For patients who need surgery for facial pain caused by trigeminal neuralgia, the most cost-effective procedure is the least often used, reports a study in the September issue of Neurosurgery, official journal of the Congress of Neurological Surgeons. The journal is published by Lippincott Williams & Wilkins, a part of Wolters Kluwer Health.
Percutaneous stereotaxic rhizotomy (PSR) provides good pain relief at much lower cost than other types of surgical treatments for trigeminal neuralgia, according to the report by Dr. Siviero Agazzi and colleagues of University of South Florida, Tampa. The researchers write, “PSR, despite being the most cost-effective, is by far the least utilized treatment modality.”
Surgical Options for Trigeminal Neuralgia
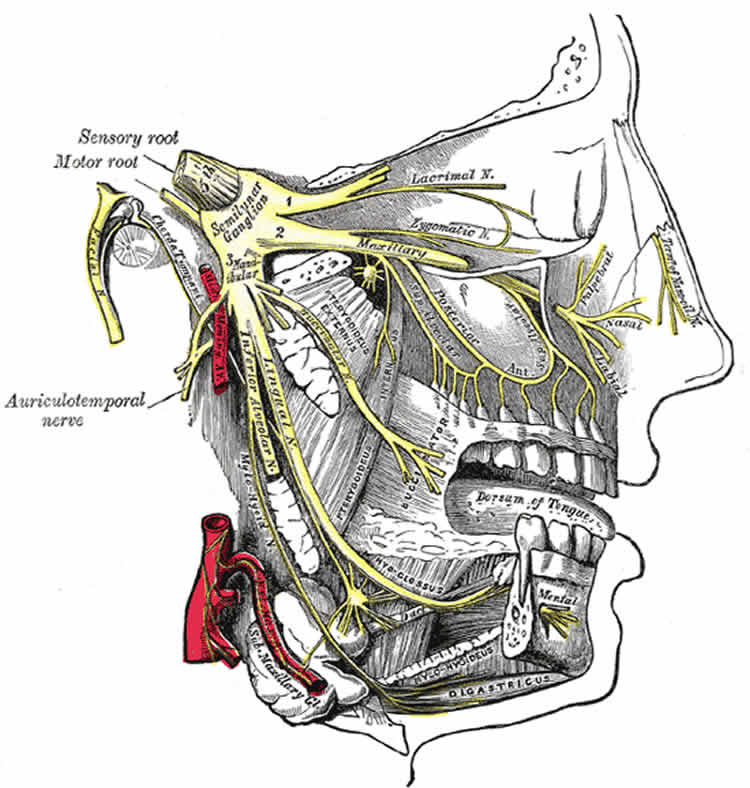
Trigeminal neuralgia is a relatively common chronic pain condition, especially among older adults. Sometimes called “tic douloureux,” trigeminal neuralgia is associated with a typical pattern of painful facial tics. Pain is thought to be caused by blood vessels placing pressure on the trigeminal nerve in the face.
When pain from trigeminal neuralgia can’t be adequately controlled by medications, various surgical procedures may be recommended. To compare the cost-effectiveness of different surgical options, the researchers analyzed data on Medicare claims for trigeminal neuralgia during 2011. Of 1,582 patients with trigeminal neuralgia, 94 patients—six percent of the total—underwent surgical treatment.
Fifty-one percent of surgically treated patients underwent a procedure called microvascular decompression (MVD), in which a pad is placed to relieve pressure on the nerve. Forty-two percent underwent stereotactic radiosurgery (SRS), a less-invasive “gamma knife” procedure. The remaining seven percent of patients underwent PSR—a percutaneous operation in which the nerve fibers causing pain are destroyed by a needle inserted from the cheek all the way into the skull.
But although PSR was the least commonly used procedures, it was the least expensive, with an average weighted cost of about $3,900. That was about one-tenth the cost of the other two options: about $40,000 for MVD and $38,000 for SRS.
Show Wide Variations in Cost-Effectiveness
Based on published data, all three procedures reduced pain from trigeminal neuralgia, with some differences in effectiveness. Over ten years, average “quality-adjusted life-years” (QALYs)—reflecting one year free of pain and without pain medications—were 8.2 for MVD, 4.9 for SRS, and 6.5 for PSR.
After accounting for these differences, PSR was by far the most cost-effective option. Cost per QALY gained was about $600 with PSR, compared to $4,900 for MVD and $7,800 for SRS. Percutaneous stereotaxic rhizotomy was eight times more cost-effective than MVD and 13 times more cost-effective than SRS.
Dr. Agazzi and coauthors emphasize that their Medicare claims study is only preliminary. It was based on small numbers of patients—including just seven treated with PSR. It also included limited data on outcomes and complications, such as facial numbness.
But within those limitations, the results suggest that PSR is an “under-utilized” procedure for patients with painful facial tics. The PSR procedure provides comparable pain relief, at a fraction of the cost of more commonly performed procedures. While further research is needed, Dr. Agazzi and colleagues note their findings are consistent with the only two previous studies evaluating the cost-effectiveness of surgical options for trigeminal neuralgia.
This article was submitted directly to NeuroscienceNews.com by Ellen Robinson at Wolters Kluwer Health. We would like to thank Ellen Robinson for this submission.
Contact: Connie Hughes – Wolters Kluwer Health
Source: Wolters Kluwer Health press release
Image Source: The image is credited to Gray’s Anatomy and is in the public domain.
Original Research: Full open access research for “Surgical Management of Trigeminal Neuralgia: Use and Cost-Effectiveness From an Analysis of the Medicare Claims Database” by Sivakanthan, Sananthan BS; Van Gompel, Jamie J. MD; Alikhani, Puya MD; van Loveren, Harry MD; Chen, Ren PhD, MPH; and Agazzi, Siviero MD, MBA in Neurosurgery. Published online August 2014 doi:10.1227/NEU.0000000000000430






