Summary: According to researchers, people with diabetes may be at increased risk of suffering from depression as a result of biological problems in regulating sugar levels that influence emotional response in the brain. Using EEG, researchers discovered those with higher levels of insulin resistance showed greater response to negative images.
Source: Iowa State University.
For millions of Americans who are obese and living with diabetes or prediabetes, feelings of sadness, anger and anxiety are often part of daily life.
A new Iowa State University study suggests those negative feelings may stem from problems regulating blood sugar levels that influence emotional response in the brain. The study found people with Type 2 diabetes and prediabetes were more likely to focus on and have a strong emotional response to threats and negative things, which affects quality of life and increases risk for depression. The research is published in the journal Psychosomatic Medicine.
Auriel Willette, an ISU assistant professor of food science and human nutrition; Tovah Wolf, lead author and a graduate student working with Willette on this project; and colleagues at the University of Wisconsin-Madison analyzed data on startle response, brain activity, cortisol levels and cognitive assessment. Data for the study came from Midlife in the U.S. (MIDUS), a national study of health and well-being.
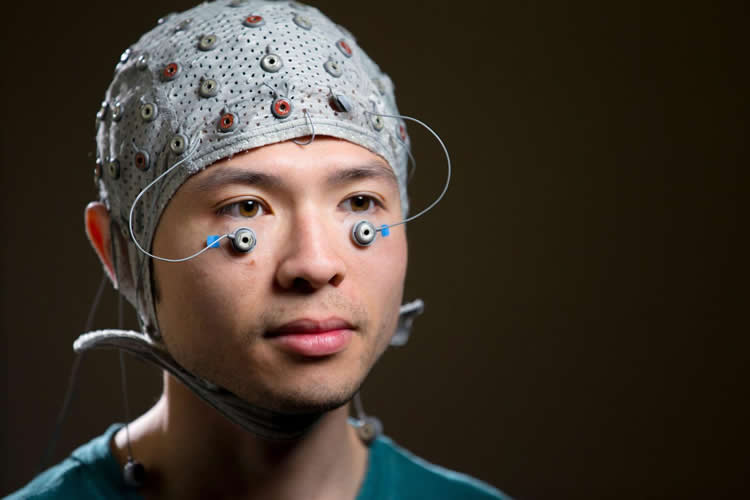
Willette says gauging the startle response allowed researchers to measure central nervous system activity using tiny electrodes placed below the eye. Study participants viewed a series of negative, positive and neutral images intended to elicit an emotional response. The electrodes captured the rate of flinch or startle, a contraction we cannot control, associated with each image, he said.
“People with higher levels of insulin resistance were more startled by negative pictures. By extension, they may be more reactive to negative things in life,” Willette said. “It is one piece of evidence to suggest that these metabolic problems are related to issues with how we perceive and deal with things that stress all of us out.”
The researchers say the evidence is even more compelling when combined with the results of EEG tests recording activity when the brain is at rest. Study participants with prediabetes and Type 2 diabetes had more activity on the right side of the brain, which is associated with depression and negative emotions. If someone is predisposed to focusing on negative things, it may become a barrier for losing weight and reversing health issues, Wolf said.
People with prediabetes and diabetes also recorded lower cortisol levels – a potential indicator of chronic stress – and cognitive test scores, providing additional support for the findings.
Personal motivation
Understanding the effect of these biological factors is an important step in helping improve the quality of life for the one-third of Americans who are obese. Wolf, a registered dietitian, says her experience working with patients suffering from chronic diseases led her to this line of research. She often noticed differences in how patients responded to stress and wondered if that influenced their motivation to live a healthy life.
“For people with blood sugar problems, being more stressed and reactive can cause blood sugar to spike. If people with prediabetes and diabetes are trying to reverse or treat the disease, stressful events may hinder their goals,” Wolf said. “Frequent negative reactions to stressful events can lead to a lower quality of life and create a vicious cycle that makes it difficult to be healthy.”
Willette can relate. He struggled with weight, at one time weighing 260 pounds, which affected his day-to-day quality of life. Willette says the risk of cardiovascular disease and other chronic illnesses related to obesity is well known, but many people may not recognize how fluctuations in blood sugar can take a toll on them every day.
