Augmented microscopy technology invented at the University of Arizona will help surgeons operate with more precision.
Researchers at the University of Arizona have invented a device that for the first time allows neurosurgeons, who use microscopes extensively while operating, to see blood flowing inside vessels and more clearly distinguish cancerous from healthy tissue under the microscope.
Called augmented microscopy, the technology gives surgeons a much more detailed picture in real time and helps them stay on course in surgeries where being off two millimeters could cause paralysis, blindness and even death. And surgeons get this better view without having to learn new technical skills or adapt to changes in the operating room.
“When we started developing this technology, we thought of it like a Google map of a surgical view, providing layers of pertinent information in real time,” said Marek Romanowski, UA associate professor of biomedical engineering. “Our augmented technology provides diagnostic information under the microscope on demand and in color, appearing directly over tissue a surgeon is operating on — as if the tissue was painted to help direct the surgeon’s work.”
A Better View
The new technology overlays an actual, or bright field, image a surgeon sees under a microscope with an electronically processed image using near-infrared fluorescence. NIR fluorescence is a computer-generated imaging technology in which contrast agents are injected in patients to illuminate vital diagnostic information and help surgeons avoid cutting the wrong vessel or removing healthy tissue.
Most neurosurgeons must look up from a surgical microscope, or stereomicroscope, to view fluorescence on a display monitor. If they have a microscope adapted to project fluorescence, it switches back and forth between the real and electronic views, the surgeons’ field of vision momentarily fading to black in between.
Further, the fluorescence shows only contrast in black and white, not anatomical structures or their spatial relationships. So surgeons must visualize how fluorescence lines up with the anatomical structures they see under the microscope.
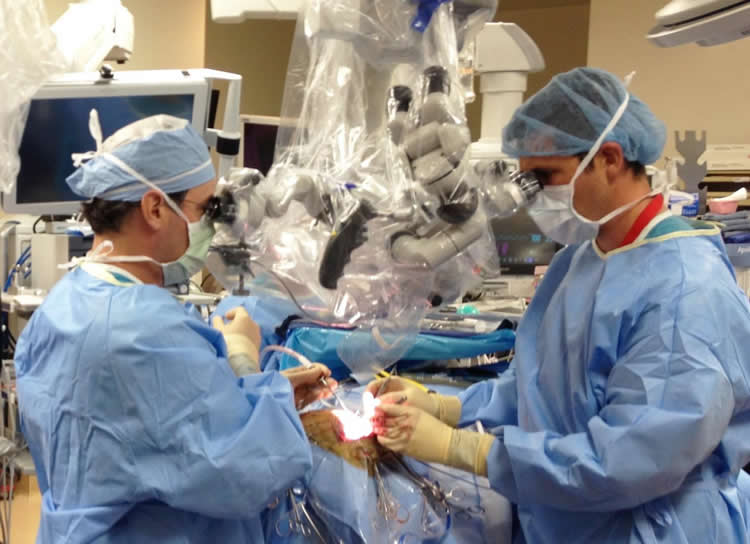
Doctoral student Jeffrey Watson, left, and associate professor Marek Romanowski assemble parts for the prototype microscopy device. Doctoral student Jeffrey Watson, left, and associate professor Marek Romanowski assemble parts for the prototype microscopy device.
The new add-on technology developed at the UA removes such interruptions or guesswork by showing surgeons real and fluorescence images simultaneously and in one location.
Romanowski describes the invention with lead author Jeffrey Watson, a biomedical engineering doctoral student in the UA Graduate Interdisciplinary Program in Biomedical Engineering; G. Michael Lemole Jr., MD, chief of the division of neurosurgery in the department of surgery at the UA College of Medicine-Tucson; and UA neurosurgery resident Nikolay Martirosyan, MD, in “Augmented microscopy: Real-time overlay of bright-field and near-infrared fluorescence images,” published in the Oct. 2015 edition of the SPIE Journal of Biomedical Optics.
“Surgeons need more information than can be provided by stereomicroscopes alone,” said Jennifer Barton, a UA professor of biomedical engineering and interim director of the UA BIO5 Institute, who specializes in cancer imaging. “Dr. Romanowski’s augmented microscopy technology provides critical functional information that can improve surgical accuracy and efficiency.”
