Summary: Does your brain stop “listening” to your lungs when you fall into a deep sleep? According to a new study, the answer is yes. Researchers discovered that during the deepest stages of non-REM sleep (characterized by slow delta waves), the brain’s activity becomes increasingly independent of the rhythm of breathing.
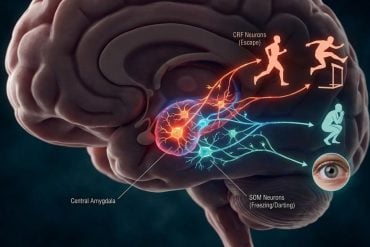
By focusing on the substantia nigra—a deep-brain region that produces dopamine and controls movement—scientists found that the usual “coupling” between breath and brain waves seen during wakefulness and lighter sleep essentially dissolves during deep rest. This discovery offers vital clues into the mechanics of anesthesia and could lead to new treatments for Parkinson’s disease, where both sleep and breathing are often severely disrupted.
Key Facts
- The “Disconnect”: While brain waves and breathing patterns are usually synchronized during quiet wakefulness and light sleep, they become mostly independent during the “slow delta” activity of the deepest non-REM sleep.
- Focus on the Substantia Nigra: This is the first study to detail how breathing affects this critical deep-brain region, which is responsible for dopamine production and motor control.
- Parkinson’s Link: Because the substantia nigra is the primary area damaged in Parkinson’s disease, understanding its “rhythm” during sleep could explain why Parkinson’s patients suffer from both sleep apnea and insomnia.
- Anesthesia Insights: The study also compared sleep states to ketamine anesthesia, finding that different states of “unconsciousness” have unique ways of linking (or unlinking) the brain to peripheral rhythms like breathing.
- The Primary Motor Cortex: In addition to the deep brain, researchers tracked the motor cortex, showing that this “breath-brain decoupling” is a widespread phenomenon during deep restorative sleep.
Source: HMH
Could the deepest parts of the brain hold some of the secrets of sleep that still remain elusive to science?
A team from Hackensack Meridian Health and its Center for Discovery and Innovation (CDI) have produced a new in-depth study penetrating into the brain, finding that during the deepest sleep, breathing patterns and brain activity become more independent from one another – unlike lighter sleep or quiet wakefulness.

The study was published in The Journal of Neuroscience in January, with the team led by CDI author Bon-Mi Gu, Ph.D., also of the Hackensack Meridian School of Medicine. The research team includes Kolsoum Dehdar, Ph.D., and Elliot Neuberg, and recently relocated from the Neuroscience Institute at Hackensack Meridian JFK University Medical Center to the CDI.
The paper focuses on the basal ganglia, clusters of neurons responsible for motor control and other roles. Of prime interest to the scientists is the tiny region called the substantia nigra, which controls movements and produces dopamine, among other functions.
The relation between these structures and sleep – and how they relate to each other’s rhythm has not heretofore been widely studied, according to the scientists.
“In this study, we provide the first detailed characterization of respiration-neural coupling across multiple states – including quiet wakefulness, non-REM sleep, REM sleep, and anesthesia – in the substantia nigra and the primary motor cortex, two regions not previously studied in this context,” write the authors.
The team measured the sleep cycles of mice, comparing electrical brain activity and breathing and how the two timed off one another. They also assessed the mice during wakefulness, as well as under ketamine anesthesia.
The scientists found nuances and variations in all states. But one consistent thread was that the deepest non-REM sleep had breathing mostly independent of the brain waves, especially with the “slow delta” activity during the deepest part of slumber.
“The strength of respiration-neural coupling varied across multiple states, including NREM sleep, REM sleep, quiet wakefulness, and anesthesia, and was directly related to the delta power, a hallmark of NREM sleep,” write the authors.
The conclusions could pave the way into better understanding of how sleep works – and could help with some disease states, they find.
“These findings provide new insights into how internal brain states interact with peripheral rhythms like respiration, with important functional implications for both sleep and anesthesia,” write the scientists.
“Furthermore,” they add, “elucidating the mechanisms underlying respiration-neural coupling, especially within basal ganglia circuits, will shed light on the pathophysiology of conditions such as Parkinson’s disease, where both sleep and respiration are commonly disrupted.”
Key Questions Answered:
A: Not at all—it’s actually a hallmark of restorative sleep. During wakefulness, your brain is highly responsive to the world (and your own body). In deep sleep, the brain essentially “closes the curtains” to focus on internal maintenance and memory consolidation, allowing its waves to flow independently of your physical breathing rhythm.
A: This region is the brain’s “dopamine factory.” We already know it’s vital for movement, but we didn’t know how it behaved during sleep. If this region fails to “decouple” or “sync up” correctly, it might be the reason why people with Parkinson’s experience such restless, low-quality sleep.
A: Yes. By understanding how breathing and brain waves interact under anesthesia versus natural sleep, doctors can develop more precise ways to monitor patients, ensuring they stay at the perfect level of unconsciousness without disrupting their vital rhythms.
Editorial Notes:
- This article was edited by a Neuroscience News editor.
- Journal paper reviewed in full.
- Additional context added by our staff.
About this sleep and neuroscience research news
Author: Seth Augenstein
Source: HMH
Contact: Seth Augenstein – HMH
Image: The image is credited to Neuroscience News
Original Research: Closed access.
“Dynamic Respiration–Neural Coupling in Substantia Nigra across Sleep and Anesthesia” by Kolsoum Dehdar, Elliot Neuberg and Bon-Mi Gu. Journal of Neuroscience
DOI:10.1523/JNEUROSCI.1154-25.2025
Abstract
Dynamic Respiration–Neural Coupling in Substantia Nigra across Sleep and Anesthesia
Respiration is increasingly recognized as a coordinator of neural activity across widespread brain regions and behavioral states. Even during sleep, respiration rhythms modulate sleep-related oscillations. While the basal ganglia are known to play roles in both sleep and respiratory regulation, their interaction with respiration rhythms remains poorly understood.
Here, we examined respiration–neural couplings in the substantia nigra pars reticulata (SNr), a major output nucleus of the basal ganglia, and the primary motor cortex (M1) across multiple states in male and female mice, including non-rapid eye movement (NREM) sleep, rapid eye movement (REM) sleep, quiet wakefulness, and anesthesia.
Simultaneous recordings of local field potentials (LFPs) from M1 and SNr along with diaphragm muscle activities revealed state-dependent, region-specific patterns of respiration–neural coupling.
Coupling strength in both SNr and M1 was attenuated during NREM sleep compared with REM sleep and quiet wakefulness. However, under ketamine/xylazine anesthesia, coupling was markedly enhanced in the SNr, but not in M1, indicating region-specific sensitivity to arousal and anesthesia state.
Notably, respiration–neural coupling was systematically related to delta sub-band power; coupling strength was reduced with increased slow delta (0.5–2 Hz) and decreased fast delta (2.5–4 Hz) powers.
In addition, slow delta was associated with SNr-M1 synchronization, suggesting that interregional communication during deep sleep may suppress respiration locking.
Together, these findings highlight dynamic, state-dependent modulation of respiration–neural couplings in corticobasal ganglia circuits, underscoring its potential role in coordinating body–brain interactions during sleep and anesthesia.