Summary: A brain network consisting of the thalamus, anterior and posterior cingulate cortex, and angular gyri was implicated in the loss, and return, of consciousness under both anesthetic and natural sleep.
Source: SfN
The loss and return of consciousness is linked to the same network of brain regions for both sleep and anesthesia, according to new research published in Journal of Neuroscience.
The biological basis of consciousness has confounded scientists for centuries. Our experimental techniques falter, as the effects of sleep and anesthetic drugs alter brain activity beyond changes in consciousness.
In addition, behavior does not always reveal someone’s state of consciousness. An unresponsive person might still be aware of their surroundings (connected), or unaware but still experiencing their internal world (disconnected).
Scheinin et al. sought networks associated with human consciousness by measuring the brain activity of adult males with PET as they fell asleep and went under anesthesia. The research team woke participants mid-experiment to interview them and confirm their state of connectedness.
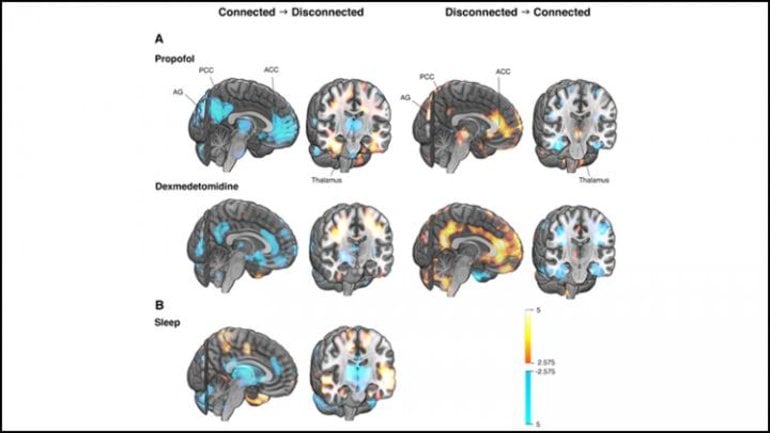
Changes in connectedness corresponded to the activity of a network comprised of regions deep inside the brain: the thalamus, anterior and posterior cingulate cortex, and angular gyri. These regions exhibited less blood flow when a participant lost connectedness and more blood flow when they regained it.
The pattern held true for both sleep and anesthesia, indicating the changes corresponded to connectedness rather than the effects of sleep or drugs, and that the network may be imperative for human consciousness.
About this consciousness research news
Source: SfN
Contact: Calli McMurray – SfN
Image: The image is credited to Scheinin et al., JNeurosci 2020
Original Research: Closed access.
“Foundations of Human Consciousness: Imaging the Twilight Zone” by Annalotta Scheinin, Oskari Kantonen, Michael Alkire, Jaakko Långsjö, Roosa E Kallionpää, Kaike Kaisti, Linda Radek, Jarkko Johansson, Nils Sandman, Mikko Nyman, Mika Scheinin, Tero Vahlberg, Antti Revonsuo, Katja Valliand Harry Scheinin. Journal of Neuroscience
Abstract
Foundations of Human Consciousness: Imaging the Twilight Zone
What happens in the brain when conscious awareness of the surrounding world fades? We manipulated consciousness in two experiments in a group of healthy males and measured brain activity with positron emission tomography. Measurements were made during wakefulness, escalating and constant levels of two anesthetic agents (Experiment 1, n=39) and during sleep-deprived wakefulness and Non-Rapid Eye Movement sleep (Experiment 2, n=37). In Experiment 1, the subjects were randomized to receive either propofol or dexmedetomidine until unresponsiveness. In both experiments, forced awakenings were applied to achieve rapid recovery from an unresponsive to a responsive state, followed by immediate and detailed interviews of subjective experiences during the preceding unresponsive condition. Unresponsiveness rarely denoted unconsciousness, as the majority of the subjects had internally generated experiences. Unresponsive anesthetic states and verified sleep stages, where a subsequent report of mental content included no signs of awareness of the surrounding world, indicated a disconnected state. Functional brain imaging comparing responsive and connected vs.unresponsive and disconnected states of consciousness during constant anesthetic exposure revealed that activity of the thalamus, cingulate cortices and angular gyri are fundamental for human consciousness. These brain structures were affected independent from the pharmacologic agent, drug concentration and direction of change in the state of consciousness. Analogous findings were obtained when consciousness was regulated by physiological sleep. State-specific findings were distinct and separable from the overall effects of the interventions, which included widespread depression of brain activity across cortical areas. These findings identify a central core brain network critical for human consciousness.
SIGNIFICANCE STATEMENT
Trying to understand the biological basis of human consciousness is currently one of the greatest challenges of neuroscience. While the loss and return of consciousness regulated by anesthetic drugs and physiological sleep are employed as model systems in experimental studies on consciousness, previous research results have been confounded by drug effects, by confusing behavioral “unresponsiveness” and internally generated consciousness, and by comparing brain activity levels across states that differ in several other respects than only consciousness. Here, we present carefully designed studies that overcome many previous confounders and for the first time reveal the neural mechanisms underlying human consciousness and its disconnection from behavioral responsiveness, both during anesthesia and during normal sleep, and in the same study subjects.







