People with depressive symptoms should be screened for obstructive sleep apnea.
A new study shows that depressive symptoms are extremely common in people who have obstructive sleep apnea, and these symptoms improve significantly when sleep apnea is treated with continuous positive airway pressure therapy.
Results show that nearly 73 percent of sleep apnea patients (213 of 293 patients) had clinically significant depressive symptoms at baseline, with a similar symptom prevalence between men and women. These symptoms increased progressively and independently with sleep apnea severity.
However, clinically significant depressive symptoms remained in only 4 percent of the sleep apnea patients who adhered to CPAP therapy for 3 months (9 of 228 patients). Of the 41 treatment adherent patients who reported baseline feelings of self-harm or that they would be “better dead,” none reported persisting suicidal thoughts at the 3-month follow-up.
“Effective treatment of obstructive sleep apnea resulted in substantial improvement in depressive symptoms, including suicidal ideation,” said senior author David R. Hillman, MD, clinical professor at the University of Western Australia and sleep physician at the Sir Charles Gairdner Hospital in Perth. “The findings highlight the potential for sleep apnea, a notoriously underdiagnosed condition, to be misdiagnosed as depression.”
Study results are published in the September issue of the Journal of Clinical Sleep Medicine.
The American Academy of Sleep Medicine reports that obstructive sleep apnea (OSA) is a common sleep disease afflicting at least 25 million adults in the U.S. Untreated sleep apnea increases the risk of other chronic health problems including heart disease, high blood pressure, Type 2 diabetes, stroke and depression.
The study group comprised 426 new patients referred to a hospital sleep center for evaluation of suspected sleep apnea, including 243 males and 183 females. Participants had a mean age of 52 years. Depressive symptoms were assessed using the validated Patient Health Questionnaire (PHQ-9), and the presence of obstructive sleep apnea was determined objectively using overnight, in-lab polysomnography. Of the 293 patients who were diagnosed with sleep apnea and prescribed CPAP therapy, 228 were treatment adherent, which was defined as using CPAP therapy for an average of 5 hours or more per night for 3 months.
According to the authors, the results emphasize the importance of screening people with depressive symptoms for obstructive sleep apnea. These patients should be asked about common sleep apnea symptoms including habitual snoring, witnessed breathing pauses, disrupted sleep, and excessive daytime sleepiness.
Funding: The study was supported by a grant from the National Health and Medical Research Council (NHMRC) of Australia.
Source: Lynn Celmer – American Academy of Sleep Medicine
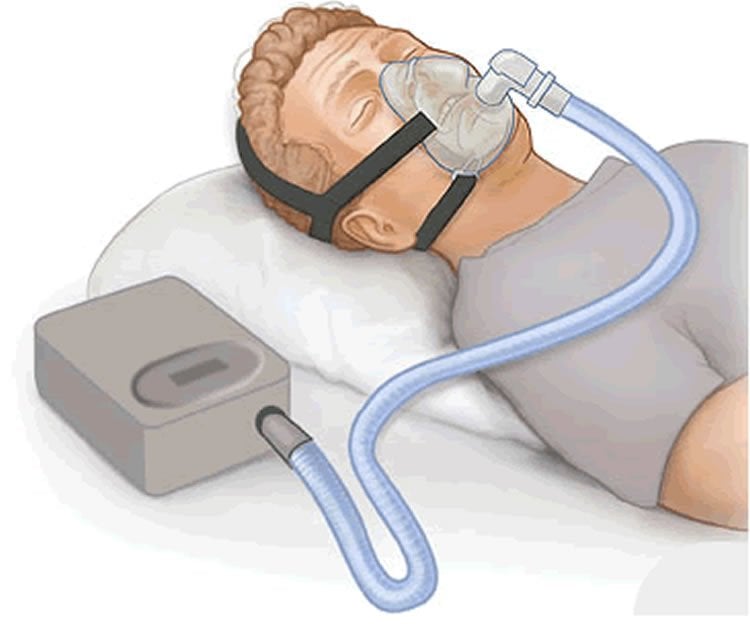
Image Source: The image is credited to PruebasBMA and is licensed CC BY-SA 3.0
Original Research: Abstract for “Depressive Symptoms before and after Treatment of Obstructive Sleep Apnea in Men and Women” by Cass Edwards, BSc; Sutapa Mukherjee, MB, PhD; Laila Simpson, PhD; Lyle J. Palmer, PhD; Osvaldo P. Almeida, MD; and David R. Hillman, MB in Journal of Clinical Sleep Medicine. Published online September 2015 doi:10.5664/jcsm.5020
Abstract
Depressive Symptoms before and after Treatment of Obstructive Sleep Apnea in Men and Women
Study Objectives
To determine prevalence of depressive symptoms in obstructive sleep apnea (OSA) and the impact of OSA treatment on depression scores.
Methods
Consecutive new patients referred for investigation of suspected OSA were approached. Consenting patients completed a patient health questionnaire (PHQ-9) for depressive symptoms when attending for laboratory polysomnography. Those with moderate/severe (apneahypopnea index [AHI] ≥ 15 events/h) and/or symptomatic mild OSA (AHI 5–14.99 events/h) were offered continuous positive airway pressure (CPAP) therapy. PHQ-9 was repeated after 3 months of CPAP with compliance recorded. Of a maximum PHQ-9 score of 27, a cut point ≥ 10 (PHQ-9 ≥ 10) was used to indicate presence of clinically significant depressive symptoms.
Results
A total of 426 participants (243 males) were recruited. Mean ± standard deviation body mass index (BMI) was 32.1 ± 7.1 kg/m2 and AHI 33.6 ± 28.9 events/h. PHQ-9 was 10.5 ± 6.1 and independently related to AHI (p < 0.001) and BMI (p < 0.001). In those without OSA, PHQ-9 ≥ 10 was more common in women, but no gender difference was evident with OSA. Of 293 patients offered CPAP, 228 were compliant (mean nightly use > 5 h) over 3 months of therapy. In them, with therapy, AHI decreased from 46.7 ± 27.4 to 6.5 ± 1.6 events/h, PHQ-9 from 11.3 ± 6.1 to 3.7 ± 2.9 and PHQ-9 ≥ 10 from 74.6% to 3.9% (p < 0.001 in each case). Magnitude of change in PHQ-9 was similar in men and women. Antidepressant use was constant throughout.
Conclusions
Depressive symptoms are common in OSA and related to its severity. They improve markedly with CPAP, implying a relationship to untreated OSA.
“Depressive Symptoms before and after Treatment of Obstructive Sleep Apnea in Men and Women” by Cass Edwards, BSc; Sutapa Mukherjee, MB, PhD; Laila Simpson, PhD; Lyle J. Palmer, PhD; Osvaldo P. Almeida, MD; and David R. Hillman, MB in Journal of Clinical Sleep Medicine. Published online September 2015 doi:10.5664/jcsm.5020






