Summary: A new study reveals functional changes occur among sensitive and motor brain regions following amputation. The findings shed new light on why some people feel phantom limb sensations following the loss of a limb.
Source: D’Or Institute for Research and Education.
After a limb amputation, brain areas responsible for movement and sensation alter their functional communication. This is the conclusion of a new study published today in Scientific Reports. According to the authors, from the D’Or Institute for Research and Education (IDOR) and Federal University of Rio de Janeiro (UFRJ), the findings may help to understand why some patients report phantom sensations and others do not.
Entitled “Lower limb amputees undergo long-distance plasticity in sensorimotor functional connectivity”, the study represents a step forward a complete comprehension of a phenomenon called brain plasticity, which means the brain’s ability to change itself in response to daily life situations. This ability is greater during the early stages of development but is still critical for learning, memory and behavior throughout our whole life. Investigating the underpinnings of brain plasticity is the key to develop new treatments against mental disorders.
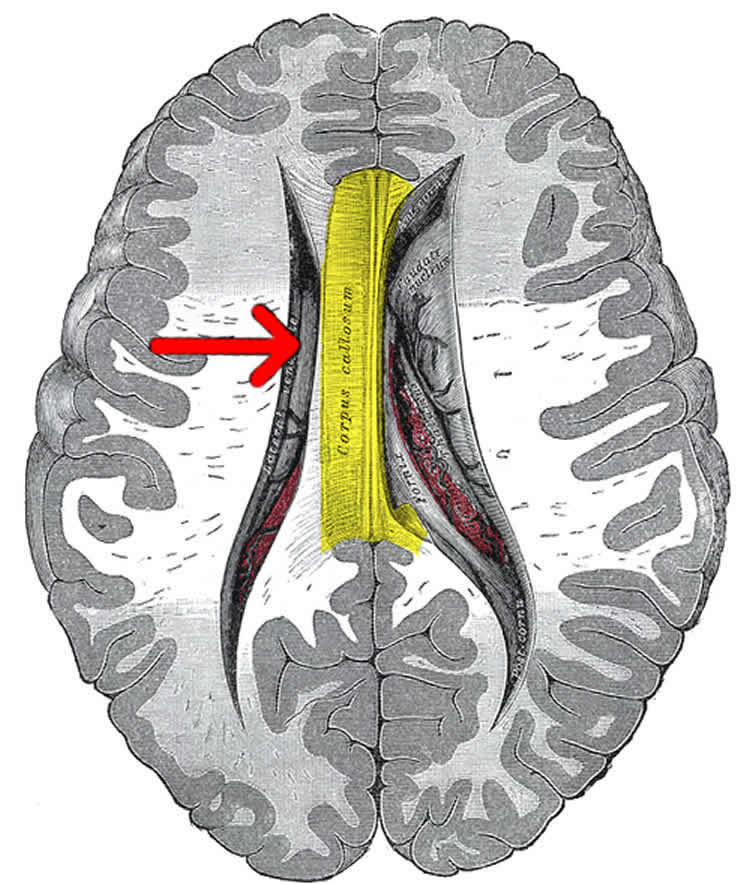
In order to go deeper on that, neuroscientists from Brazil decided to investigate the brain after lower limb amputation. In a previous study from the group, a magnetic resonance imaging experiment revealed that the brain overreacts when the stump is touched. Also, they found that the corpus callosum – brain structure that connects cortical areas responsible for movement and sensations – loses its strength. These findings have raised curiosity about what would be the impact of an impaired corpus callosum on the cortical areas it connects.
Led by Fernanda Tovar-Moll, radiologist and president at IDOR, researchers investigated the differences in functional connectivity (i.e. the communication of brain areas) among motor and sensitive areas connected by the corpus callosum in nine lower limb amputees and nine healthy volunteers.
The results showed that authors’ idea was correct: in response to the touch on the stump, sensitive and motor areas of patients’ brains exhibited an abnormal pattern of communication among the right and left hemispheres, probably as a consequence of impaired corpus callosum. In addition, sensitive and motor areas of the same hemisphere showed increased functional communication in amputees.
“The brain changes in response to amputation have been investigated for years in those patients who report the phantom limb pain. However, our findings show that there is a functional imbalance even in the absence of pain, in patients reporting only phantom sensations”, explains Ivanei Bramati, medical physicist and Ph.D. student at IDOR.
According to the authors, understanding the changes of neural networks in response to the amputation can pave the way for the development of new technologies and devices to treat this disorder and offer patients a better quality of life.
Funding: The work was supported by the National Institute of Translational Neuroscience (INNT), National Council for Scientific and Technological Development (CNPq), Rio de Janeiro Foundation for the Support of Science (FAPERJ), CAPES Foundation..
Source: Catarina Chagas – D’Or Institute for Research and Education
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is in the public domain.
Original Research: Open access research for “Lower limb amputees undergo long-distance plasticity in sensorimotor functional connectivity” by Ivanei E. Bramati, Erika C. Rodrigues, Elington L. Simões, Bruno Melo, Sebastian Höfle, Jorge Moll, Roberto Lent & Fernanda Tovar-Moll in Scientific Reports. Published February 21 2019.
doi:10.1038/s41598-019-39696-z
[cbtabs][cbtab title=”MLA”]D’Or Institute for Research and Education”Phantom Limb Sensation Explained.” NeuroscienceNews. NeuroscienceNews, 22 February 2019.
<https://neurosciencenews.com/phantom-limb-sensation-10794/>.[/cbtab][cbtab title=”APA”]D’Or Institute for Research and Education(2019, February 22). Phantom Limb Sensation Explained. NeuroscienceNews. Retrieved February 22, 2019 from https://neurosciencenews.com/phantom-limb-sensation-10794/[/cbtab][cbtab title=”Chicago”]D’Or Institute for Research and Education”Phantom Limb Sensation Explained.” https://neurosciencenews.com/phantom-limb-sensation-10794/ (accessed February 22, 2019).[/cbtab][/cbtabs]
Abstract
Lower limb amputees undergo long-distance plasticity in sensorimotor functional connectivity
Amputation in adults is associated with an extensive remapping of cortical topography in primary and secondary sensorimotor areas. Here, we used tactile residual limb stimulation and 3T functional magnetic resonance imaging in humans to investigate functional connectivity changes in the sensorimotor network of patients with long-term lower limb traumatic amputations with phantom sensation, but without pain. We found a pronounced reduction of inter-hemispheric functional connectivity between homologous sensorimotor cortical regions in amputees, including the primary (S1) and secondary (S2) somatosensory areas, and primary (M1) and secondary (M2) motor areas. We additionally observed an intra-hemispheric increased functional connectivity between primary and secondary somatosensory regions, and between the primary and premotor areas, contralateral to amputation. These functional connectivity changes in specialized small-scale sensory-motor networks improve our understanding of the functional impact of lower limb amputation in the brain. Our findings in a selective group of patients with phantom limb sensations, but without pain suggest that disinhibition of neural inputs following traumatic limb amputation disrupts sensorimotor topology, unbalancing functional brain network organization. These findings step up the description of brain plasticity related with phantom sensations by showing that pain is not critical for sensorimotor network changes after peripheral injury.






