Summary: A new automated method can identify and track the development of tau deposits in the brain. The method could lead to an earlier diagnosis of Alzheimer’s disease.
Source: Mass General
Amyloid-beta and tau are the two key abnormal protein deposits that accumulate in the brain during the development of Alzheimer’s disease, and detecting their buildup at an early stage may allow clinicians to intervene before the condition has a chance to take hold.
A team led by investigators at Massachusetts General Hospital (MGH) has now developed an automated method that can identify and track the development of harmful tau deposits in a patient’s brain. The research, which is published in Science Translational Medicine, could lead to earlier diagnoses of Alzheimer’s disease.
“While our understanding of Alzheimer’s disease has increased greatly in recent years, many attempts to treat the condition so far have failed, possibly because medical interventions have taken place after the stage at which the brain injury becomes irreversible,” says lead author Justin Sanchez, a data analyst at MGH’s Gordon Center for Medical Imaging.
In an attempt to develop a method for earlier diagnosis, Sanchez and his colleagues, under the leadership of Keith A. Johnson, MD, of the departments of Radiology and Neurology at MGH, evaluated brain images of amyloid-beta and tau obtained by positron emission tomography, or PET, in 443 adults participating in several observational studies of aging and Alzheimer’s disease. Participants spanned a wide range of ages, with varying degrees of amyloid-beta and cognitive impairment — from healthy 20-year-olds to older patients with a clinical diagnosis of Alzheimer’s dementia. The researchers used an automated method to identify the brain region most vulnerable to initial cortical tau buildup in each individual PET scan.
“We hypothesized that applying our method to PET images would enable us to detect the initial accumulation of cortical tau in cognitively normal people, and to track the spread of tau from this original location to other brain regions in association with amyloid-beta deposition and the cognitive impairment of Alzheimer’s disease,” explains Sanchez. He notes that cortical tau, when it spreads from its site of origin to neocortical brain regions under the influence of amyloid-beta, appears to be the “bullet” that injures brains in Alzheimer’s disease.
The technique revealed that tau deposits first emerge in the rhinal cortex region of the brain, independently from amyloid-beta deposits, before spreading to the nearby temporal neocortex. “We observed initial cortical tau accumulation at this site of origin in cognitively normal individuals without evidence of elevated amyloid-beta, as early as 58 years old,” says Sanchez.
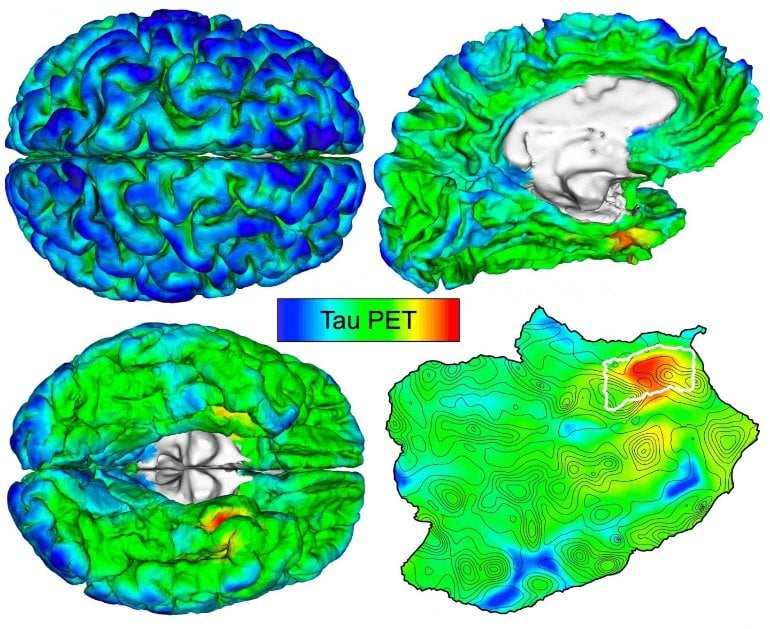
Importantly, when the scientists followed 104 participants for two years, they found that people with the highest initial levels of tau at the point of origin exhibited the most spread of tau throughout the brain over time.
The findings suggest that PET measurements of tau focused on precisely individualized specific brain regions may predict an individual’s risk of future tau accumulation and consequent Alzheimer’s disease. Targeting tau when detected at an early stage might prevent the condition or slow its progression.
“Clinical trials evaluating the efficacy of anti-tau therapeutics would benefit from an automated, individualized imaging method to select cognitively normal individuals vulnerable to impending tau spread, thus advancing our efforts to provide effective interventions for patients at risk for Alzheimer’s disease,” says Sanchez.
Funding: This work was supported by the National Institutes of Health.
About this Alzheimer’s disease research news
Source: Mass General
Contact: Michael Morrison – Mass General
Image: The image is credited to Justin Sanchez
Original Research: Closed access.
“The cortical origin and initial spread of medial temporal tauopathy in Alzheimer’s disease assessed with positron emission tomography” by Justin Sanchez et al. Science Translational Medicine
Abstract
The cortical origin and initial spread of medial temporal tauopathy in Alzheimer’s disease assessed with positron emission tomography
Advances in molecular positron emission tomography (PET) have enabled anatomic tracking of brain pathology in longitudinal studies of normal aging and dementia, including assessment of the central model of Alzheimer’s disease (AD) pathogenesis, according to which TAU pathology begins focally but expands catastrophically under the influence of amyloid-β (Aβ) pathology to mediate neurodegeneration and cognitive decline. Initial TAU deposition occurs many years before Aβ in a specific area of the medial temporal lobe. Building on recent work that enabled focus of molecular PET measurements on specific TAU-vulnerable convolutional temporal lobe anatomy, we applied an automated anatomic sampling method to quantify TAU PET signal in 443 adult participants from several observational studies of aging and AD, spanning a wide range of ages, Aβ burdens, and degrees of clinical impairment. We detected initial cortical emergence of tauopathy near the rhinal sulcus in clinically normal people and, in a subset with longitudinal 2-year follow-up data (n = 104), tracked Aβ-associated spread of TAU from this site first to nearby neocortex of the temporal lobe and then to extratemporal regions. Greater rate of TAU spread was associated with baseline measures of both global Aβ burden and medial temporal lobe TAU. These findings are consistent with clinicopathological correlation studies of Alzheimer’s tauopathy and enable precise tracking of AD-related TAU progression for natural history studies and prevention therapeutic trials.