Researchers have developed a procedure to mimic in laboratory experiments a form of brain trauma commonly seen in combat veterans, and findings suggest a new diagnostic tool for early detection and a potential treatment.
About one in five wounded soldiers suffers from traumatic brain injury and an estimated 52 percent of those injuries are blast-induced neurotrauma. A subclass called mild blast-induced neurotrauma is particularly difficult to diagnose because people who have it often display no obvious motor impairment or other neurological symptoms, said Riyi Shi, a professor in Purdue University’s Department of Basic Medical Sciences, College of Veterinary Medicine, and Weldon School of Biomedical Engineering.
“Many times they don’t even realize they’ve been injured, and this is particularly alarming because these injuries have been linked to severe long-term psychiatric and degenerative neurological dysfunction,” he said. “The underlying mechanisms of injury remain poorly understood, impeding development of diagnostic and treatment strategies.”
The initial injury is caused by the shock wave from explosions. However, researchers believe secondary damage takes place in the days and weeks that follow the initial injury, and this secondary damage might be treatable.
The researchers have developed a method to mimic mild blast-induced neurotrauma in laboratory rats, representing a new strategy to establish a clinically relevant “animal model” that recreates typical human symptom profiles. This model can be used to study the effects and pinpoint mechanisms responsible for ongoing damage that occurs following the initial injury, Shi said.
Findings, which appeared on Aug. 21 in the Journal of Neurosurgery, suggest a simple urine test could be used to diagnose the injury, and damaging effects might be alleviated through drug therapy that reduces the concentration of a toxic compound produced by traumatized cells.
“Early detection and intervention could potentially mitigate or prevent delayed onset development of significant neurological dysfunction,” Shi said.
The paper was authored by graduate students Michael Walls, Nicholas Race, Lingxing Zheng, Sasha M. Vega Alvarez, Glen Acosta, Jonghyuck Park and Shi.
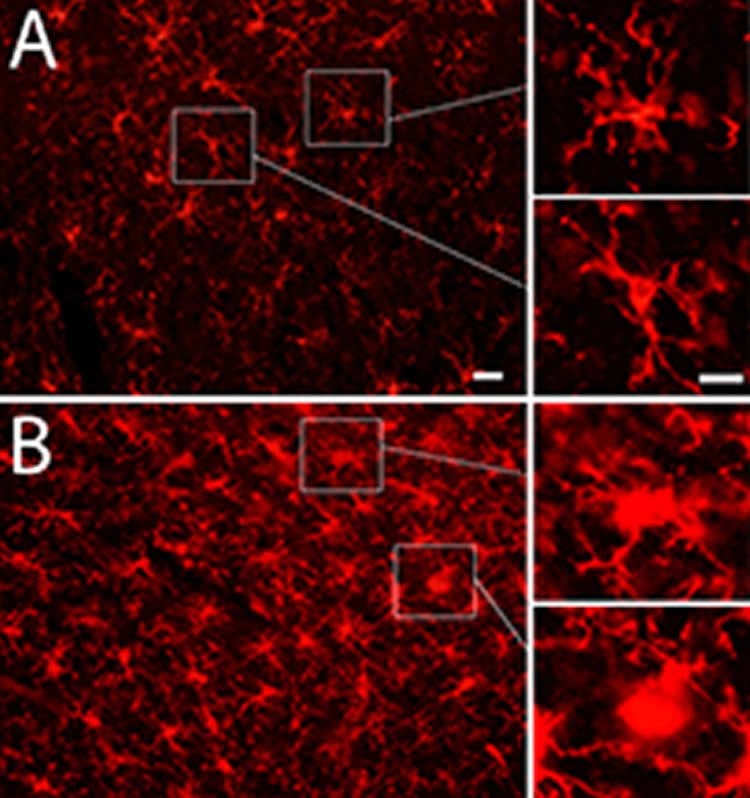
The research shows evidence of brain inflammation that may indicate ongoing damage, potentially leading to altered brain function and degenerative diseases.
“We detected structural and biochemical brain damage without obvious motor or cognitive deficits,” Shi said. “These findings highlight the difficulty and importance of early detection, indicating missed early diagnosis and subsequent lack of intervention could lead to serious long-term consequences.”
A neurotoxin called acrolein is produced within the body after nerve cells are damaged and has been shown to lead to continued damage. However, the concentration of acrolein could be reduced using the drug hydralazine, which has been approved by the U.S. Food and Drug Administration for hypertension, he said.
The drug has been shown to be effective in reducing acrolein levels in previous research led by Shi, who is working to develop a low-dose version for that purpose in humans.
