment, and those who had damaged or less-connected regions of white matter showed less improvement.
They also found that brain stimulation could partially reverse some of the abnormalities in brain activity caused by TBI.
The team cautions that while more work is needed to confirm the findings, it could mean brain stimulation might prove a useful treatment approach for other neurological conditions with abnormal brain activity as a feature, such as dementia.
“We found that people with stronger white matter connections in their brain had better improvement with stimulation,” Dr Li explained.
“This might be an important reason why previous studies have found that some people benefit from stimulation, whilst others don’t and means we can start using brain stimulation in a more personalised way.”
According to the researchers, the study is limited in that in that they only investigated one type of cognitive behaviour and would need to be replicated in other types of behaviour to show if the findings apply more generally. In addition, they only stimulated one region of the brain, so they don’t know whether the effects are specific to this region, or whether other regions can be stimulated.
Dr Li explains the team will now focus on larger studies with more participants to investigate what other factors influence someone’s response to brain stimulation. They will also apply the technique to other conditions with abnormalities in brain activity to see if they can alter activity and improve brain function.
Funding: The work was supported by the Wellcome Trust and the National Institute for Health Research. Patients were predominantly recruited from St Mary’s Hospital (Imperial College Healthcare NHS Trust) and imaged at the Imperial College Clinical Imaging Facility.
Source:
Imperial College London
Media Contacts:
Ryan O’Hare – Imperial College London
Image Source:
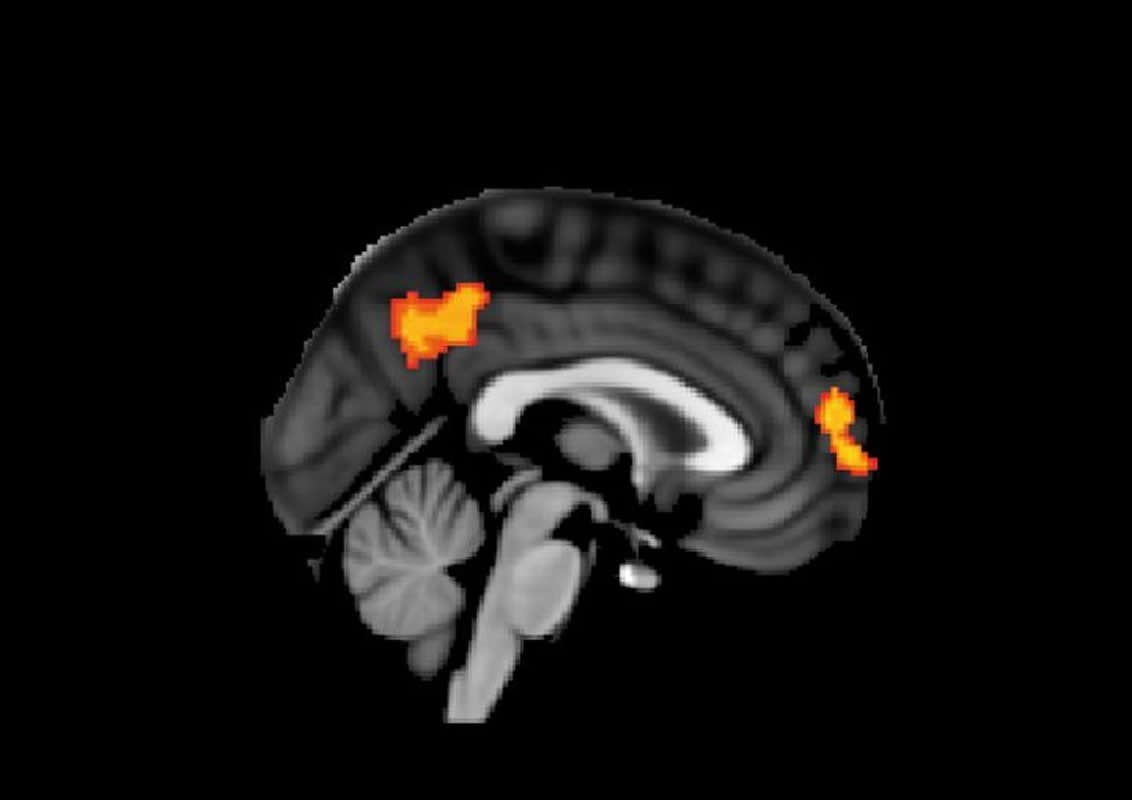
The image is credited to Lucia Li et al.
Original Research: Open access
“Traumatic axonal injury influences the cognitive effect of non-invasive brain stimulation”. Lucia Li et al.
Brain. doi:10.1093/brain/awz252
Abstract
Traumatic axonal injury influences the cognitive effect of non-invasive brain stimulation
Non-invasive brain stimulation has been widely investigated as a potential treatment for a range of neurological and psychiatric conditions, including brain injury. However, the behavioural effects of brain stimulation are variable, for reasons that are poorly understood. This is a particular challenge for traumatic brain injury, where patterns of damage and their clinical effects are heterogeneous. Here we test the hypothesis that the response to transcranial direct current stimulation following traumatic brain injury is dependent on white matter damage within the stimulated network. We used a novel simultaneous stimulation-MRI protocol applying anodal, cathodal and sham stimulation to 24 healthy control subjects and 35 patients with moderate/severe traumatic brain injury. Stimulation was applied to the right inferior frontal gyrus/anterior insula node of the salience network, which was targeted because our previous work had shown its importance to executive function. Stimulation was applied during performance of the Stop Signal Task, which assesses response inhibition, a key component of executive function. Structural MRI was used to assess the extent of brain injury, including diffusion MRI assessment of post-traumatic axonal injury. Functional MRI, which was simultaneously acquired to delivery of stimulation, assessed the effects of stimulation on cognitive network function. Anodal stimulation improved response inhibition in control participants, an effect that was not observed in the patient group. The extent of traumatic axonal injury within the salience network strongly influenced the behavioural response to stimulation. Increasing damage to the tract connecting the stimulated right inferior frontal gyrus/anterior insula to the rest of the salience network was associated with reduced beneficial effects of stimulation. In addition, anodal stimulation normalized default mode network activation in patients with poor response inhibition, suggesting that stimulation modulates communication between the networks involved in supporting cognitive control. These results demonstrate an important principle: that white matter structure of the connections within a stimulated brain network influences the behavioural response to stimulation. This suggests that a personalized approach to non-invasive brain stimulation is likely to be necessary, with structural integrity of the targeted brain networks an important criterion for patient selection and an individualized approach to the selection of stimulation parameters.