Summary: Study sheds light on the role brain insulin plays in weight and visceral fat accumulation.
Source: DZD
Just where fat is deposited in the body and to what degree a person may benefit from a lifestyle intervention depends, among other things, on how sensitive the brain is to insulin. If the person’s brain responds sensitively to the hormone, a significant amount of weight can be lost, unhealthy visceral fat reduced, and the weight loss can be maintained over the long term. However, If the person’s brain responds only slightly or not at all to insulin, the person only loses some weight at the beginning of the intervention and then experiences weight regain. Over the long term, the visceral fat also increases. These are the results of a long-term study by the German Center for Diabetes Research (DZD), Helmholtz Zentrum München and Tübingen University Hospital which has now been published in Nature Communications.
To which extent body fat has an unhealthy effect depends primarily on where it is stored. If fat accumulates in the abdomen, this is particularly unfavorable. This is because the visceral fat releases numerous neurotransmitters that affect blood pressure, influence the secretion of the hormone insulin and can cause inflammation. This increases the risk of diabetes, cardiovascular disease and certain types of cancer. The subcutaneous fat which accumulates on the buttocks, thighs and hips has no adverse health effects. However, it is still unclear why fat storage does not occur in the same place in all people. Studies in the Tübingen Lifestyle Intervention Program (TULIP) [1] suggest that brain insulin responsiveness could play an important role here. They showed that people with a high insulin sensitivity in the brain benefit significantly more from a lifestyle intervention with a diet rich in fiber and exercise than people with insulin resistance in the brain. Not only did they lose more weight, they also had a healthier fat distribution. But how does insulin sensitivity affect the distribution of body fat and weight in the long term? Researchers from the German Center for Diabetes Research (DZD), Helmholtz Zentrum München and Tübingen University Hospital investigated this question in a long-term study. For this purpose, they recorded the follow-up data of 15 participants over a period of nine years, in which the insulin sensitivity in the brain was determined by magnetoencephalography before the start of a 24-month lifestyle intervention.
High insulin sensitivity associated with reduction in visceral fat and weight
It was found that insulin action in the brain not only determines body weight, but also the distribution of fat in the body. “Subjects with high insulin sensitivity in the brain benefited from the lifestyle intervention with a pronounced reduction in weight and visceral fat. Even after the lifestyle intervention had ended, they only regained a small amount of fat during the nine-year follow-up,” said the head of the study, Professor Martin Heni from Tübingen University Hospital. In contrast, people with brain insulin resistance only showed a slight weight loss in the first nine months of the program. “Afterwards, their body weight and visceral fat increased again during the following months of lifestyle intervention,” said first author PD Dr. Stephanie Kullmann from the IDM.
Since the insulin action in the hypothalamus is crucial for the regulation of peripheral energy metabolism, the researchers also investigated how insulin sensitivity in this area of the brain is related to the distribution of body fat. For this purpose, they examined a cross-sectional cohort of 112 participants. The analysis of the data showed that people with high insulin sensitivity in the hypothalamus form little visceral fat. However, insulin sensitivity has no influence on the mass of subcutaneous fat.
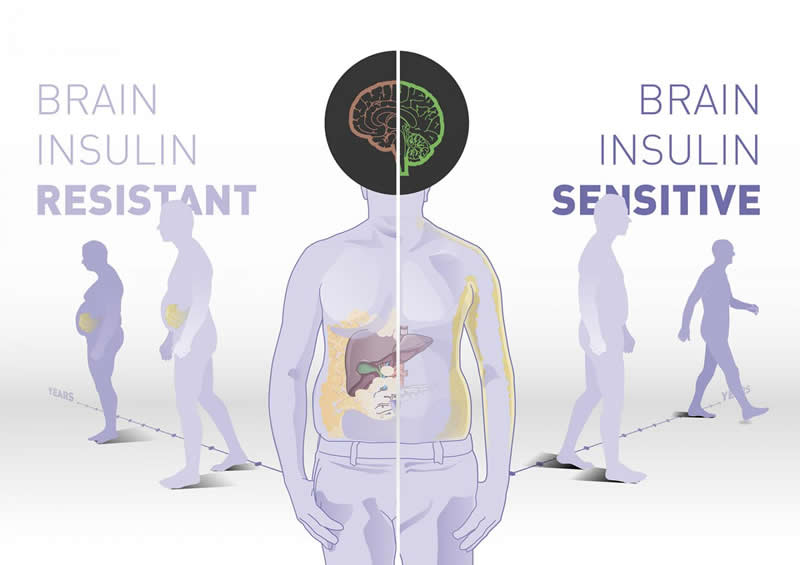
Our study reveals a novel key mechanism that regulates fat distribution in humans. Insulin sensitivity in the brain determines where fat is deposited, “said Heni, summarizing the results. Since visceral fat not only plays a role in the development of type 2 diabetes, but also increases the risk of cardiovascular disease and cancer, the study results may also open up new approaches for treatment options beyond metabolic diseases. The researchers in Tübingen are already working on new therapies to abolish insulin resistance in the brain and thus have a beneficial effect on body fat distribution.
About this neuroscience research article
Source:
DZD
Media Contacts:
Martin Heni – DZD
Image Source:
The image is credited to IDM.
Original Research:Open access
“Brain insulin sensitivity is linked to adiposity and body fat distribution”. by Stephanie Kullmann, Vera Valenta, Robert Wagner, Otto Tschritter, Jürgen Machann, Hans-Ulrich Häring, Hubert Preissl, Andreas Fritsche & Martin Heni.
British Journal of Pharmacology doi:10.1038/s41467-020-15686-y
Abstract
Brain insulin sensitivity is linked to adiposity and body fat distribution
Brain insulin action regulates eating behavior and energy fluxes throughout the body. However, numerous people are brain insulin resistant. How brain insulin responsiveness affects long-term weight and body fat composition in humans is still unknown. Here we show that high brain insulin sensitivity before lifestyle intervention associates with a more pronounced reduction in total and visceral fat during the program. High brain insulin sensitivity is also associated with less regain of fat mass during a nine year follow-up. Cross-sectionally, strong insulin responsiveness of the hypothalamus associates with less visceral fat, while subcutaneous fat is unrelated. Our results demonstrate that high brain insulin sensitivity is linked to weight loss during lifestyle intervention and associates with a favorable body fat distribution. Since visceral fat is strongly linked to diabetes, cardiovascular risk and cancer, these findings have implications beyond metabolic diseases and indicate the necessity of strategies to resolve brain insulin resistance.
Feel Free To Share This Neuroscience News.






