Summary: Researchers have developed a new, sophisticated device that delivers vagus nerve stimulation to help treat chronic pain.
Source: Vienna University of Technology
The vagus nerve plays an important role in our body. It consists of various fibres, some of which connect to the internal organs, but the vagus nerve can also be found in the ear. It is of great importance for various body functions, including the perception of pain. Therefore, a lot of research has been focussing on how the vagus nerve can be stimulated effectively and gently with special electrodes.
An important step forward has now been achieved through a cooperation between the TU Wien (Vienna) and MedUni Vienna: the microanatomy of the vagus nerve branches in the human ear, in relation to auricular blood vessels, has been studied with a precision on a micrometer scale. Then a 3D computer model was created to calculate the optimal stimulation of nerve branches using tiny needle-shaped electrodes. These results were then tested on patients. This way, a novel stimulation pattern could be determined, which stimulates the vagus nerve in the ear particularly well.
Tiny electrodes directly on the ear
The team of the electrical engineer Prof. Eugenijus Kaniusas (Institute for Microwave and Circuit Engineering, TU Wien) in cooperation with the Medical University of Vienna has already conducted several studies in which chronic pain or even peripheral circulatory disorders were treated with electrical stimulation of the vagus nerve in the ear. In this process, small electrodes are inserted directly into the ear, which then – controlled by a small portable device worn on the neck – create specific electrical pulses.
A major challenge, however, is to attach the electrodes in exactly the right place. “It is important not to hit any blood vessels, and the electrodes have to be placed at exactly the right distance from the nerve,” explains Eugenijus Kaniusas. “If the electrode is too far away, the nerve is not stimulated at all. If it is too close, the signal is too strong, leading to blockage of the nerve. The nerve can become ‘tired’ over time and eventually stop sending signals to the brain.”
Until now, medical doctors had to rely on experience when positioning the electrodes in the ear. Now, for the first time, a microanatomical study has been carried out to investigate in great detail spatial arrangements of the nerve fibres and blood vessels in the ear. For this purpose, sectional images of tissue samples were photographed in high resolution and then combined into a three-dimensional model on the computer by Babak Dabiri Razlighi, a researcher in Eugenijus Kaniusas’ team.
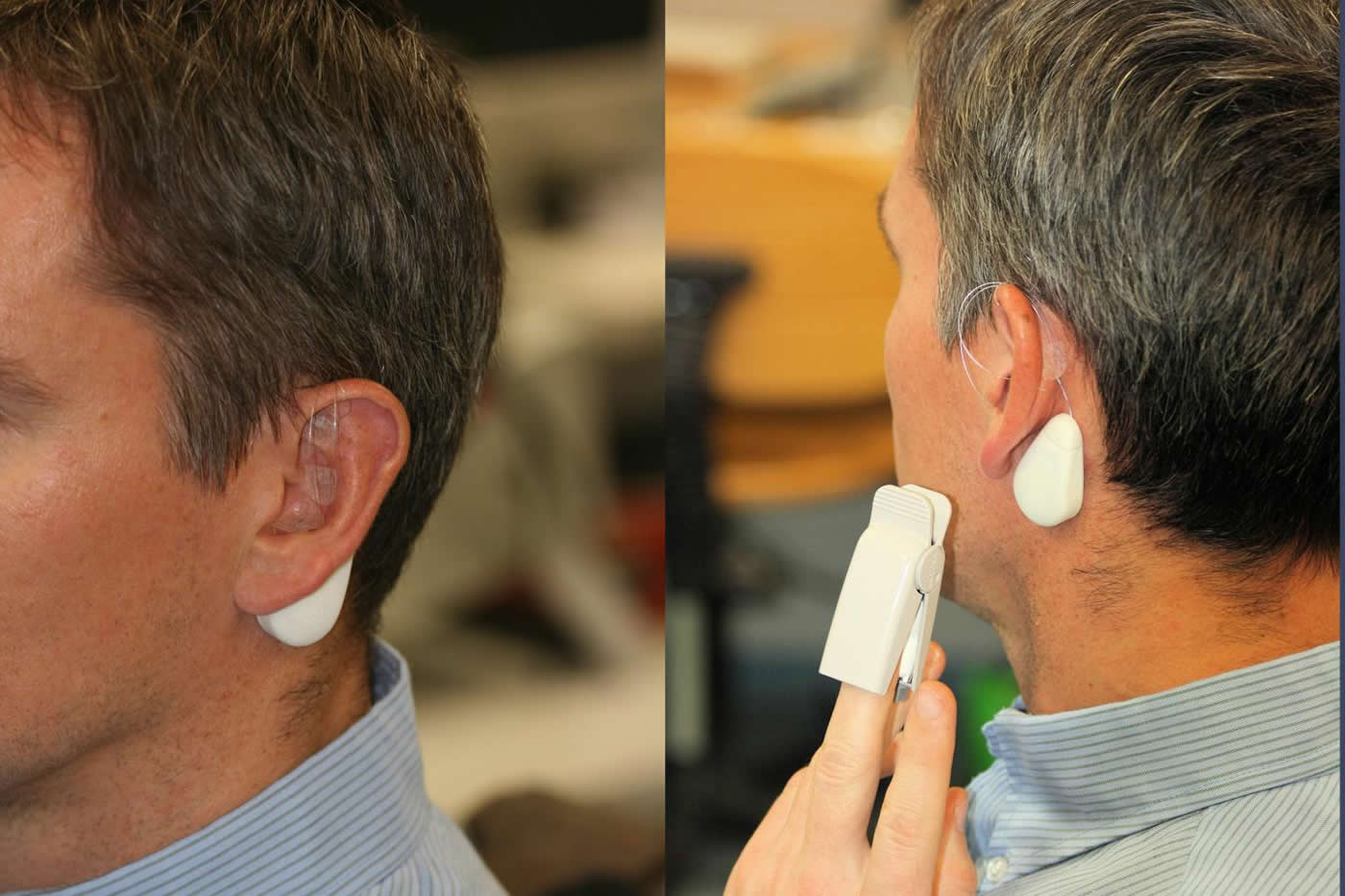
“The blood vessels can be made clearly visible in patients by shining light through the ear”, says Prof. Wolfgang J. Weninger from MedUni Vienna. “The nerves, however, cannot be seen. Our microanatomical measurements on donated human bodies now tell us exactly where the nerves run in relation to blood vessels, as well as the average distance between blood vessels and nerves at certain important positions of the ear. This helps us to find the correct spot for placing the stimulation electrodes.”
Three-phase signal for optimal stimulation
