Summary: Why does Alzheimer’s disease (AD) destroy some neurons while leaving others nearby completely untouched? With a major five-year grant from the NIH, researchers are building a “multiscale” digital model of the hippocampus to solve this mystery.
The team is creating a virtual testbed that connects the dots between microscopic gene activity and large-scale memory networks. This model allows scientists to simulate the progression of the disease in a way that is impossible in living patients, helping them identify the exact “tipping points” where memory circuits begin to fail.
Key Facts
- Multiscale Modeling: The project links three levels of biology: individual cells (molecular), local circuits (3D reconstruction), and whole-brain networks (fMRI-scale modeling).
- The Vulnerability Mystery: AD is not uniform. The study aims to find out why specific hippocampal neurons deteriorate rapidly while others remain resilient, focusing on gene expression changes that precede cell death.
- The “Virtual Testbed”: Researchers can use the model to virtually test new drugs or interventions to see if protecting a specific cell type can stabilize the entire memory network before irreversible damage occurs.
- Precision Neuroscience: By analyzing both mouse models and donated human brain tissue, the team is building on the Hippocampus Gene Expression Atlas (HGEA) to create a high-resolution map of disease progression.
- Open Science: All computational models and data generated by the study will be made openly available to the global scientific community to accelerate Alzheimer’s research.
Source: USC
With a new model of the brain region essential to memory formation, from cells to whole-brain networks, the team hopes to identify critical changes in the progression of Alzheimer’s disease that could point the way to earlier, more effective treatments.
A team of researchers at the USC Mark and Mary Stevens Neuroimaging and Informatics Institute (Stevens INI) at the Keck School of Medicine of USC has received a major grant from the National Institutes of Health to investigate a long-standing mystery in Alzheimer’s disease (AD): how does the loss of specific neurons in the hippocampus lead to the cognitive impairment seen in patients with AD?
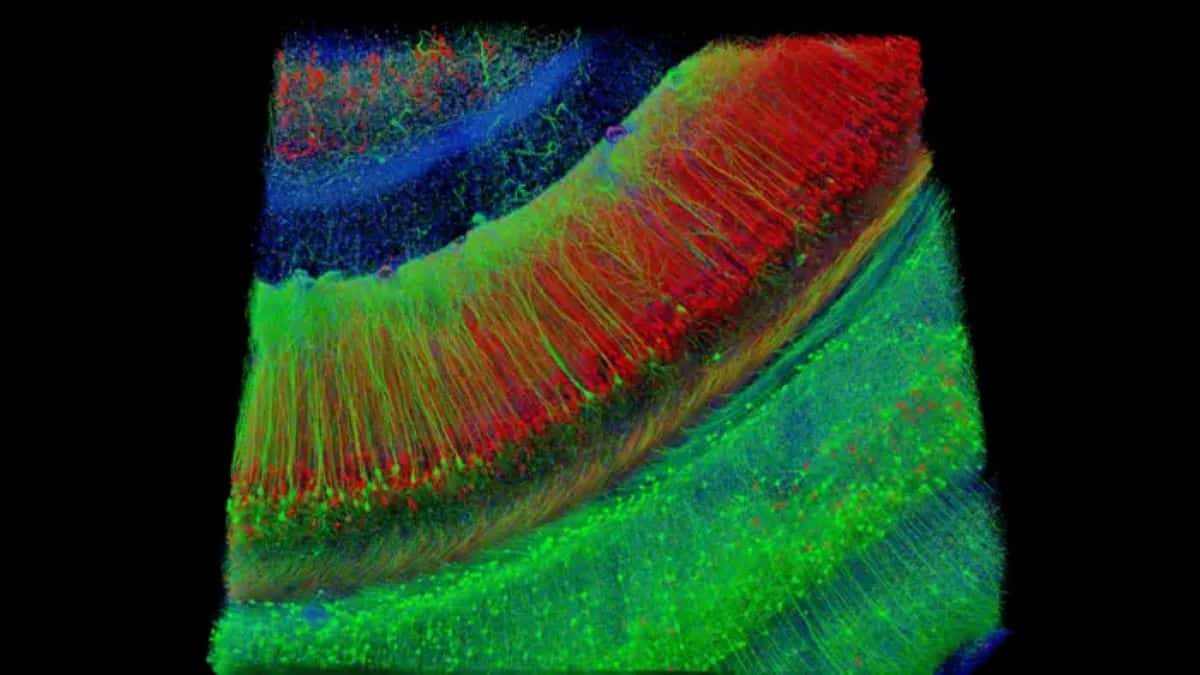
Led by Michael S. Bienkowski, PhD, an assistant professor of physiology and neuroscience and of biomedical engineering at the Keck School of Medicine, the five-year NIH R01 award will support the development of a powerful new cell type-specific multiscale model of the hippocampus, a brain region essential for memory formation that is among the first areas affected by AD.
