Summary: Researchers implicate a brain region called the paracingulate sulcus in the experience of hallucinations. The findings shed light into why some people are more likely to hallucinate than others, and provides a new target for treatment aimed at reducing the experience.
Source: The Conversation.
Imagine hearing a voice that screams, “You’re no good at this and you’re going to fail every exam” but not knowing where it came from. Or suddenly seeing a poisonous snake slithering towards you. Even if you’ve never had a hallucination – a sensory event that is experienced as real, despite having no material world cause – it’s easy to imagine how frightening they can be.
Despite advances in brain imaging technology, we still have a limited understanding of the biological processes behind hallucinations. But new research has discovered that a key region of the brain, the paracingulate sulcus, may underlie the experience. This delivers a glimmer of insight into why some people are more likely to hallucinate and provides a neural target for treatments that aim to tackle such terrifying experiences.
When someone has a hallucination, the basic problem is that they fail to distinguish between real events and those created by the imagination. As a result, hallucinations have been described as an impairment in “reality monitoring”.
Imagination centre
Recent studies that have taken images of the brain using functional Magnetic Resonance Imaging (fMRI) have shown there is an area of the frontal lobe particularly related to imagination. The outer layer of tissue (cortex) around a fold (sulcus) in the brain known as the paracingulate activates when you imagine yourself in a future scenario or imagine what others are thinking or feeling. We also know from studying patients with brain damage that the frontal lobe in general is important for complex human behaviours, such as planning and our sense of self.
The key role played by the paracingulate sulcus area in imagination suggests that it is also involved in reality monitoring. If this part of the brain functions poorly then it might influence your ability to differentiate reality from imagination – and so increase the likelihood that you could experience hallucinations.
To test this theory, Jane Garrison and her colleagues at the University of Cambridge, undertook a large-scale study of paracingulate sulcus anatomy. This particular brain fold can look very different in different people: in some brains, it is long and uninterrupted; in others, it is short and broken up – and some people have virtually no paracingulate sulcus at all.
Longer folds actually mean there is less brain cell-carrying grey matter tissue in the area. Other individual differences in sulcus anatomy can also affect the connections to the rest of the brain through the white matter tissue that carries neural signals. These structural variations can affect the local processing that takes place in a brain region.
The researchers measured the paracingulate sulcus length of three groups of people using structural MRI brain scans: schizophrenic patients who experienced hallucinations, schizophrenics who did not, and a control group of healthy individuals. Remarkably, those patients who experienced hallucinations had significantly reduced paracingulate sulcus length compared to those patients who had no hallucinations.
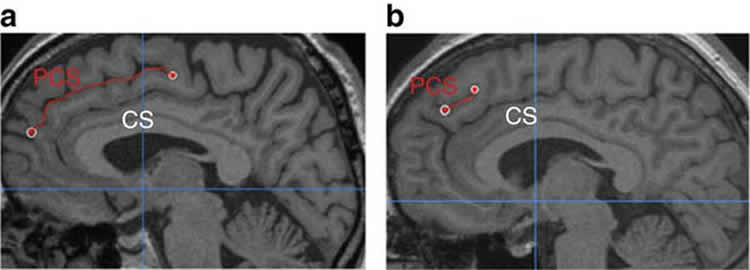
Analyses indicated that a reduction in sulcus length by 1cm led to an increased likelihood of experiencing hallucinations of nearly 20%. Plus, sulcus length did not differ between the schizophrenics without hallucinations and the control individuals. This suggests that sulcus length specifically relates to the experience of hallucinations rather than schizophrenia more generally.
Shedding light on schizophrenia
Interestingly, a shorter paracingulate sulcus was also more likely no matter what kind of hallucinations the patients suffered, whether they heard voices, saw images, felt touches, or smelt odours that weren’t real. This links the region to hallucinatory experience in general, rather than specific problems with, for example, visual or aural perception.
This study doesn’t just shed light on why some patients with schizophrenia might experience hallucinations while others might not. It also tells us more fundamentally about the neural basis for the hallucinatory process. In understanding what makes some people more likely to experience hallucinations, we begin to appreciate the anatomical features of the brain that underpin our experience of self and human consciousness.
The result is that the paracingulate sulcus may become an important target in new brain therapies that aim to tackle local regions of dysfunction. Techniques such as transcranial magnetic stimulation, in which an electromagnetic field is placed just above the scalp and then disturbed, have the power to safely change activity levels in cortical brain areas. Now, researchers hoping to improve the lives of hallucination sufferers have an area pinpointed on the cortical map from where to start.
Source: Charlotte Rae – The Conversation
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Garrison et al, Nature Communications.
[cbtabs][cbtab title=”MLA”]The Conversation”Hallucinations May Be Caused By a Fold in the Brain.” NeuroscienceNews. NeuroscienceNews, 4 January 2019.
<https://neurosciencenews.com/hallucinations-paracinuglate-sulcus-10435/>.[/cbtab][cbtab title=”APA”]The Conversation(2019, January 4). Hallucinations May Be Caused By a Fold in the Brain. NeuroscienceNews. Retrieved January 4, 2019 from https://neurosciencenews.com/hallucinations-paracinuglate-sulcus-10435/[/cbtab][cbtab title=”Chicago”]The Conversation”Hallucinations May Be Caused By a Fold in the Brain.” https://neurosciencenews.com/hallucinations-paracinuglate-sulcus-10435/ (accessed January 4, 2019).[/cbtab][/cbtabs]






