Summary: Applying rapid short pulses of ultrasound can non-invasively deliver liposomes directly to the brain, across the blood-brain barrier.
Source: King’s College London
In a new study researchers from the School of Biomedical Engineering & Imaging Sciences, in collaboration with the Noninvasive Surgery & Biopsy Laboratory led by Dr. James Choi at Imperial College London, have found that applying rapid short pulses (RaSP) of ultrasound can non-invasively deliver liposomes to the brain, across the blood-brain barrier. This is a specialized barrier between the brain and blood which restricts the entry of molecules to the brain, including over 90 percent of drugs.
Their results were published in the Journal of Controlled Release.
There are currently no non-invasive ways to minimize the damage to the blood-brain barrier and there is a big demand for methods to deliver large macromolecules to the brain safely to treat brain diseases.
Liposomal nanomedicines carry high concentrations of drugs and target drug release at the sites of inflammation and infection, in particular to deliver multiple drugs that cannot cross the brain and treat neurodegenerative diseases as well as brain tumors.
Liposomes are important for multiple treatments as they have shown promise in cancer, inflammation and infection treatment by delivering high concentrations of drugs. Clinically approved liposome formulations include Pfizer/BioNTech’s BNT162b2 COVID vaccine.
The additional advantage that liposomes have over other drug carriers include the ability to deliver high drug concentration of hydrophilic as well as hydrophobic drugs. They can be easily modified passively or actively to achieve target specificity, says Aishwarya Mishra, Ph.D. student, School of Biomedical Engineering & Imaging Sciences.
Focused ultrasound is a method of delivering high frequency sound waves concentrated onto a specific area to deliver a large amount of controlled energy to cause temporary or permanent disturbance in the target area depending on the duration and frequency of the sound wave.
Previous studies have delivered liposomes to the brain but have shown this delivery to be invasive and damaging to brain vasculature.
Delivery of liposomes with RaSP sequences shows promise with a diffused delivery and larger spread. Liposomes can reach inside certain (neuronal) cells in the brain. These sequences were found to be safer by investigating with microscopy techniques whether any brain damage was observed compared to conventionally used long pulses of focused ultrasound.
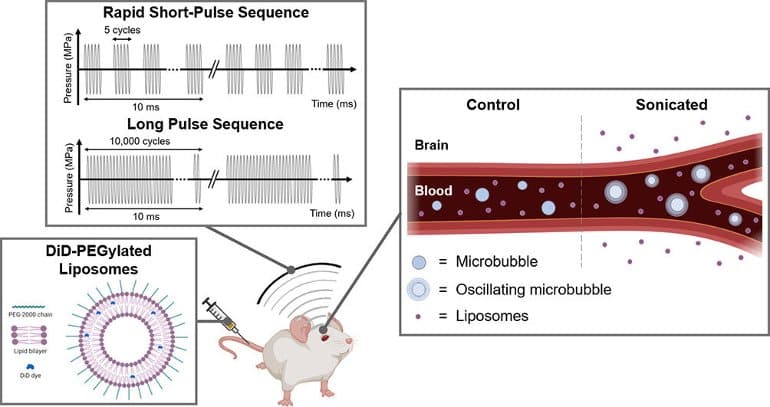
In this study, the researchers used a mouse model where the ultrasound waves were focused on the left side of the mouse brain. Microbubbles, gas filled bubbles which oscillate (expand and contract) in sync with ultrasound waves—and liposomes—lipid balls filled with medicine—were then injected into the bloodstream through the tail.
The ultrasound waves make the microbubbles oscillate which opens the brain’s barrier around the bubbles leading to entry of liposomes.
“Our other key finding was the ability to study the liposomes being delivered to different types of neuronal cells showing the liposomes are taken up by these targets and can be used to treat the diseases associated with these cells,” says Mishra.
About this neuroscience research news
Author: Press Office
Source: King’s College London
Contact: Press Office – King’s College London
Image: The image is credited to the researchers
Original Research: Open access.
“Liposome delivery to the brain with rapid short-pulses of focused ultrasound and microbubbles” by Sophie V. Morse et al. Journal of Controlled Release
Abstract
Liposome delivery to the brain with rapid short-pulses of focused ultrasound and microbubbles
Liposomes are clinically used drug carriers designed to improve the delivery of drugs to specific tissues while minimising systemic distribution. However, liposomes are unable to cross the blood-brain barrier (BBB) and enter the brain, mostly due to their large size (ca. 100 nm).
A noninvasive and localised method of delivering liposomes across the BBB is to intravenously inject microbubbles and apply long pulses of ultrasound (pulse length: >1 ms) to a targeted brain region.
Recently, we have shown that applying rapid short pulses (RaSP) (pulse length: 5 μs) can deliver drugs with an improved efficacy and safety profile. However, this was tested with a relatively smaller 3-kDa molecule (dextran).