Summary: A new study links obesity in early adulthood with an increased risk of developing multiple sclerosis later in life.
Source: PLOS.
Individuals who are obese in early adulthood face a heightened risk of developing multiple sclerosis (MS), according to new research conducted by Dr. Brent Richards of the Lady Davis Institute at the Jewish General Hospital, Quebec, Canada and colleagues, published in PLOS Medicine. This result provides further confirmation of previous observational studies that had suggested the existence of such a link.
MS is a progressive neurological disorder which can lead to disability and death, involving damage to the myelin which surrounds nerves in the spinal cord and brain. Causes of the disease are poorly understood, although immune-mediated mechanisms are likely. Currently available treatments have only modest effects on the disease and its symptoms, which underlines the importance of identifying preventive measures.
The team, comprised of researchers in Canada and the UK, and led by Lauren Mokry, carried out a Mendelian randomization study in large population datasets to investigate whether genetically determined obesity was associated with increased risk of MS. Such a study decreases the probability that exposures linked to obesity, such as smoking, can explain the findings. They found that a change in body mass index from overweight to obese (equivalent to an average size adult woman increasing in weight from 150 to 180 pounds) was associated with an increase of about 40% in the risk of MS.
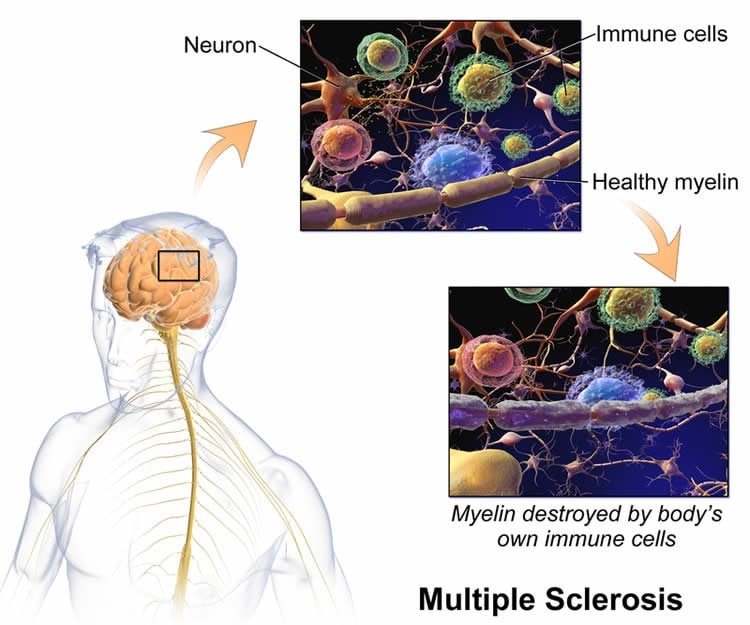
“These findings may carry important public health implications because of the high prevalence of obesity in many countries” note the authors in their research article; “[because the] median age of onset for MS is 28-31 years … [these findings should provide motivation] to combat increasing youth obesity rates by implementing community and school-based interventions that promote physical activity and nutrition.”
In a Perspective discussing the research, Alberto Ascherio and Kassandra L. Munger note that, factoring in earlier research, Richards and colleagues’ study “suggest[s] that obesity in early life is indeed causally related to multiple sclerosis risk and provide[s] a further rationale for obesity prevention.”
Funding: JBR and LEM are supported by the Canadian Institute of Health Research. JBR is supported by Fonds de la recherche en sante du Quebec (FRSQ) and Merck. NJT and GDS work within the Medical Research Council Integrative Epidemiology Unit at the University of Bristol (MC_UU_12013/1&3). SS is supported by the Cambridge NIHR Biomedical Research Centre. The funders played no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Competing Interests: GDS is a member of the Editorial Board of PLOS Medicine. The other authors declare that no competing interests exist.
Source: PLOS
Image Source: This NeuroscienceNews.com image is credited to BruceBlaus and is licensed CC BY SA 4.0.
Original Research: Full open access research for for “Obesity and Multiple Sclerosis: A Mendelian Randomization Study” by Lauren E. Mokry, Stephanie Ross, Nicholas J. Timpson, Stephen Sawcer, George Davey Smith, and J. Brent Richards in PLOS Medicine. Published online June 28 2016 doi:10.1371/journal.pmed.1002053
[cbtabs][cbtab title=”MLA”]PLOS. “Obesity Linked to Increased Risk of Multiple Sclerosis.” NeuroscienceNews. NeuroscienceNews, 28 June 2016.
<https://neurosciencenews.com/multiple-sclerosis-obesity-4590/>.[/cbtab][cbtab title=”APA”]PLOS. (2016, June 28). Obesity Linked to Increased Risk of Multiple Sclerosis. NeuroscienceNews. Retrieved June 28, 2016 from https://neurosciencenews.com/multiple-sclerosis-obesity-4590/[/cbtab][cbtab title=”Chicago”]PLOS. “Obesity Linked to Increased Risk of Multiple Sclerosis.” https://neurosciencenews.com/multiple-sclerosis-obesity-4590/ (accessed June 28, 2016).[/cbtab][/cbtabs]
Abstract
Obesity and Multiple Sclerosis: A Mendelian Randomization Study
Background
Observational studies have reported an association between obesity, as measured by elevated body mass index (BMI), in early adulthood and risk of multiple sclerosis (MS). However, bias potentially introduced by confounding and reverse causation may have influenced these findings. Therefore, we elected to perform Mendelian randomization (MR) analyses to evaluate whether genetically increased BMI is associated with an increased risk of MS.
Methods and Findings
Employing a two-sample MR approach, we used summary statistics from the Genetic Investigation of Anthropometric Traits (GIANT) consortium and the International MS Genetics Consortium (IMSGC), the largest genome-wide association studies for BMI and MS, respectively (GIANT: n = 322,105; IMSGC: n = 14,498 cases and 24,091 controls). Seventy single nucleotide polymorphisms (SNPs) were genome-wide significant (p < 5 x 10−8) for BMI in GIANT (n = 322,105) and were investigated for their association with MS risk in the IMSGC. The effect of each SNP on MS was weighted by its effect on BMI, and estimates were pooled to provide a summary measure for the effect of increased BMI upon risk of MS. Our results suggest that increased BMI influences MS susceptibility, where a 1 standard deviation increase in genetically determined BMI (kg/m2) increased odds of MS by 41% (odds ratio [OR]: 1.41, 95% CI 1.20–1.66, p = 2.7 x 10−5, I2 = 0%, 95% CI 0–29). Sensitivity analyses, including MR-Egger regression, and the weighted median approach provided no evidence of pleiotropic effects. The main study limitations are that, while these sensitivity analyses reduce the possibility that pleiotropy influenced our results, residual pleiotropy is difficult to exclude entirely. Conclusion
Genetically elevated BMI is associated with risk of MS, providing evidence for a causal role for obesity in MS etiology. While obesity has been associated with many late-life outcomes, these findings suggest an important consequence of childhood and/or early adulthood obesity.
“Obesity and Multiple Sclerosis: A Mendelian Randomization Study” by Lauren E. Mokry, Stephanie Ross, Nicholas J. Timpson, Stephen Sawcer, George Davey Smith, and J. Brent Richards in PLOS Medicine. Published online June 28 2016 doi:10.1371/journal.pmed.1002053