Cancer Research UK scientists have developed a technique they believe could be used to detect tiny secondary tumors in the brain, a process that is currently impossible, according to research published in PNAS, Monday.
The scientists at Cancer Research UK’s Gray Institute for Radiation Oncology and Biology at the University of Oxford showed that a special dye recognises and sticks to a molecule called VCAM-1, in mice. The molecule is produced in greater amounts on blood vessels in cancer that has spread to the brain from other parts of the body – known as brain metastases.
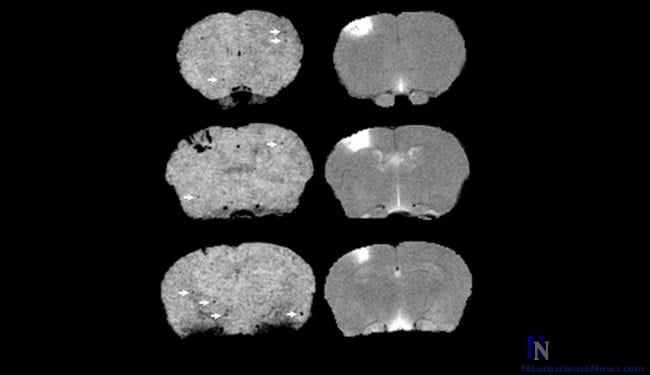
A medical imaging technique called magnetic resonance imaging (MRI) can ‘take a photo’ of the dye distribution in the brain. This could enable cancer doctors to detect brain metastases that are much smaller than is currently possible.
Secondary cancer that has spread to the brain is extremely difficult to treat successfully. Approximately 10 per cent of patients with cancer develop brain metastases.
Small secondary brain tumours can be treated with whole brain radiotherapy or surgery, and there are new chemotherapy treatments in development. But currently, it is only possible to detect larger secondary brain tumours, which are more difficult to treat.
Cancer Research UK scientist, Dr Nicola Sibson, from the Gray Institute, said: “We urgently need to find ways to diagnose these cancers at an earlier stage to improve survival rates.
“Our research suggests a new possible approach to do just this. The next stage is to build on these results and carry out clinical trials. If successful, we hope that early detection using this technique could increase the number of available treatment options for these patients.”
Dr Julie Sharp, Cancer Research UK’s senior science information manager, said:
“This exciting discovery reveals that a single protein could enable doctors to literally paint a picture with a medical dye to detect cancer that has spread to the brain, at a very early stage, when treatment has a greater chance of being successful.
“Thanks to the generosity of the public we’ve invested in research that has contributed to progress in brain tumour treatment, with survival almost doubling in children since the 1960s. But sadly less progress has been made in adults – a situation that urgently needs to change. We hope that research such as this to improve detection will increase survival from this hard-to-treat disease.”
Notes about this brain research article
Contact: Cancer Research UK press office
Source: Cancer Research UK press release
Image Source: Neuroscience News image adapted from PNAS research image by Seres et al
Original Research: Abstract for “Molecular MRI enables early and sensitive detection of brain metastases” by Seres et al. in PNAS (2012)