Summary: A new study reports amputees often feel as though their prosthetic limb is part of their body.
Source: EPFL.
The famous idiom “seeing is believing” is not enough to help amputees with the use of their prosthetic limb. Many amputees opt out of prolonged use of their prosthetic limb because their missing limb simply does not fit their prosthesis. In other words, their own perception of the missing limb, or the brain’s representation of it, does not match-up with what they see of the prosthesis.
The underlying problem is twofold. Amputees still feel their missing limb, even if it is physically gone, and this ghost limb aka phantom limb is perceived as much smaller that the lost limb. Next, the commercially available prosthetic limb does not yet provide sensory feedback other than what the patient sees, meaning that the patient has no sense of touch from the prosthetic limb and must constantly watch it for correct use.
Tricking the brain to embody the prosthetic limb
Now, in a scientific collaboration led by EPFL (Ecole polytechnique fédérale de Lausanne), scientists show that amputees can actually be convinced that the prosthetic hand belongs to their own body. They do this by going beyond the “seeing is believing” idiom based on established research on how the brain identifies what belongs to its own body. Instead of using the sense of sight alone, they used an astute combination of two senses: sight and touch. The results are published today in the Journal of Neurology, Neurosurgery & Psychiatry.
“The brain regularly uses its senses to evaluate what belongs to the body and what is external to the body. We showed exactly how vision and touch can be combined to trick the amputee’s brain into feeling what it sees, inducing embodiment of the prosthetic hand with an additional effect that the phantom limb grows into the prosthetic one,” explains Giulio Rognini of EPFL’s Laboratory of Cognitive Neuroprosthetics led by Olaf Blanke, in a collaboration with Silvestro Micera of EPFL and Scuola Superiore Sant’Anna in Italy. “The setup is portable and could one day be turned into a therapy to help patients embody their prosthetic limb permanently.”
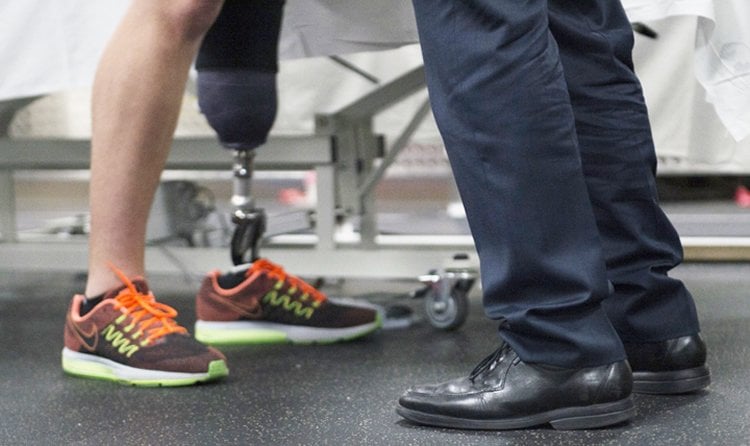
In two hand amputees, the scientists provided artificial tactile sensations at the tip of the index finger – of the phantom limb – by stimulating the patient’s nerve in the stump. At the same time, the patient wore virtual reality goggles which showed the index finger of the prosthetic limb glowing in synchrony with the administered touch sensations. This combination of virtual reality with artificial tactile sensations takes the rubber-hand illusion to another level.
Both patients reported feeling as though the prosthetic hand belonged to their own body. Moreover, when asked to evaluate the position of their hands, both patients felt as though their phantom limb had extended into the prosthetic limb. Previous to the experiment, they both reported that the phantom hand was small and directly connected to the stump, as if the phantom limb had no forearm, a change in size referred to as “telescoping” in scientific jargon. In fact, their phantom limb extended during the experiment, and remained extended for up to 10 minutes afterwards.
The experiment simply requires the patient to passively observe two sensations on the fingertip, the visual glow and the artificial touch happening in synchrony, in order for embodiment and extension of the phantom limb to take place. This is the first time that the principles of multisensory integration, in particular how the brain integrates bodily multisensory information to create the coherent and compelling experience of having a body, have been tailored to provoke embodiment of the prosthetic hand and reduction of telescoping.