The new device, a small box fitted inside a surgical microscope, combines electronic circuitry and optical technologies to superimpose the fluorescence image on the real one and send the augmented view up through the microscope’s right eyepiece to the surgeon.
Lemole, a former flight surgeon in the Air Force Reserve, likens the technology to the head-up display in an airplane cockpit.
“If you can place your critical gauges directly in the pilot’s line of sight, they don’t need to look in a different direction while performing critical maneuvers. It won’t change the way they fly the plane, but it gives them more information, without distraction.”
Promise for Brain Cancer and Aneurysm Patients
Perhaps the most valuable application for augmented microscopy is treating brain cancer, said Romanowski, who holds appointments with the University of Arizona Cancer Center and BIO5 Institute.
More than 20,000 new cases of primary brain cancer are diagnosed in the United States each year, and each year nearly 16,000 patients die from the disease, Romanowski said. Of the half-million patients who die of any other cancer, up to a third has some form of cancer spreading to the brain.
“Brain cancer is especially difficult to remove,” he said. “Current surgical microscopes limit how much of the cancer tissue surgeons can see and how precisely they can determine its boundaries.”
Lemole, a skull base neurosurgeon, routinely operates on brain cancer patients, manipulating vessels the width of a pin to remove malignant tumors. He walks a fine line to remove all of the cancer without removing healthy tissue.
“Aggressive resection is associated with the risk of removing normal brain tissue and impairing functions of the patient,” he and his co-authors write in the Journal of Biomedical Optics. “On the other hand, incomplete resection of tumor results in its immediate relapse in 90 percent of patients. Intraoperative NIR imaging may aid in resection of these challenging tumors.”
Augmented microscopy also holds promise for aneurysm, a bulging of an artery caused by weakened arterial walls. Neurosurgeons treat aneurysm by sealing it off from connecting vessels to prevent a rupture. Nearly half the patients with ruptured aneurysms die, Lemole said, and at least half the survivors have major mobility and other problems.
Augmented technology could improve aneurysm patients’ prognosis, by giving surgeons real-time feedback on every delicate and potentially deadly surgical maneuver they make.
“When I pick up and clip a vessel, I like to see the implications of what happens in that very moment,” he said.
Funding: This research was supported by the National Cancer Institute of the National Institutes of Health under Grant No. CA120350 and by the National Heart, Lung and Blood Institute of the National Institutes of Health under Grant No. HL007955.
Source: Pete Brown – University of Arizona
Image Source: The image is credited to Nikolay Martirosyan, MD.
Original Research: Abstract for “Augmented microscopy: real-time overlay of bright-field and near-infrared fluorescence images” by Jeffrey R. Watson; Christian F. Gainer; Nikolay Martirosyan; Jesse Skoch; G. Michael Lemole, Jr.; Rein Anton; and Marek Romanowski in Journal of Biomedical Optics. Published online October 6 2015 doi:10.1117/1.JBO.20.10.106002
Abstract
Augmented microscopy: real-time overlay of bright-field and near-infrared fluorescence images
Intraoperative applications of near-infrared (NIR) fluorescent contrast agents can be aided by instrumentation capable of merging the view of surgical field with that of NIR fluorescence. We demonstrate augmented microscopy, an intraoperative imaging technique in which bright-field (real) and electronically processed NIR fluorescence (synthetic) images are merged within the optical path of a stereomicroscope. Under luminance of 100,000 lx, representing typical illumination of the surgical field, the augmented microscope detects 189 nM concentration of indocyanine green and produces a composite of the real and synthetic images within the eyepiece of the microscope at 20 fps. Augmentation described here can be implemented as an add-on module to visualize NIR contrast agents, laser beams, or various types of electronic data within the surgical microscopes commonly used in neurosurgical, cerebrovascular, otolaryngological, and ophthalmic procedures.
“Augmented microscopy: real-time overlay of bright-field and near-infrared fluorescence images” by Jeffrey R. Watson; Christian F. Gainer; Nikolay Martirosyan; Jesse Skoch; G. Michael Lemole, Jr.; Rein Anton; and Marek Romanowski in Journal of Biomedical Optics. Published online October 6 2015 doi:10.1117/1.JBO.20.10.106002