Summary: Pain signaling occurs much faster than previously believed. Researchers report thickly myelinated nerves contribute to pain processing speeds.
Source: Linkoping University
Pain signals can travel as fast as touch signals, according to a new study from researchers at Linköping University in Sweden, Liverpool John Moores University in the UK, and the National Institutes of Health (NIH) in the US. The discovery of a rapid pain-signalling system challenges our current understanding of pain. The study is published in the scientific journal Science Advances.
It has until now been believed that nerve signals for pain are always conducted more slowly than those for touch. The latter signals, which allow us to determine where we are being touched, are conducted by nerves that have a fatty sheath of myelin that insulates the nerve. Nerves with a thick layer of myelin conduct signals more rapidly than unmyelinated nerves. In contrast, the signalling of pain in humans has been thought to be considerably slower and carried out by nerves that have only a thin layer of myelin, or none at all.
In monkeys and many other mammals, on the other hand, part of the pain-signalling system can conduct nerve signals just as fast as the system that signals touch. The scientists speculated whether such a system is also present in humans.
“The ability to feel pain is vital to our survival, so why should our pain-signalling system be so much slower than the system used for touch, and so much slower than it could be?” asks Saad Nagi, principal research engineer of the Department of Clinical and Experimental Medicine and the Center for Social and Affective Neuroscience (CSAN) at Linköping University.
To answer this, the scientists used a technique that allowed them to detect the signals in the nerve fibres from a single nerve cell. They examined 100 healthy volunteers and looked for nerve cells that conducted signals as rapidly as the nerve cells that detect touch, but that had the properties of pain receptors, otherwise known as nociceptors. Pain receptors are characterised by the ability to detect noxious stimuli, such as pinching and abrasion of the skin, while not reacting to light touch. The researchers found that 12% of thickly myelinated nerve cells had the same properties as pain receptors, and in these nerve cells the conduction speed was as high as in touch-sensitive nerve cells.
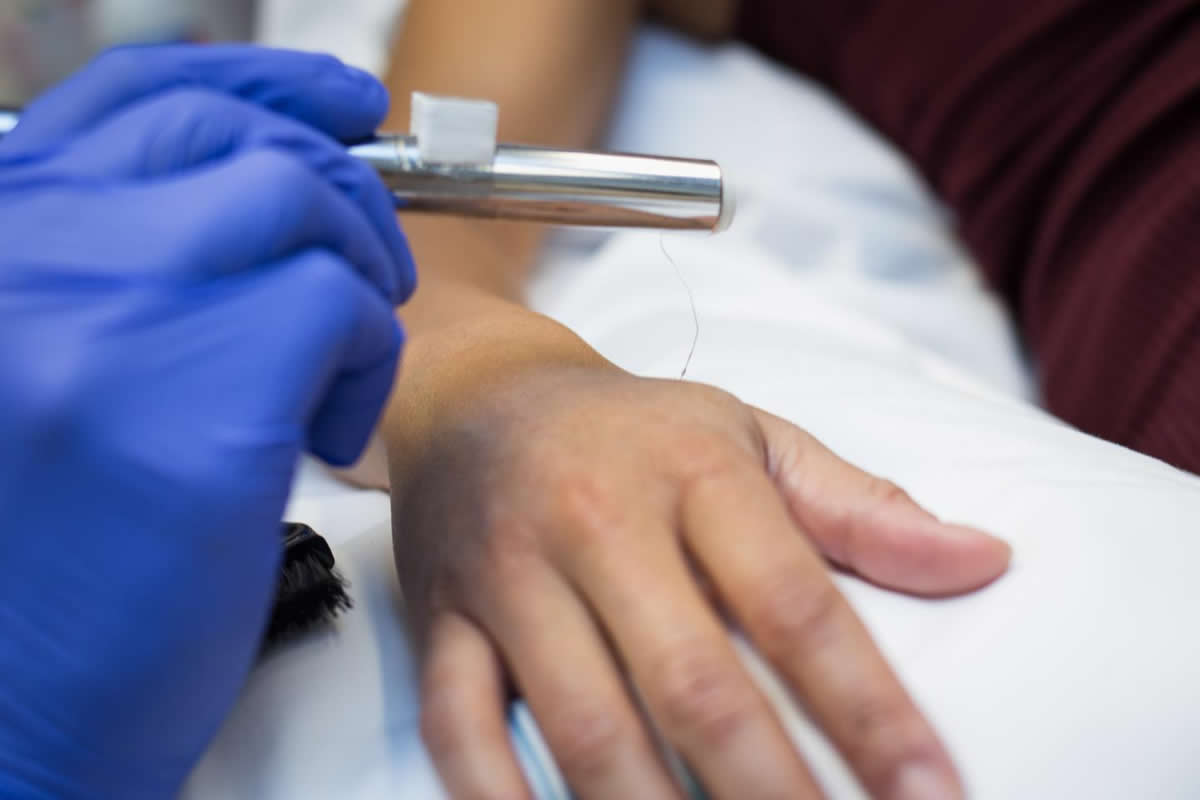
The next step of the scientists’ research was to determine the function of these ultrafast pain receptors. By applying short electrical pulses through the measurement electrodes, they could stimulate individual nerve cells. The volunteers described that they experienced sharp or pinprick pain.