Building upon results from a European-wide collaboration
The study builds upon research that opened new avenues is prosthetics. In 2014, in a European collaboration led by EPFL, scientists overcame a major hurdle by giving an amputee the ability to feel – in real-time – with the help of their prosthetic hand. Information about touch coming from sensors at the prosthetic fingertips were directly processed and relayed into the nervous system via electrodes that were surgically wired to the stump’s main nerves. The potential of this technology is still being explored, and two years later in 2016, the scientists showed that the enhanced prosthetic technology could even help the same amputee detect differences in texture.
Source: Hillary Sanctuary – EPFL
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Air Force photo by Master Sgt. Adrian Cadiz.
Original Research: Abstract for “Multisensory bionic limb to achieve prosthesis embodiment and reduce distorted phantom limb perceptions” by Giulio Rognini, Francesco Maria Petrini, Stanisa Raspopovic, Giacomo Valle, Giuseppe Granata, Ivo Strauss, Marco Solcà1,2, Javier Bello-Ruiz, Bruno Herbelin, Robin Mange, Edoardo D’Anna, Riccardo Di Iorio, Giovanni Di Pino, David Andreu, David Guiraud, Thomas Stieglitz, Paolo Maria Rossini, Andrea Serino, Silvestro Micera, and Olaf Blanke in Journal of Neurology Neurosurgery & Psychiatry Published August 2018.
doi:10.1136/jnnp-2018-318570
[cbtabs][cbtab title=”MLA”]EPFL”Amputees Feel as Though Their Prosthetic Limb Belongs to Their Own Body.” NeuroscienceNews. NeuroscienceNews, 13 August 2018.
<https://neurosciencenews.com/prosthetic-body-mapping-9694/>.[/cbtab][cbtab title=”APA”]EPFL(2018, August 13). Amputees Feel as Though Their Prosthetic Limb Belongs to Their Own Body. NeuroscienceNews. Retrieved August 13, 2018 from https://neurosciencenews.com/prosthetic-body-mapping-9694/[/cbtab][cbtab title=”Chicago”]EPFL”Amputees Feel as Though Their Prosthetic Limb Belongs to Their Own Body.” https://neurosciencenews.com/prosthetic-body-mapping-9694/ (accessed August 13, 2018).[/cbtab][/cbtabs]
Abstract
Multisensory bionic limb to achieve prosthesis embodiment and reduce distorted phantom limb perceptions
Introduction
A major goal of neuroprosthetics is to design artificial limbs that are experienced (‘embodied’) like real limbs. However, despite important technological advances, this goal has not been reached and prosthesis embodiment is still very limited. Differently from our physical body, current bionic limbs do not provide the continuous multisensory feedback required for a limb to be experienced as one’s own. Here, we present a novel neuroprosthetic approach that combines peripheral neurotactile stimulation—inducing tactile sensation on the missing limb—and immersive digital technology—providing visual illumination of the prosthetic hand. We tested whether coherent multisensory visuo-tactile neural stimulation (VTNS)1 induced higher prosthesis embodiment and reduced the distorted perception of the phantom limb (telescoping, ie, the phantom limb is perceived as shorter than the intact limb).
Methods
Patient 1 and patient 2 are transradial left forearm chronic amputees, who suffered upper limb telescoping. Patients were implanted with transverse intrafascicular multichannel electrodes (TIMEs), which induced the sensation of a vibration in a circumscribed skin region of the finger 2 via medial nerve stimulation in patient 1 (online supplementary figure 1A) and in a skin region of finger 5 via ulnar nerve stimulation in patient 2 (online supplementary figure 1B and material 1). Neurotactile stimulation2 was coupled with automatised visual illumination of a skin region on the patient’s prosthetic hand that corresponded to the somatotopic location of touch sensations experienced on the phantom hand (VTNS; online supplementary video 1, online supplementary figure 1, online supplementary material 1). VTNS was administered in two conditions, either with synchronous visual and neurotactile stimulation or in a control condition of asynchronous stimulation (1.5–2.5s delay).






