Summary: A new study reports anemia may negatively affect the outcomes of patients with TBI.
Source: University of Missouri.
Finding lays foundation for new treatment protocols for anemic patients.
Approximately half of patients hospitalized with traumatic brain injuries are anemic, according to recent studies, but anemia’s effects on the recovery of these patients is not clear. Now, researchers from the University of Missouri School of Medicine have found evidence that anemia can negatively influence the outcomes of patients with traumatic brain injuries.
“More research is needed to develop treatment protocols for anemic patients with traumatic brain injuries,” said N. Scott Litofsky, M.D., chief of the MU School of Medicine’s Division of Neurological Surgery and lead author of the study. “Anemia occurs when there is a shortage of red blood cells, which causes reduced oxygen flow to vital organs throughout the body. There has been a lack of consensus among physicians regarding the relationship of anemia and traumatic brain injuries on a patient’s health. Because of this uncertainty, treatment protocols are unclear and inconsistent. Our observational study found that a patient’s outcome is worse when he or she is anemic.”
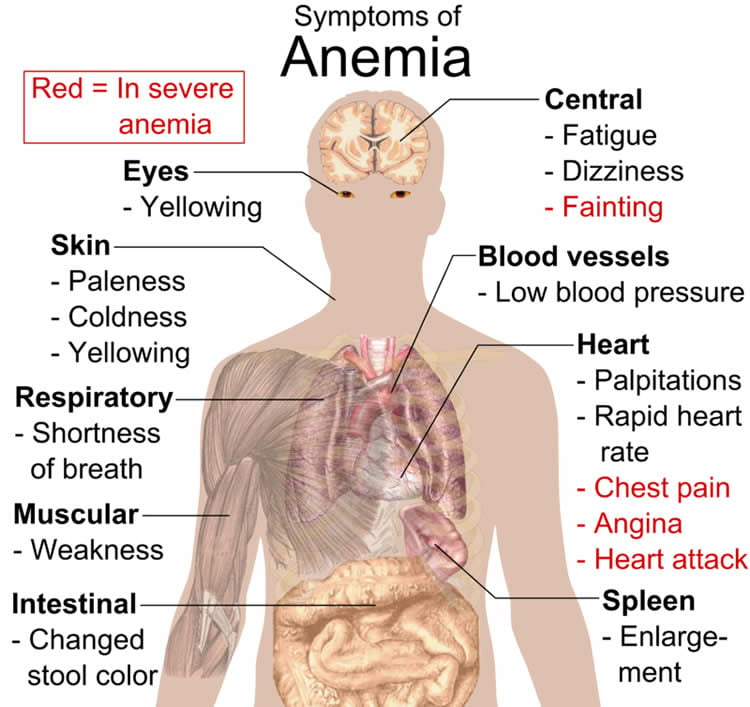
Red blood cells contain hemoglobin, a protein crucial to the delivery of oxygenated blood. The researchers studied the outcomes of 939 traumatic brain injury patients with anemia admitted to the Frank L. Mitchell Jr., M.D., Trauma Center, a Level I trauma center that is part of MU Health Care. The researchers compared hemoglobin levels of these patients and their outcomes within one year of surgery.
Despite also having more severe head and systemic injuries, patients with lower levels of hemoglobin had a poor outcome. For each increase in hemoglobin of 1 gram above 7 grams per deciliter of blood, the likelihood of a good outcome increased by 33 percent.
To restore a patient’s hemoglobin level, a patient can receive a blood transfusion. However, stored blood may not perform as well as a patient’s own blood, and patients may experience allergic reactions or viral infections as a result of the transfusion. Additionally, the cost of one unit of blood ranges from $200 to $300.
“The purpose of this study is not to propose transfusion guidelines, but rather to show that anemia can be harmful to patients with traumatic brain injuries,” Litofsky said. “Now that we have shown that anemia affects a patient’s recovery, further studies are needed to determine the best way to correct it. The ultimate goal of this research is to help patients recover more quickly from traumatic brain injuries.”
