Summary: Researchers have discovered a new methoc that can predict a person’s current level of awareness and whether they will recover awareness within a year of a TBI.
Source: Cell Press.
The precise diagnosis and prognosis of recovery of consciousness of patients after a severe brain injury is a challenging clinical task, as some brain-injured patients retain certain levels of awareness despite appearing fully unresponsive. Now, researchers reporting in the Cell Press journal Current Biology on May 26 have evidence that readily obtainable measures of the amount of glucose (sugar) consumed by the brain can directly predict a person’s current level of awareness, or the likelihood that they will recover awareness within a year.
“In nearly all cases, whole-brain energy turnover directly predicted either the current level of awareness or its subsequent recovery,” says Ron Kupers of the University of Copenhagen and Yale University. “In short, our findings indicate that there is a minimal energetic requirement for sustained consciousness to arise after brain injury.”
In the new study, Kupers, together with Johan Stender and colleagues from the University of Copenhagen in Denmark and the University of Liège in Belgium, aimed to develop more-reliable diagnostic markers for the assessment of current and future levels of consciousness to complement routine bedside clinical examinations. To this end, they quantified and mapped cerebral glucose metabolism in 131 brain-injured patients, all of whom were suffering from either full or partial loss of consciousness.
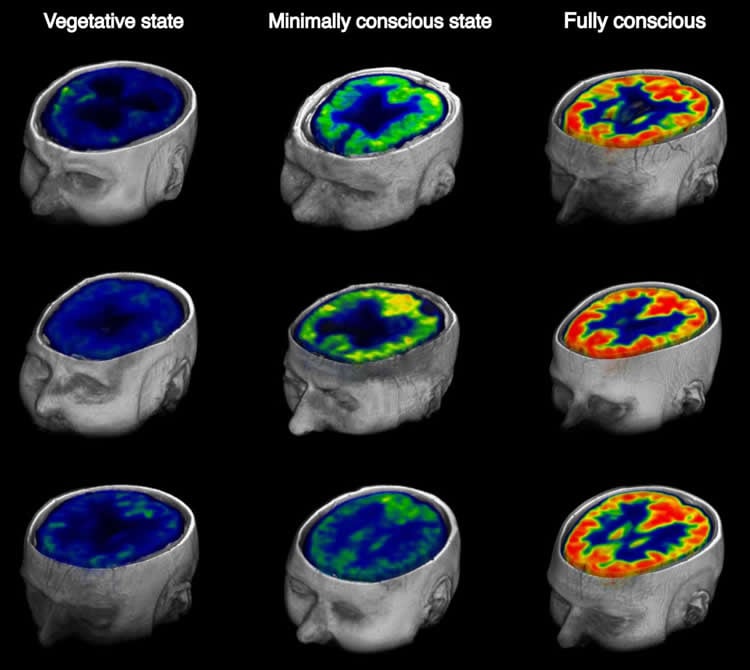
Their results showed that the patients’ individual levels of behavioral responsiveness were strongly linked to their overall cerebral energy turnover. In fact, patients with glucose metabolism below a well-defined threshold of 42 percent of normal cortical activity appeared to be fully unconscious and did not recover consciousness at 1-year follow-up. In contrast, nearly all patients with brain metabolic activity above this energetic threshold either showed signs of awareness at the initial examination or had recovered responsiveness a year later.
Overall, the researchers report, the cerebral metabolic rate accounted for the current level, or imminent return, of awareness in 94 percent of patients.
“The discovery of a clear metabolic boundary between the conscious and unconscious states could imply that the brain undergoes a fundamental state change at a certain level of energy turnover, in a sense that consciousness ‘ignites’ as brain activity reaches a certain threshold,” Stender says. “We were not able to test this hypothesis directly, but it provides a very interesting direction for future research.”
“The take-home message [for now] is that consciousness is a highly energy demanding process, involving the brain at large,” Kupers says. “This fundamental physiological trait can help clinicians determine the potential for recovery of awareness in patients suffering from severe brain injuries of any kind.”
The researchers say it will be important to verify the findings in an independent patient population. They also hope to explore how brain metabolism changes over time in brain-injured patients.
Funding: The study was supported financially by the University of Copenhagen, the Belgian Fund for Scientific Research, the James S. McDonnell Foundation, the Belgian American Educational Foundation, the Wallonie-Bruxelles International, the European Commission, the European Space Agency, the Wallonia- Brussels Federation Concerted Research Action, and the Belgian interuniversity attraction pole.
Source: Joseph Caputo – Cell Press
Image Source: This NeuroscienceNews.com image is credited to Stender et al.
Original Research: Abstract for “The Minimal Energetic Requirement of Sustained Awareness after Brain Injury” by Johan Stender, Kristian Nygaard Mortensen, Aurore Thibaut, Sune Darkner, Steven Laureys, Albert Gjedde, and Ron Kupers in Current Biology. Published online April 28 2016 doi:10.1016/j.cub.2016.04.024
[cbtabs][cbtab title=”MLA”]Cell Press. “A Way To Measure Awareness, or its Impending Return, in Brain Injury Patients.” NeuroscienceNews. NeuroscienceNews, 26 May 2016.
<https://neurosciencenews.com/brain-injury-awareness-4314/>.[/cbtab][cbtab title=”APA”]Cell Press. (2016, May 26). A Way To Measure Awareness, or its Impending Return, in Brain Injury Patients. NeuroscienceNews. Retrieved May 26, 2016 from https://neurosciencenews.com/brain-injury-awareness-4314/[/cbtab][cbtab title=”Chicago”]Cell Press. “A Way To Measure Awareness, or its Impending Return, in Brain Injury Patients.” https://neurosciencenews.com/brain-injury-awareness-4314/ (accessed May 26, 2016).[/cbtab][/cbtabs]
Abstract
The Minimal Energetic Requirement of Sustained Awareness after Brain Injury
Differentiation of the minimally conscious state (MCS) and the unresponsive wakefulness syndrome (UWS) is a persistent clinical challenge. Based on positron emission tomography (PET) studies with [18F]-fluorodeoxyglucose (FDG) during sleep and anesthesia, the global cerebral metabolic rate of glucose has been proposed as an indicator of consciousness. Likewise, FDG-PET may contribute to the clinical diagnosis of disorders of consciousness (DOCs). However, current methods are non-quantitative and have important drawbacks deriving from visually guided assessment of relative changes in brain metabolism. We here used FDG-PET to measure resting state brain glucose metabolism in 131 DOC patients to identify objective quantitative metabolic indicators and predictors of awareness. Quantitation of images was performed by normalizing to extracerebral tissue. We show that 42% of normal cortical activity represents the minimal energetic requirement for the presence of conscious awareness. Overall, the cerebral metabolic rate accounted for the current level, or imminent return, of awareness in 94% of the patient population, suggesting a global energetic threshold effect, associated with the reemergence of consciousness after brain injury. Our data further revealed that regional variations relative to the global resting metabolic level reflect preservation of specific cognitive or sensory modules, such as vision and language comprehension. These findings provide a simple and objective metabolic marker of consciousness, which can readily be implemented clinically. The direct correlation between brain metabolism and behavior further suggests that DOCs can fundamentally be understood as pathological neuroenergetic conditions and provide a unifying physiological basis for these syndromes.
“The Minimal Energetic Requirement of Sustained Awareness after Brain Injury” by Johan Stender, Kristian Nygaard Mortensen, Aurore Thibaut, Sune Darkner, Steven Laureys, Albert Gjedde, and Ron Kupers in Current Biology. Published online April 28 2016 doi:10.1016/j.cub.2016.04.024