Scientists from King’s College London and the University of Roehampton have identified a key mechanism in the brain which might be associated with the onset and development of psychosis.
Using a Magnetic Resonance Imaging (MRI) technique they found that 52 young people deemed to be at ultra high risk of psychosis had increased or ‘hyperactive’levels of blood flow compared to 27 healthy controls in the hippocampus, striatum and midbrain – all brain regions that are particularly implicated in the onset of psychotic disorders like schizophrenia.
This study is one of the first in humans to confirm results from animal research, which has already shown that increased activity in these brain regions drives the development of psychosis.
In the study, published today in the American Journal of Psychiatry and funded by the Medical Research Council, the researchers also repeated the MRI scans after 18 months to examine how blood flow levels had changed. In participants whose presenting symptoms had resolved, the researchers found that resting blood flow levels in the hippocampus had decreased to the levels seen in healthy participants. This suggests that normalisation of blood flow in the hippocampus may underlie clinical improvement in these participants.
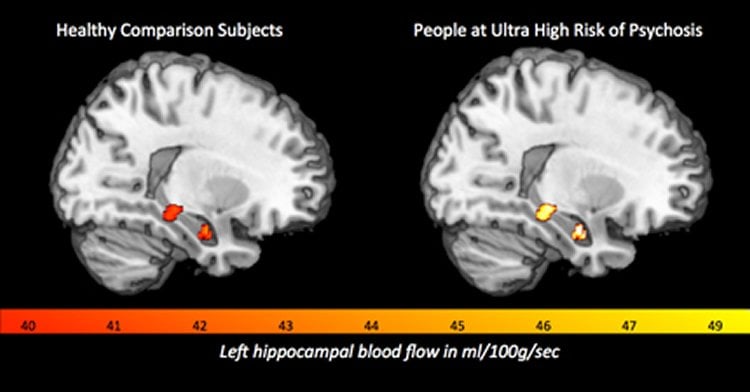
Professor Paul Allen from the Institute of Psychiatry, Psychology & Neuroscience (IoPPN) at King’s College London and the University of Roehampton said: ‘Our research identified significant differences in brain blood flow between healthy people and those at ultra high risk of psychosis. These differences help us understand the neurobiological mechanisms that underlie the development of psychosis.’
Professor Philip McGuire, also from the IoPPN at King’s College London, added: ‘These findings are also important in terms of clinical practice. They underline the potential of brain scanning to help clinicians predict whether people who are at increased risk of psychosis will go on to develop a disorder or whether they will recover.
‘In addition, understanding what is happening in the brain at this stage also informs the ongoing development of new treatments designed to prevent the development of psychotic disorders.’
Source: Jack Stonebridge – King’s College London
Image Source: The image is credited to the researchers
Original Research: Abstract for “Resting Hyperperfusion of the Hippocampus, Midbrain, and Basal Ganglia in People at High Risk for Psychosis” by Paul Allen, Ph.D. Christopher A. Chaddock, Ph.D. Alice Egerton, Ph.D. Oliver D. Howes, M.D., Ph.D. Ilaria Bonoldi, M.D. Fernando Zelaya, Ph.D. Sagnik Bhattacharyya, M.D., Ph.D. Robin Murray, M.D. Philip McGuire, M.D., Ph.D. in American Journal of Psychiatry. Published online December 16 2015 doi:10.1176/appi.ajp.2015.15040485
Abstract
Resting Hyperperfusion of the Hippocampus, Midbrain, and Basal Ganglia in People at High Risk for Psychosis
Objective:
Animal models suggest that the development of psychosis involves hyperactivity in the hippocampus that drives increased activity in the midbrain and basal ganglia. The authors examined this hypothesis by measuring resting perfusion in the hippocampus, basal ganglia, and midbrain in people at high risk of psychosis.
Method:
Pseudo-continuous arterial spin labeling imaging was used to measure resting regional cerebral blood flow (rCBF) in 52 individuals at ultra-high risk for psychosis and in 27 healthy volunteers. The severity of psychotic symptoms was assessed using the Comprehensive Assessment of At-Risk Mental States. The ultra-high-risk subjects were reassessed after a mean of 17 months, using the same measures as at baseline.
Results:
At baseline, relative to healthy volunteers, ultra-high-risk subjects showed elevated rCBF in the hippocampus, basal ganglia, and midbrain. In the ultra-high-risk sample overall, at follow-up, symptomatic improvement and reduced rCBF in the hippocampus and ventral striatum were observed. Subjects whose symptoms had resolved such that they no longer met ultra-high-risk criteria showed a longitudinal reduction in left hippocampal rCBF that was not evident in subjects who remained in a high-risk state or had become psychotic.
Conclusions:
A high risk for psychosis was associated with increased resting activity in the hippocampus, midbrain, and basal ganglia. Subsequent resolution of the high-risk state was linked to a normalization of activity in these regions. These findings are consistent with animal models that propose that psychotic symptoms may be generated when hippocampal hyperactivity drives hyperactivity in regions involved in subcortical dopamine signaling.
“Resting Hyperperfusion of the Hippocampus, Midbrain, and Basal Ganglia in People at High Risk for Psychosis” by Paul Allen, Ph.D. Christopher A. Chaddock, Ph.D. Alice Egerton, Ph.D. Oliver D. Howes, M.D., Ph.D. Ilaria Bonoldi, M.D. Fernando Zelaya, Ph.D. Sagnik Bhattacharyya, M.D., Ph.D. Robin Murray, M.D. Philip McGuire, M.D., Ph.D. in American Journal of Psychiatry. Published online December 16 2015 doi:10.1176/appi.ajp.2015.15040485







