Summary: Functional connectivity problems associated with temporal lobe epilepsy appear to improve after surgery.
Source: Vanderbilt University
Successful epilepsy surgery can improve brain connectivity similar to patterns seen in people without epilepsy, according to a new study published in the journal Neurosurgery.
The Vanderbilt University Medical Center (VUMC) study of 15 people with temporal lobe epilepsy is the first to show improvements in brain networks after surgery compared to a group of healthy subjects.
Brain networks involved in the study are important for keeping the brain awake and alert, according to senior author Dario Englot, MD, PhD, surgical director of VUMC’s Epilepsy Program.
“It’s important to realize that, over time, seizures lead to brain network problems which may be related to cognitive deficits seen in patients with epilepsy,” said Englot.
“Our new results show some brain network activity can improve with surgery if you stop the seizures.”
Over 3 million people in the U.S., or roughly 1 percent, have epilepsy. Nearly one-third of people with epilepsy have bad seizures despite taking medication, leading to a reduced quality of life with a persistent risk of injury and limitations on mobility, socializing and working.
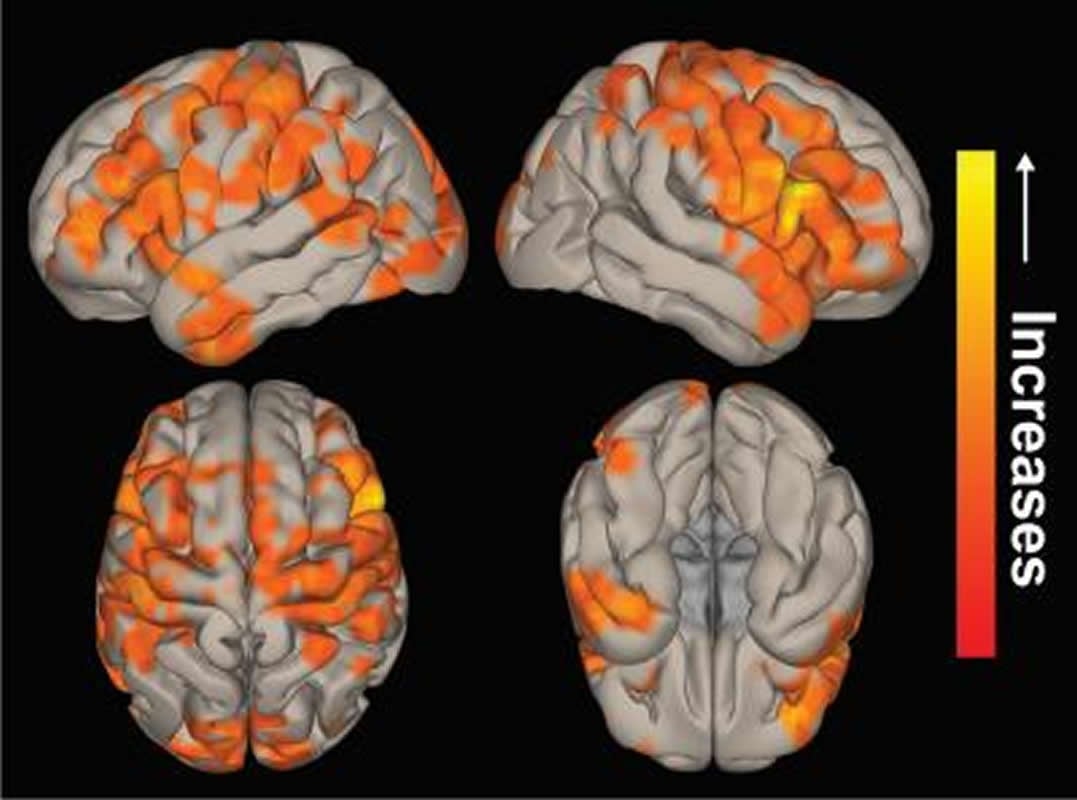
“We know that the patients can have large decreases in neural connectivity due to chronic seizures, but what’s surprising in these results is that the connectivity can improve after surgery to levels very similar to healthy control subjects,” said first author Hernán González, an MD/PhD candidate at Vanderbilt University School of Medicine.