“When we activated an individual nerve cell, it caused a perception of pain, so we conclude that these nerve cells are connected to pain centres in the brain”, says Saad Nagi.
The research team also investigated patients with various rare neurological conditions. One group of people had, as adults, acquired nerve damage that led to the thickly myelinated nerve fibres being destroyed, while the small fibres were spared. These patients cannot detect light touch. The scientists predicted that the loss of myelinated nerve fibres should also affect the rapidly conducting pain system they had identified. It turned out that these people had an impaired ability to experience mechanical pain. Examination of patients with two other rare neurological conditions gave similar results. These results may be highly significant for pain research, and for the diagnosis and care of patients with pain.
“It’s becoming evident that thickly myelinated nerve fibres contribute to the experience of pain when it has a mechanical cause. Our results challenge the textbook description of a rapid system for signalling touch and a slower system for signalling pain. We suggest that pain can be signalled just as rapidly as touch”, says Saad Nagi.
Funding: The study is an international research collaboration funded by, among others, the Swedish Research Council, ALF Region Östergötland, the Pain Relief Foundation and the Intramural Research Program of the NIH (NCCIH).
Source:
Linkoping University
Media Contacts:
Saad Nagi – Linkoping University
Image Source:
The image is credited to Charlotte Perhammar/LiU.
Original Research: Open access
“An ultra-fast system for signaling mechanical pain in human skin”. Saad S. Nagi, Andrew G. Marshall, Adarsh Makdani, Ewa Jarocka, Jaquette Liljencrantz, Mikael Ridderström, Sumaiya Shaikh, Francis O´Neill, Dimah Saade, Sandra Donkervoort, A. Reghan Foley, January Minde, Mats Trulsson, Jonathan Cole, Carsten G. Bönnemann, Alexander T. Chesler, M. Catherine Bushnell, Francis McGlone, and Håkan Olausson.
Nature. doi:10.1126/sciadv.aaw1297
Abstract
An ultra-fast system for signaling mechanical pain in human skin
The canonical view is that touch is signaled by fast-conducting, thickly myelinated afferents, whereas pain is signaled by slow-conducting, thinly myelinated (“fast” pain) or unmyelinated (“slow” pain) afferents. While other mammals have thickly myelinated afferents signaling pain (ultrafast nociceptors), these have not been demonstrated in humans. Here, we performed single-unit axonal recordings (microneurography) from cutaneous mechanoreceptive afferents in healthy participants. We identified A-fiber high-threshold mechanoreceptors (A-HTMRs) that were insensitive to gentle touch, encoded noxious skin indentations, and displayed conduction velocities similar to A-fiber low-threshold mechanoreceptors. Intraneural electrical stimulation of single ultrafast A-HTMRs evoked painful percepts. Testing in patients with selective deafferentation revealed impaired pain judgments to graded mechanical stimuli only when thickly myelinated fibers were absent. This function was preserved in patients with a loss-of-function mutation in mechanotransduction channel PIEZO2. These findings demonstrate that human mechanical pain does not require PIEZO2 and can be signaled by fast-conducting, thickly myelinated afferents.