The computer model can also be used to calculate which electrical signals should be used. Not only the strength of the signal is important, but also its shape: “In our computer simulation, it was shown for the first time that from a biophysical point of view, a triphasic signal pattern should be helpful, similar to what is known from power engineering – only with much lower magnitude,” reports Kaniusas. “Three different electrodes each deliver oscillating electrical pulses, but these pulses are not in synch, there needs to be a specific time delay.”
This type of stimulation was tested on people suffering from chronic pain – and the experiments showed that indeed the triphasic stimulation pattern is particularly effective.
“Vagus nerve stimulation is a promising technique, the effect of which has been validated with our new findings and is now being further improved,” says Eugenijus Kaniusas. “Vagus nerve stimulation is often a lifesaving option, especially for people with chronic pain who have already been treated with other methods and do not respond to medication anymore.
About this neuroscience research article
Source:
Vienna University of Technology
Media Contacts:
Eugenijus Kaniusas – Vienna University of Technology
Image Source:
The image is credited to TU Wien.
Original Research: Open access
“High-Resolution Episcopic Imaging for Visualization of Dermal Arteries and Nerves of the Auricular Cymba Conchae in Humans”. by Eugenijus Kaniusas et al.
Frontiers in Neuroanatomy doi:10.3389/fnana.2020.00022
Abstract
High-Resolution Episcopic Imaging for Visualization of Dermal Arteries and Nerves of the Auricular Cymba Conchae in Humans
Therapeutic applications of auricular vagus nerve stimulation (VNS) have drawn recent attention. Since the targeted stimulation process and parameters depend on the electrode–tissue interaction, the lack of structural anatomical information on innervation and vascularization of the auricle restrain the current optimization of stimulation paradigms. For the first time, we employed high-resolution episcopic imaging (HREM) to generate histologic volume data from donated human cadaver ears. Optimal parameters for specimen preparation were evaluated. Anatomical 3D vascular and nerve structures were reconstructed in one sample of an auricular cymba conchae (CC). The feasibility of HREM to visualize anatomical structures was assessed in that diameters, occupied areas, volumes, and mutual distances between auricular arteries, nerves, and veins were registered. The selected region of CC (3 × 5.5 mm) showed in its cross-sections 21.7 ± 2.7 (mean ± standard deviation) arteries and 14.66 ± 2.74 nerve fibers. Identified nerve diameters were 33.66 ± 21.71 μm, and arteries had diameters in the range of 71.58 ± 80.70 μm. The respective occupied area showed a share of, on average, 2.71% and 0.3% for arteries and nerves, respectively, and similar volume occupancy for arteries and nerves. Inter-centroid minimum distance between arteries and nerves was 274 ± 222 μm. The density of vessels and nerves around a point within CC on a given grid was assessed, showing that 50% of all vessels and nerves were found in a radial distance of 1.6–1.8 mm from any of these points, which is strategically relevant when using stimulation needles in the auricle for excitation of nerves. HREM seems suitable for anatomical studies of the human ear. A 3D model of CC was established in the micrometer scale, which forms the basis for future optimization of the auricular VNS. Obviously, the presented single cadaver study needs to be validated by additional anatomical data on the innervation and vascularization of the auricle.
Feel Free To Share This Neuroscience News.







