Summary: A new mathematical model can accurately reproduce experimental results on pain sensitivity and predict how the results are affected by the time of day.
Source: PLOS
A new computational model successfully predicts how daily pain sensitivity rhythms affect pain processing, both in healthy adults and in people with neuropathic pain. Jennifer Crodelle of New York University and colleagues present these findings in PLOS Computational Biology.
Just as processes like metabolism and alertness exhibit a daily rhythm, pain sensitivity changes over the course of the day. Sensitivity is usually highest in the middle of the night and lowest in the late afternoon. However, this rhythm is flipped for people with neuropathic pain, who feel severe pain in response to a typically non-painful stimulus. For these patients, the lowest pain sensitivity occurs at night.
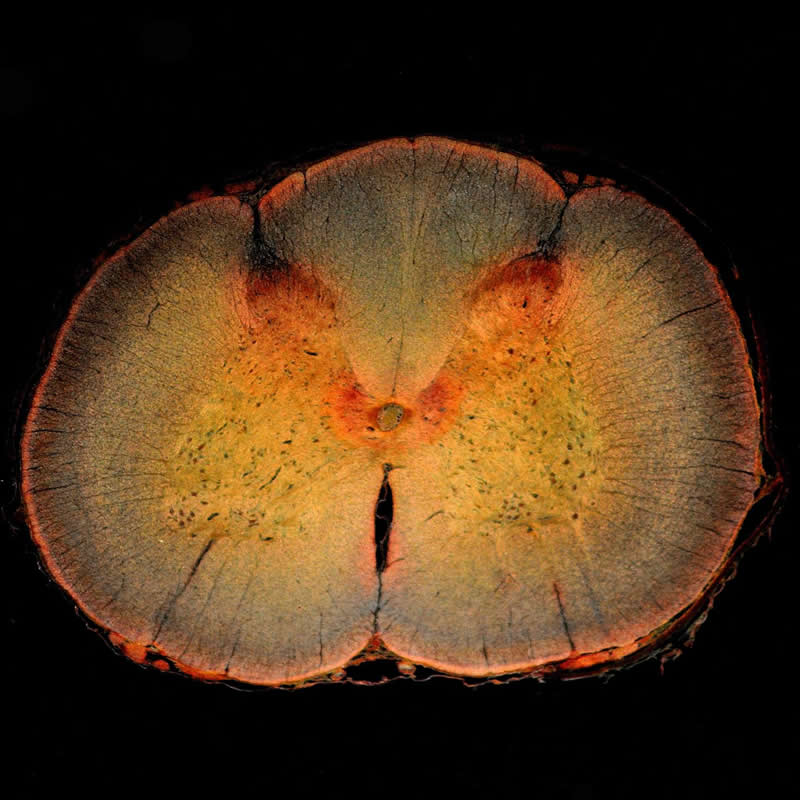
The mechanisms underlying both normal and neuropathic pain rhythms have been unclear. To gain new insights, Crodelle and colleagues built a mathematical model that simulates how pain is transmitted from a nerve to the spinal cord’s dorsal horn, where the pain is initially processed.
The researchers found that their model successfully reproduces experimental results on pain sensitivity and predicts how these results are affected by the time of day. For instance, it predicts the time-of-day effects on pain inhibition, the phenomenon in which one feels a lessening of pain from applying light pressure, such as by grabbing a stubbed toe.
The model also suggests a potential mechanism for the flipped sensitivity rhythm in people with neuropathic pain: a change from inhibition to excitation in the synaptic connections between nerve cells. This finding points to targets for further experimental study and potential treatment.
“Our modeling results provide a first step in understanding how the daily rhythm in pain sensitivity affects normal pain processing across the day and potentially how the daily rhythm can benefit pain management strategies in clinical settings,” Crodelle says.
“For example, pain relief medication could be titrated appropriately across the day, thus reducing the total amount of medication needed.”
Potential next steps are to incorporate factors that may influence the daily pain sensitivity rhythm, such as sleep deprivation and jet lag. The model could also aid investigations into how pain sensitivity is reduced by a chronic pain treatment known as spinal cord stimulation.
Funding: The authors were funded by the National Institute for Mathematical and Biological Synthesis, sponsored by the National Science Foundation through NSF Award DBI-1300426, with additional support from The University of Tennessee, Knoxville (JC, SHP, MHH, VB) http://www.nimbios.org. This work was also partially supported by the following sources: NSF Mathematical Sciences PostDoctoral Research Fellowship DMS-1703761 (JC), University of Michigan (SHP), NSF Award DMS-1412119 (VB), and the Pritzker Neuropsychiatric Disorders Research Consortium (MHH). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Source:
PLOS
Media Contacts:
Jennifer Crodelle – PLOS
Image Source:
The image is credited to dw_ross/Flickr.
Original Research: Open access
“Modeling the daily rhythm of human pain processing in the dorsal horn”. Jennifer Crodelle, Sofia H. Piltz, Megan Hastings Hagenauer, Victoria Booth.
PLOS Computational Biology. doi:10.1371/journal.pcbi.1007106
Abstract
Modeling the daily rhythm of human pain processing in the dorsal horn
Experimental studies show that human pain sensitivity varies across the 24-hour day, with the lowest sensitivity usually occurring during the afternoon. Patients suffering from neuropathic pain, or nerve damage, experience an inversion in the daily modulation of pain sensitivity, with the highest sensitivity usually occurring during the early afternoon. Processing of painful stimulation occurs in the dorsal horn (DH), an area of the spinal cord that receives input from peripheral tissues via several types of primary afferent nerve fibers. The DH circuit is composed of different populations of neurons, including excitatory and inhibitory interneurons, and projection neurons, which constitute the majority of the output from the DH to the brain. In this work, we develop a mathematical model of the dorsal horn neural circuit to investigate mechanisms for the daily modulation of pain sensitivity. The model describes average firing rates of excitatory and inhibitory interneuron populations and projection neurons, whose activity is directly correlated with experienced pain. Response in afferent fibers to peripheral stimulation is simulated by a Poisson process generating nerve fiber spike trains at variable firing rates. Model parameters for fiber response to stimulation and the excitability properties of neuronal populations are constrained by experimental results found in the literature, leading to qualitative agreement between modeled responses to pain and experimental observations. We validate our model by reproducing the wind-up of pain response to repeated stimulation. We apply the model to investigate daily modulatory effects on pain inhibition, in which response to painful stimuli is reduced by subsequent non-painful stimuli. Finally, we use the model to propose a mechanism for the observed inversion of the daily rhythmicity of pain sensation under neuropathic pain conditions. Underlying mechanisms for the shift in rhythmicity have not been identified experimentally, but our model results predict that experimentally-observed dysregulation of inhibition within the DH neural circuit may be responsible. The model provides an accessible, biophysical framework that will be valuable for experimental and clinical investigations of diverse physiological processes modulating pain processing in humans.