Funding: The researchers say additional work is needed to determine if the link between insulin resistance and emotional response is causal, and explore options for potential interventions. Vera Tsenkova, Carol D. Ryff and Richard Davidson, all with the University of Wisconsin-Madison, contributed to the research.
Source: Auriel Willette – Iowa State University
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Christopher Gannon, Iowa State University.
Original Research: Abstract for “Neural, Hormonal, and Cognitive Correlates of Metabolic Dysfunction and Emotional Reactivity” by Tovah Wolf; Vera Tsenkova; Carol D. Ryff; Richard J. Davidson; and Auriel A. Willette in Psychosomatic Medicine: Journal of Biobehavioral Medicine. Published March 28 2018.
doi:10.1097/PSY.0000000000000582
[cbtabs][cbtab title=”MLA”]Iowa State University “Brain Activity May Explain Diabetics’ Negative Feelings and Increased Depression Risk.” NeuroscienceNews. NeuroscienceNews, 7 May 2018.
<https://neurosciencenews.com/diabetes-depression-eeg-8982/>.[/cbtab][cbtab title=”APA”]Iowa State University (2018, May 7). Brain Activity May Explain Diabetics’ Negative Feelings and Increased Depression Risk. NeuroscienceNews. Retrieved May 7, 2018 from https://neurosciencenews.com/diabetes-depression-eeg-8982/[/cbtab][cbtab title=”Chicago”]Iowa State University “Brain Activity May Explain Diabetics’ Negative Feelings and Increased Depression Risk.” https://neurosciencenews.com/diabetes-depression-eeg-8982/ (accessed May 7, 2018).[/cbtab][/cbtabs]
Abstract
Neural, Hormonal, and Cognitive Correlates of Metabolic Dysfunction and Emotional Reactivity
Objective
Pre-diabetes and type 2 diabetes (i.e., hyperglycemia) are characterized by insulin resistance (IR). These problems with energy metabolism may exacerbate emotional reactivity to negatively valenced stimuli and related phenomena like predisposition toward negative affect, as well as cognitive deficits. Higher emotional reactivity is seen with hyperglycemia and IR. Yet, it is largely unknown how metabolic dysfunction correlates with related neural, hormonal, and cognitive outcomes.
Methods
Among 331 adults from the Midlife in the United States (MIDUS), we cross-sectionally examined eye- blink response (EBR) to gauge reactivity to negative, positive, or neutrally-valenced pictures from international affect picture system (IAPS) stimuli proximal to an acoustic startle probe. Increased EBR to negative stimuli was considered an index of stress reactivity. Frontal alpha asymmetry, a biomarker of negative affect predisposition, was determined using resting electroencephalography (EEG).
Methods
Baseline urinary cortisol output was collected. Cognitive performance was gauged using the Brief Test of Adult Cognition by telephone (BTACT). Fasting glucose and insulin characterized hyperglycemia or the homeostatic model assessment of IR (HOMA-IR).
Results
Higher HOMA-IR corresponded to an increased startle response, measured by EBR magnitude, for negative versus positive stimuli [R2=0.218, F(1,457)=5.48, p=.020, euglycemia: Mean±SD=.092±.776, hyperglycemia: Mean±SD=.120±.881]. Participants with hyperglycemia vs. euglycemia showed greater right frontal alpha asymmetry [F(1,307)=6.62, p=.011, euglycemia: Mean±SD=.018±.167, hyperglycemia: Mean±SD=-.029±.160] and worse BTACT arithmetic performance [F(1,284)=4.25, p=.040, euglycemia: Mean±SD=2.390±1.526), hyperglycemia: Mean±SD=1.920±1.462]. Baseline urinary cortisol (log10 μg/12 hr) was also dysregulated in individuals with hyperglycemia [[F(1,324)=5.09, p=.025, euglycemia: Mean±SD=1.052±.332, hyperglycemia: Mean±SD=.961±.362].
Conclusion
These results suggest that dysmetabolism is associated with increased emotional reactivity, predisposition toward negative affect, and specific cognitive deficits.