A previous Vanderbilt study showed that, although seizures start in the temporal lobe, epilepsy can affect connections in distant brain regions, including the brainstem. These findings highlight possible reasons for unexplained cognitive problems, such as difficulty with attention and concentration. Both studies were done in collaboration with Victoria Morgan, PhD, associate professor of Radiology.
A future study will examine whether patients see improvement in their cognition and quality of life that accompanies the recovery of brain connectivity after surgery.
“Surgery is an underutilized treatment for people who continue to have seizures despite trialing multiple medications,” said Englot. “Early surgery can help improve quality of life for epilepsy patients, and now we are learning that surgery may lead to changes in brain networks.”
The epilepsy monitoring units at VUMC have eight adult beds and four pediatric beds. For adults, VUMC’s Epilepsy Program is the only epilepsy center in Tennessee designated Level 4 by the National Association of Epilepsy Centers — the highest possible level. For children, VUMC is one of the state’s two Level 4 epilepsy centers.
Funding: This work was supported in part by the National Institutes of Health grants R00 NS097618 (DJE), R01 NS075270 (VLM), T32 EB021937 (HJFG), and T32 GM07347 (HJFG).
Source:
Vanderbilt University
Media Contacts:
Craig Boerner – Vanderbilt University
Image Source:
The image is credited to Vanderbilt University Medical Center.
Original Research: Closed access
“Brainstem Functional Connectivity Disturbances in Epilepsy may Recover After Successful Surgery “. Hernán F J González, MS; Sarah E Goodale, BE; Monica L Jacobs, PsyD; Kevin F Haas, MD, PhD; Bennett A Landman, PhD; Victoria L Morgan, PhD; and Dario J Englot, MD, PhD.
Neurosurgery. doi:10.1093/neuros/nyz128
Abstract
Brainstem Functional Connectivity Disturbances in Epilepsy may Recover After Successful Surgery
BACKGROUND
Focal seizures in temporal lobe epilepsy (TLE) are associated with widespread brain network perturbations and neurocognitive problems.
OBJECTIVE
To determine whether brainstem connectivity disturbances improve with successful epilepsy surgery, as recent work has demonstrated decreased brainstem connectivity in TLE that is related to disease severity and neurocognitive profile.
METHODS
We evaluated 15 adult TLE patients before and after (>1 yr; mean, 3.4 yr) surgery, and 15 matched control subjects using magnetic resonance imaging to measure functional and structural connectivity of ascending reticular activating system (ARAS) structures, including cuneiform/subcuneiform nuclei (CSC), pedunculopontine nucleus (PPN), and ventral tegmental area (VTA).
RESULTS
TLE patients who achieved long-term postoperative seizure freedom (10 of 15) demonstrated increases in functional connectivity between ARAS structures and fronto-parietal-insular neocortex compared to preoperative baseline (P = .01, Kruskal–Wallis), with postoperative connectivity patterns resembling controls’ connectivity. No functional connectivity changes were detected in 5 patients with persistent seizures after surgery (P = .9, Kruskal–Wallis). Among seizure-free postoperative patients, larger increases in CSC, PPN, and VTA functional connectivity were observed in individuals with more frequent seizures before surgery (P < .05 for each, Spearman's rho). Larger postoperative increases in PPN functional connectivity were seen in patients with lower baseline verbal IQ (P = .03, Spearman's rho) or verbal memory (P = .04, Mann–Whitney U). No changes in ARAS structural connectivity were detected after successful surgery.
CONCLUSION
ARAS functional connectivity disturbances are present in TLE but may recover after successful epilepsy surgery. Larger increases in postoperative connectivity may be seen in individuals with more severe disease at baseline.