Summary: For the 60 million Americans living with chronic pain, the sensation isn’t just a lingering warning—it’s a biological misinterpretation. A groundbreaking study has finally mapped the specific neural “loop” responsible for this persistence.
By tracing a glowing trail of neurons from the spinal cord to the cortex and back again, researchers discovered a dedicated circuit that activates only after injury or inflammation. Most significantly, they found that silencing this circuit eliminates chronic hypersensitivity while leaving “protective” acute pain (the kind that tells you a stove is hot) perfectly intact.
Key Facts
- Separation of Pain: The study proves that acute and chronic pain are neurologically distinct. One is a vital survival signal; the other is a dedicated “pathological” circuit that can be targeted individually.
- The “Sensitization” Loop: The circuit originates in the spinal cord, travels through the thalamus and cortex, hits the brainstem (RVM), and loops back to the spine.
- Touch into Pain: In a chronic state, this circuit causes the brain to misinterpret gentle touch as a painful stimulus.
- Artificial Induction: In healthy mice, simply activating this circuit multiple times was enough to create a chronic pain state that lasted for weeks, even without an actual injury.
- Treatment Potential: Since this circuit is not engaged in “normal” pain, drugs or therapies that “jam” this specific loop could treat chronic conditions without dulling a person’s ability to sense immediate danger.
Source: Stanford
A new map of a brain circuit specific to chronic pain suggests a promising route to treatment for the roughly 60 million Americans living with persistent pain, according to a study published in Nature.
The study showed that silencing the specific cells that drive this circuit eased chronic pain while preserving acute pain responses—in other words, the body’s ability to signal danger.
“A surprise to us was that acute pain and chronic pain can be completely separate,” said senior author Xiaoke Chen, a Wu Tsai Neurosciences Institute affiliate and associate professor of biology at Stanford Humanities and Sciences. “There is a dedicated circuit that only activates after injury, which gives us the opportunity to target the chronic pain component but leave protective acute pain intact.”
The research was supported in part by the NeuroChoice Initiative, a Wu Tsai Neuro Big Ideas in Neuroscience project focused on understanding biological mechanisms of addiction, including the risk for people who take prescription opioids for chronic pain.
A misinterpretation in the brain
Pain is a critical response all animals have evolved to warn us of danger and motivate us to seek healing. The defining feature of chronic pain is that it persists long after the immediate threat has dissipated. It can follow an injury, inflammation or other condition, and people with chronic pain are at greater risk of mental health problems and opioid misuse.
A hallmark of chronic pain is sensitization, where patients become hypersensitive to touch and other normally benign sensations. “In chronic pain, the brain misinterprets touch to be a painful stimulus,” said Chen.
Identifying the specific neurological circuit loop responsible for this misinterpretation could help correct it. Previous research has shown it’s possible to dampen pain by electrically stimulating the periaqueductal gray (PAG) and its downstream region called the rostral ventromedial medulla (RVM). Researchers have hypothesized that the PAG-RVM may form a system that’s important for chronic pain as well, but researchers had yet to identify a full circuit for chronic pain.
Mapping a new pain pathway
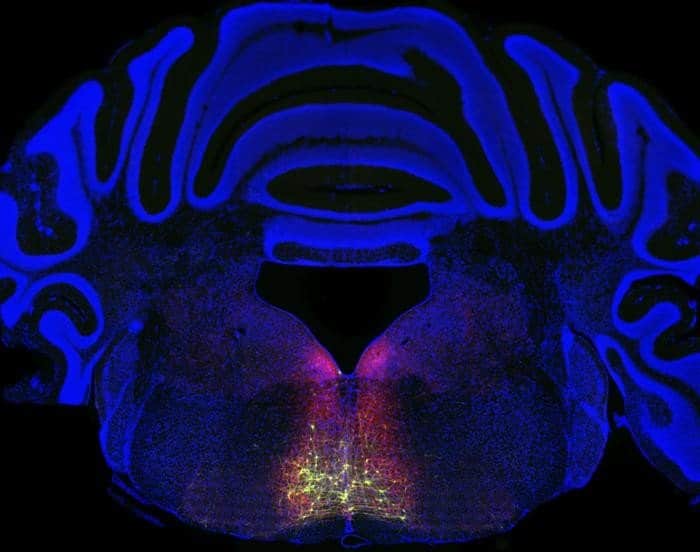
To find that full circuit, Chen’s team worked backwards from a group of neurons found in the RVM known to be involved in pain sensitization. Building on previous genetic methods, they tagged neurons along the chronic pain circuit with a fluorescent protein.
The glowing trail that resulted revealed a previously unknown circuit loop originating in the spinal cord, then linking to the thalamus, the cortex, the brainstem (where the RVM is located), and back to the spinal cord.