A multiscale model is a way to connect information across different “levels” of the brain, from tiny details like cells and circuits to larger regions and whole-brain networks, so researchers can see how changes at one level affect the others.
AD affects more than 6 million Americans, a number expected to nearly double by 2050. Although the buildup of toxic proteins such as amyloid and tau is a hallmark of the disease, these changes do not damage all neurons equally. Understanding how specific cell types change over the course of the disease could reveal the circuits underlying cognitive impairment and dementia and identify new targets for earlier, more effective interventions.
“Alzheimer’s doesn’t damage the brain uniformly,” said Bienkowski. “Even within the same brain region, some neurons deteriorate rapidly while others remain relatively intact. This project is designed to model how cellular and molecular changes to these neurons and their connections begin to disrupt the hippocampal network and lead to dysfunction.”
The research builds on Bienkowski’s earlier work developing the Hippocampus Gene Expression Atlas(HGEA), a detailed map that defines distinct hippocampal neuron populations based on their gene activity and wiring patterns.
Using this framework, the new study will combine cutting-edge molecular imaging, 3D circuit reconstruction, and advanced computational modeling to gain an understanding of the functional consequences of how Alzheimer’s-relatedchanges unfold over time.
The research team includes two members of the USC Institute for Technology and Medical Systems (ITEMS), Gianluca Lazzi, PhD, and Jean-Marie Bouteiller, PhD, whose world-class expertise in computational modeling of the hippocampus and retina is integral to the study.
Together, the team will analyze both mouse models of AD and donated human brain tissue to identify cell types that show early signs of stress, altered gene activity, or structural damage before neurons die. These findings will then be integrated into a multiscale model that simulates how the progressive loss or disconnection of specific neurons disrupts memory-related brain networks.
“This multiscale approach allows us to connect changes that occur in different parts of the hippocampus at different progressive timepoints” said Bienkowski. “It’s a way to study Alzheimer’s disease mechanisms at different scales that simply isn’t possible in living patients and provides a virtual testbed for safely and rapidly evaluating new disease treatment targets.”
A key innovation of the project is its ability to virtually test how protecting or restoring specific neuron types might stabilize memory-related brain networks. By simulating AD progression across multiple stages, the model could help researchers identify the most critical tipping points in disease progression and prioritize therapeutic strategies before irreversible damage occurs.
Arthur W. Toga, PhD, director of the Stevens INI and the Ghada Irani Chair in Neuroscience at the Keck School of Medicine of USC, said the project reflects a broader shift in AD research toward precision neuroscience.
“This work demonstrates how integrating large-scale data, advanced imaging, and computational modeling can transform our understanding of neurodegenerative disease,” Toga said.
“By revealing brain circuits and cells at a level of detail that cannot be captured in living humans, this kind of cellular-scale research complements in vivo studies and helps connect what we see in patients to the underlying biology. By pinpointing which neurons matter most and when they become vulnerable, this research lays essential groundwork for more targeted and effective treatments.”
All computational models and methodological advances developed through the project will be made openly available to the scientific community, thereby maximizing the impact of the NIH investment and accelerating progress across the field.
Key Questions Answered:
A: The hippocampus is the brain’s “memory gateway.” It’s one of the first areas hit by Alzheimer’s, but it’s also incredibly complex. By mastering a model of this specific region from the cellular level up, researchers can understand the “blueprint” of how the disease breaks memory before it spreads to the rest of the brain.
A: You can’t safely test experimental treatments on a living person’s specific hippocampal circuits, nor can you see their individual neurons in real-time. This model acts like a “flight simulator” for Alzheimer’s, allowing scientists to crash the system, restart it, and test “what-if” scenarios to see which cells are most vital for saving a patient’s memory.
A: Brain networks are resilient; they can often handle the loss of a few neurons. However, there is a critical point where enough connections are lost that the whole system collapses—this is when symptoms like dementia appear. The goal is to find the exact moment before that collapse so we can intervene when the brain is still salvageable.
Editorial Notes:
- This article was edited by a Neuroscience News editor.
- Journal paper reviewed in full.
- Additional context added by our staff.
About this Alzheimer’s disease research news
Author: Laura LeBlanc
Source: USC
Contact: Laura LeBlanc – USC
Image: The image is credited to Stevens INI