The study, “The Negative Impact of Anemia in Outcome from Traumatic Brain Injury,” was presented at the recent 84th American Association of Neurological Surgeons Annual Scientific Meeting. The research also was recently published by the peer-reviewed journal World Neurosurgery. Research reported in this publication was supported by the MU School of Medicine and the MU Department of Surgery. The researchers have no conflicts of interest to declare related to this study.
In addition to Litofsky, the research team included Simon Martin and Jenna Diaz, medical students at the MU School of Medicine; Bin Ge and Greg Petroski; statisticians with the MU Medical Research Office; Douglas Miller, M.D., professor in the MU Department of Pathology and Anatomical Sciences; and Stephen Barnes, M.D., professor and chief of the MU Division of Acute Care Surgery.
Funding: This work was supported by the University of Missouri School of Medicine, University of Missouri Department of Surgery.
Source: Derek Thompson – University of Missouri
Image Source: This NeuroscienceNews.com image is credited to Mikael Häggström and is in the public domain.
Original Research: Abstract for “The Negative Impact of Anemia in Outcome from Traumatic Brain Injury” by N. Scott Litofsky, Simon Martin, Jenna Diaz, Bin Ge, Greg Petroski, Douglas C. Miller, Stephen L. Barnes in World Neurosurgery. Published online May 2016 doi:10.1016/j.wneu.2016.02.076
[cbtabs][cbtab title=”MLA”]University of Missouri. “Anemia Could Affect Recovery From TBI.” NeuroscienceNews. NeuroscienceNews, 25 May 2016.
<https://neurosciencenews.com/anemia-tbi-neurology-4301/>.[/cbtab][cbtab title=”APA”]University of Missouri. (2016, May 25). Anemia Could Affect Recovery From TBI. NeuroscienceNews. Retrieved May 25, 2016 from https://neurosciencenews.com/anemia-tbi-neurology-4301/[/cbtab][cbtab title=”Chicago”]University of Missouri. “Anemia Could Affect Recovery From TBI.” https://neurosciencenews.com/anemia-tbi-neurology-4301/ (accessed May 25, 2016).[/cbtab][/cbtabs]
Abstract
The Negative Impact of Anemia in Outcome from Traumatic Brain Injury
Background
Whether anemia complicating traumatic brain injury (TBI) has an impact on patient outcomes is controversial; therefore, recommendations for blood transfusions for such patients are inconsistent. We hypothesized that patient outcome after TBI would be worse in patients with lower hemoglobin levels.
Methods
We retrospectively reviewed records of patients with TBI and head Abbreviated Injury Scale >3 with abnormal head computed tomography findings and neurologic injury. The relationships between initial hemoglobin and lowest hemoglobin during hospitalization at threshold values of ≤7, ≤8, ≤9, and ≤10 g/dL were investigated relative to Glasgow Outcome Score at last follow-up not exceeding 1 year.
Results
Of 939 patients meeting inclusion criteria, initial and lowest hemoglobin concentrations were significant predictors of poor outcome (P < 0.0001). For each 1 g/dL higher hemoglobin value, the likelihood of a good outcome increased by 33%. More severe levels of initial anemia were associated with lower Glasgow Coma Scale, greater head Abbreviated Injury Scale, and greater Injury Severity Score (P < 0.0001). Female patients had worse outcome than male patients only for initial hemoglobin between 7 and 8 g/dL (P < 0.05). Blood transfusion was associated with poorer outcome at hemoglobin levels ≤9 and ≤10 g/dL (P < 0.05), but not at lower hemoglobin thresholds.
Conclusions
Patient outcome after TBI is worse in patients with lower hemoglobin. Initial hemoglobin and lowest hemoglobin after admission are independently associated with poor outcome. Our data support consideration of blood transfusion when hemoglobin is ≤8 g/dl.
“The Negative Impact of Anemia in Outcome from Traumatic Brain Injury” by N. Scott Litofsky, Simon Martin, Jenna Diaz, Bin Ge, Greg Petroski, Douglas C. Miller, Stephen L. Barnes in World Neurosurgery. Published online May 2016 doi:10.1016/j.wneu.2016.02.076






