Patients with traumatic brain injuries are not benefiting from recent advances in cognitive neuroscience research – and they should be, scientists report in a special issue of Current Opinion in Behavioral Sciences.
Those who treat brain-injured patients rarely make use of new scientific discoveries about the workings of the brain. Instead, doctors, nurses and emergency personnel rely on a decades-old tool, the Glasgow coma scale, to categorize brain injuries as mild, moderate or severe. Brain scans are sometimes performed to help identify damaged regions, and then most patients receive one or more of the following four diagnoses: coma (no response to sensory stimulation), delirium (impaired ability to sustain attention), amnesia (impaired memory) and dysexecutive syndrome (impaired ability to engage in goal-directed thought).
These crude classifications reveal little about the underlying brain mechanisms that are damaged as a result of brain trauma, said Aron Barbey, a University of Illinois professor of neuroscience, of psychology, and of speech and hearing science. He and his colleagues propose that doctors take a deeper look at the brain networks that enable the regulation and control of attention, memory and thought – termed “cognitive control processes” – and use this knowledge to develop more targeted treatment strategies. Barbey is a professor in the Beckman Institute for Advanced Science and Technology and in the Carl R. Woese Institute for Genomic Biology at the U. of I.
“Traumatic brain injury is a global public health epidemic with an incidence that continues to rise,” Barbey said. “By 2020, the World Health Organization projects TBI will be the world’s leading cause of neurological disability across all age groups.
“An emerging area of research seeks to develop better ways to assess traumatic brain injury. Recent findings demonstrate that multiple, interdependent brain networks drive and organize cognition. It is these networks that are highly susceptible to brain injury,” he said.
Cognitive neuroscientists have identified dozens of brain networks, each of which engages a specific set of brain structures to perform particular tasks. Each node in a network communicates with the others via axons, the nerve fibers that bundle together to form white-matter tracts.
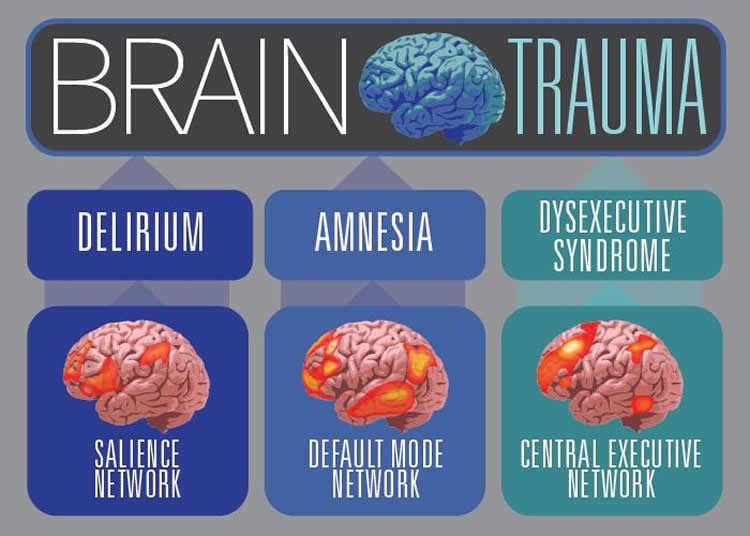
“There are three core networks that support cognitive control processes that often are impaired in traumatic brain injury,” Barbey said. “The ‘salience network’ directs attention to significant events in our environment and is known to enable coordinated behavior. The ‘default mode network’ supports an internal focus of attention, enabling autobiographical memory and the ability to envision future events. Finally, the ‘central executive network’ directs attention to the external environment and supports goal-directed thought, such as planning and problem solving.”
Disruption of the salience network corresponds to symptoms seen in those diagnosed with delirium, Barbey said. A diagnosis of amnesia corresponds to disruption of the default mode network, and dysexecutive syndrome is associated with damage to the central executive network, he said.
A coma diagnosis reflects systemwide failure, Barbey said.
Understanding which brain networks are damaged in brain-injured patients will help doctors better predict the kinds of impairments their patients will experience, and will guide clinical treatment and therapy.
To that end, the researchers recommend therapies that have shown promise in strengthening specific cognitive control functions.
Many methods that are familiar to cognitive neuroscience but little-used in patient therapy should be tested in patient populations, the researchers wrote. These include interventions that target specific brain networks, such as transcranial direct-current brain stimulation, and approaches that deliver global benefits to brain health, such as physical fitness training.
Research indicates that brain stimulation can be applied to specific brain networks to enhance their ability to respond optimally to cognitive rehabilitation, Barbey said. Physical fitness is known to promote brain health and therefore may enhance resilience to brain injury, he said.
“The goal is to develop more precise assessment standards for traumatic brain injury and to translate discoveries from cognitive neuroscience into effective clinical therapies that promote recovery from brain injury,” he said.
Source: Diana Yates – University of Illinois
Image Source: Image credited to Julie McMahon
Original Research: Abstract for “Network topology and dynamics in traumatic brain injury” by Aron K Barbey, Antonio Belli, Ann Logan, Rachael Rubin, Marta Zamroziewicz, and Joachim T Operskalski in Current Opinion in Behavioral Sciences. Published online April 24 2015 doi:10.1016/j.cobeha.2015.04.002
Abstract
Network topology and dynamics in traumatic brain injury
We propose a network approach to clinical translation that defines core behavioral phenotypes of traumatic brain injury (TBI) with respect to damage to specific intrinsic connectivity networks (ICNs). We survey recent approaches to clinical translation from cognitive neuroscience that enhance network function and recovery from brain injury through interventions that deliver targeted (network specific) and global (systemic) effects. A network approach provides insight into the mechanisms of brain injury, linking ICN characteristics to specific profiles of cognitive impairment, providing key neurobiological targets for therapeutic intervention, and motivating new perspectives about the nature of cognitive recovery and rehabilitation in TBI.
“Network topology and dynamics in traumatic brain injury” by Aron K Barbey, Antonio Belli, Ann Logan, Rachael Rubin, Marta Zamroziewicz, and Joachim T Operskalski in Current Opinion in Behavioral Sciences. Published online April 24 2015 doi:10.1016/j.cobeha.2015.04.002