New findings indicate elevated levels of acrolein in brain tissue and in urine from research animals lacking neurological signs of damage. Acrolein concentrations were three times the normal level the first day of the experiment and remained elevated five days later. The findings suggest urine tests showing elevated acrolein might indicate trauma despite the lack of symptoms following mild blast injury. Treatment at this point could reduce the risk of developing chronic neurological diseases, said Shi, who is a member of the International Brain Mechanics and Trauma Lab, a newly established initiative aiming to gather multidisciplinary expertise for the study of brain mechanics in trauma and diseases.
Funding: The research was supported in part by the Indiana State Department of Health (Grant #204200 to RS), National Institutes of Health (Grant # NS073636 to RS), and Indiana CTSI Collaboration in Biomedical Translational Research Pilot Program Grant (Grant #RR025761 to RS). Funding for the LSM710 was provided by NIH NCRR Shared instrumentation Grant 1 S10 RR023734-01A1.
Source: Emil Venere – Purdue
Image Source: The image is credited to Riyi Shi/Purdue
Original Research: Abstract for “Structural and biochemical abnormalities in the absence of acute deficits in mild primary blast-induced head trauma” by Michael K. Walls, MS, Nicholas Race, BS, Lingxing Zheng, PhD, Sasha M. Vega-Alvarez, MS, Glen Acosta, MS, Jonghyuck Park, PhD, and Riyi Shi, MD, PhD in Journal of Neurosurgery. Published online August 21 2015 doi:10.3171/2015.1.JNS141571
Abstract
Structural and biochemical abnormalities in the absence of acute deficits in mild primary blast-induced head trauma
OBJECT
Blast-induced neurotrauma (BINT), if not fatal, is nonetheless potentially crippling. It can produce a wide array of acute symptoms in moderate-to-severe exposures, but mild BINT (mBINT) is characterized by the distinct absence of acute clinical abnormalities. The lack of observable indications for mBINT is particularly alarming, as these injuries have been linked to severe long-term psychiatric and degenerative neurological dysfunction. Although the long-term sequelae of BINT are extensively documented, the underlying mechanisms of injury remain poorly understood, impeding the development of diagnostic and treatment strategies. The primary goal of this research was to recapitulate primary mBINT in rodents in order to facilitate well-controlled, long-term investigations of blast-induced pathological neurological sequelae and identify potential mechanisms by which ongoing damage may occur postinjury.
METHODS
A validated, open-ended shock tube model was used to deliver blast overpressure (150 kPa) to anesthetized rats with body shielding and head fixation, simulating the protective effects of military-grade body armor and isolating a shock wave injury from confounding systemic injury responses, head acceleration, and other elements of explosive events. Evans Blue-labeled albumin was used to visualize blood-brain barrier (BBB) compromise at 4 hours postinjury. Iba1 staining was used to visualize activated microglia and infiltrating macrophages in areas of peak BBB compromise. Acrolein, a potent posttraumatic neurotoxin, was quantified in brain tissue by immunoblotting and in urine through liquid chromatography with tandem mass spectrometry at 1, 2, 3, and 5 days postinjury. Locomotor behavior, motor performance, and short-term memory were assessed with open field, rotarod, and novel object recognition (NOR) paradigms at 24 and 48 hours after the blast.
RESULTS
Average speed, maximum speed, and distance traveled in an open-field exploration paradigm did not show significant differences in performance between sham-injured and mBINT rats. Likewise, rats with mBINT did not exhibit deficits in maximum revolutions per minute or total run time in a rotarod paradigm. Short-term memory was also unaffected by mBINT in an NOR paradigm. Despite lacking observable motor or cognitive deficits in the acute term, blast-injured rats displayed brain acrolein levels that were significantly elevated for at least 5 days, and acrolein’s glutathione-reduced metabolite, 3-HPMA, was present in urine for 2 days after injury. Additionally, mBINT brain tissue demonstrated BBB damage 4 hours postinjury and colocalized neuroinflammatory changes 24 hours postinjury.
CONCLUSIONS
This model highlights mBINT’s potential for underlying detrimental physical and biochemical alterations despite the lack of apparent acute symptoms and, by recapitulating the human condition, represents an avenue for further examining the pathophysiology of mBINT. The sustained upregulation of acrolein for days after injury suggests that acrolein may be an upstream player potentiating ongoing postinjury damage and neuroinflammation. Ultimately, continued research with this model may lead to diagnostic and treatment mechanisms capable of preventing or reducing the severity of long-term neurological dysfunction following mBINT.
“Structural and biochemical abnormalities in the absence of acute deficits in mild primary blast-induced head trauma” by Michael K. Walls, MS, Nicholas Race, BS, Lingxing Zheng, PhD, Sasha M. Vega-Alvarez, MS, Glen Acosta, MS, Jonghyuck Park, PhD, and Riyi Shi, MD, PhD in Journal of Neurosurgery. Published online August 21 2015 doi:10.3171/2015.1.JNS141571






