Summary: Visual responsiveness in the somatosensory cortex diminishes significantly following mirror therapy for phantom limb pain. Before therapy, researchers discovered a strong, unexpected activation in the sensorimotor foot region of amputees to visually presented images of the foot. This response was no longer present following mirror therapy.
Source: Brunel University
Easing phantom limb pain can be as simple as looking in the mirror.
Scientists who have mapped how mirror therapy changes the brain may now be able to predict just how much treatment will ease a particular patient’s pain.
Phantom limb pain—feeling intense pain in a missing limb—happens to more than 90% of amputees and can start just 24 hours after surgery. Drugs don’t work well.
Mirror therapy—symmetrical exercises in a mirror where patients “see” their phantom limb move as if it were really there—has long been used to treat it.
Now new research charting brain changes before and after therapy means scientists may soon be able to predict how well it will work in different people.
The sensation-processing part of the brain, the somatosensory cortex, maps the body surfaces. For example, wiggling your toes activates the ‘toe area’ of the brain. Losing the limb may alter these maps.
“Mirror therapy works by kind of fooling the brain with visual inputs,” said Brunel University London’s Dr. Annie Chan. Her study is one of the first to track how over time mirror therapy changes brain activation after the loss of somatosensory feedback from a missing foot through amputation.
Working at the National Institute of Mental Health (Laboratory of Brain and Cognition, Section of learning and Plasticity), Bethesda, U.S., the team measured brain activity before, during and after four weeks of daily mirror therapy. They compared results from amputees with those from people without amputations.
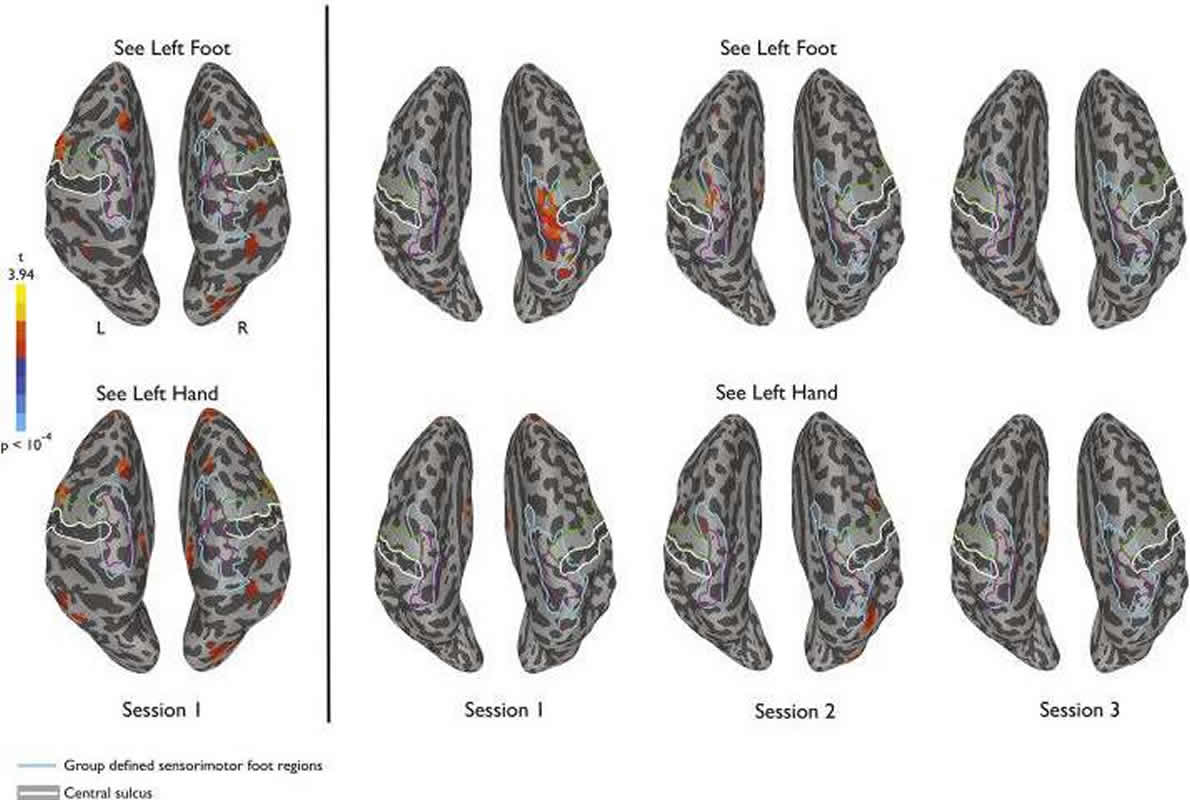
“Prior to therapy, we found a strong unexpected activation or response in sensorimotor foot region of amputees to visually presented images of the foot. This unexpected activation was absent in people without amputations,” said Dr. Chan.
“This response to visually presented limbs was no longer present at the end of the mirror therapy when perceived phantom limb pain was also reduced.”
Overall, the amputees’ phantom limb pain was reduced by 46% from the first scan through to the third session of therapy.
“Our findings highlight the visual responses to the body in amputees might be useful in predicting the efficacy of pain management program for other neuropathy pain. Future work will be needed to establish the robustness of our findings with a much larger sample size and whether similar effects are observed in arm amputees.”
Source:
Brunel University
Media Contacts:
Hayley Jarvis – Brunel University
Image Source:
The image is adapted from the Brunel University news release.
Original Research: Open access
“Visual responsiveness in sensorimotor cortex is increased following amputation and reduced after mirror therapy”. Annie W.-Y. Chan et al.
NeuroImage: Clinical. doi:10.1016/j.nicl.2019.101882
Abstract
Visual responsiveness in sensorimotor cortex is increased following amputation and reduced after mirror therapy
Phantom limb pain (PLP) following amputation, which is experienced by the vast majority of amputees, has been reported to be relieved with daily sessions of mirror therapy. During each session, a mirror is used to view the reflected image of the intact limb moving, providing visual feedback consistent with the movement of the missing/phantom limb. To investigate potential neural correlates of the treatment effect, we measured brain responses in volunteers with unilateral leg amputation using functional magnetic resonance imaging (fMRI) during a four-week course of mirror therapy. Mirror therapy commenced immediately following baseline scans, which were repeated after approximately two and four week intervals. We focused on responses in the region of sensorimotor cortex corresponding to primary somatosensory and motor representations of the missing leg. At baseline, prior to starting therapy, we found a strong and unexpected response in sensorimotor cortex of amputees to visually presented images of limbs. This response was stronger for images of feet compared to hands and there was no such response in matched controls. Further, this response to visually presented limbs was no longer present at the end of the four week mirror therapy treatment, when perceived phantom limb pain was also reduced. A similar pattern of results was also observed in extrastriate and parietal regions typically responsive to viewing hand actions, but not in regions corresponding to secondary somatosensory cortex. Finally, there was a significant correlation between initial visual responsiveness in sensorimotor cortex and reduction in PLP suggesting a potential marker for predicting efficacy of mirror therapy. Thus, enhanced visual responsiveness in sensorimotor cortex is associated with PLP and modulated over the course of mirror therapy.