By chemically silencing that circuit, the team showed it was specific to chronic pain. Before silencing, mice shied away even from relatively gentle touches—a key sign they were experiencing chronic pain. Afterward, the mice responded appropriately to gentle and rougher stimuli. In other words, their chronic pain subsided, leaving their protective acute pain response intact.
“When silencing this group of cells, the sensitized pain goes away,” said Chen. “Therefore, the activity of these cells is necessary for injury or inflammation-induced pain sensitization.”
Activating the same circuit in healthy mice actually induced chronic pain. By chemically stimulating neurons in the circuit multiple times, the team found they could increase pain sensitivity in the mice and that this sensitivity lasted for weeks afterward. “Just activating these neurons is enough to induce a chronic pain state,” said Chen.
The experiments confirmed the circuit’s specific role in chronic pain. “This group of cells is not engaged in normal pain, but only in chronic pain that occurs after injury or inflammation,” Chen said.
The discovery of a new circuit doesn’t mean the previously proposed PAG-RVM pain system is irrelevant. More likely, the two circuits control pain in opposite ways. While stimulating the newly identified circuit increases pain, stimulating the PAG-RVM system reduces pain. “We think that reducing pain and promoting pain are driven by two separate circuits,” said Chen.
Jamming the chronic pain circuit
With the circuit now mapped, Chen is searching for molecular changes that lead the RVM neurons to light up the chronic pain circuit. It may be possible to develop drugs that block this change or that jam the signals the neurons send through the loop. Future medications that target this circuit could potentially ease chronic pain without impacting the ability to feel immediate, acute pain.
Chen is also researching genetic databases from chronic pain patients to determine whether similar changes occur in humans. That work will help researchers confirm whether the same molecular changes identified in mice also control chronic pain in humans, Chen said.
At a deeper level, the discovery raises an intriguing question: Why does a dedicated chronic pain circuit exist at all? Chen thinks it may be linked to how the brain detects internal damage, particularly since the brain itself lacks pain-sensing neurons. For now, “it’s still a mystery,” he said.
Key Questions Answered:
A: It’s a bit of a biological mystery. Senior author Xiaoke Chen suggests it might be the brain’s way of monitoring internal damage that it otherwise couldn’t “feel.” However, in chronic pain, this system goes into overdrive, effectively “lying” to the brain by telling it that a gentle touch is a wound.
A: No—and that’s the breakthrough! Previous painkillers (like opioids) dull all pain, which is dangerous. This study shows we can “snip” the chronic loop while leaving the “emergency broadcast system” of acute pain fully operational.
A: The circuit has been mapped in mice, and the team is currently cross-referencing human genetic databases to see if the same molecular “switches” exist in us. If they match, it opens the door for a entirely new class of non-opioid medications.
Editorial Notes:
- This article was edited by a Neuroscience News editor.
- Journal paper reviewed in full.
- Additional context added by our staff.
About this pain research news
Author: Nathan Collins
Source: Stanford University
Contact: Nathan Collins – Stanford University
Image: The image is credited to Courtesy Xiaoke Chen/Stanford University
Original Research: Open access.
“Deconstruction of a spino-brain–spinal cord circuit that drives chronic pain” by Qian Wang (王倩), Joo Han Lee (이주한), Gregory Nachtrab, Yuan Yuan, Lei Yuan, Wei Qi, Manuel A. Mohr, Jing Xiong, Mark A. Horowitz & Xiaoke Chen (陈晓科). Nature
DOI:10.1038/s41586-026-10296-y
Abstract
Deconstruction of a spino-brain–spinal cord circuit that drives chronic pain
Tissue inflammation or nerve injury at the periphery can cause chronic pain. Although the spinal-cord-projecting neurons in the rostral ventromedial medulla (RVMSC neurons) can promote pain chronification, the pathway by which peripheral injury signals drive these neurons is poorly understood.
Here we report a circuit loop that extends from the spinal cord to the ventral posterolateral thalamus and posterior complex of the thalamus, proceeds to the primary somatosensory cortex and returns to the spinal cord via the lateral superior colliculus, which in turn connects to μ-opioid-receptor-expressing RVMSC neurons.
Silencing any node along this multisynaptic circuit has minimal effects on nociception in healthy mice, but can eliminate mechanical hypersensitization and restore normal nociceptive response thresholds in mouse models of inflammatory and neuropathic pain. In healthy mice, repetitive—but not acute—activation of each node in this circuit is sufficient to cause robust chronic mechanical hypersensitization.
Our findings reveal a spino-brain–spinal cord circuit loop that links ascending and descending pathways and specifically drives chronic mechanical pain. This could enable the identification of cellular targets for treating chronic pain.