Smokers who are able to quit might actually be hard-wired for success, according to a study from Duke Medicine.
The study, published in Neuropsychopharmacology, showed greater connectivity among certain brain regions in people who successfully quit smoking compared to those who tried and failed.
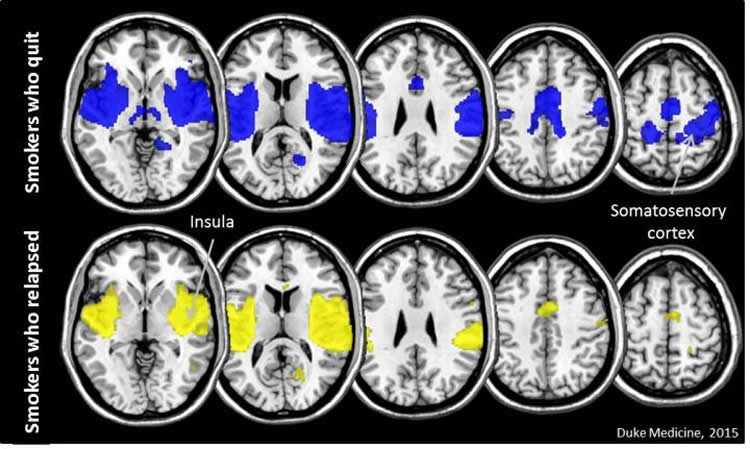
The researchers analyzed MRI scans of 85 people taken one month before they attempted to quit. All participants stopped smoking and the researchers tracked their progress for 10 weeks. Forty-one participants relapsed. Looking back at the brain scans of the 44 smokers who quit successfully, the researchers found they had something in common before they stopped smoking — better synchrony (coordinated activity) between the insula, home to urges and cravings, and the somatosensory cortex, a part of the brain that is central to our sense of touch and motor control.
“Simply put, the insula is sending messages to other parts of the brain that then make the decision to pick up a cigarette or not,” said Merideth Addicott, Ph.D., assistant professor at Duke and lead author of the study.
The insula, a large region in the cerebral cortex, has been the subject of many smoking cessation studies that show this area of the brain is active when smokers are craving cigarettes, said Joseph McClernon, Ph.D., associate professor at Duke and the study’s senior author. Other studies have found that smokers who suffer damage to the insula appear to spontaneously lose interest in smoking.
“There’s a general agreement in the field that the insula is a key structure with respect to smoking and that we need to develop cessation interventions that specifically modulate insula function,” McClernon said. “But in what ways do we modulate it, and in whom? Our data provides some evidence on both of those fronts, and suggests that targeting connectivity between insula and somatosensory cortex could be a good strategy.”
Neurofeedback and transcranial magnetic stimulation, used to improve depression, are two treatments that modulate brain activity. With the findings in this study, researchers now have more information on where to further investigate, McClernon said.
“We have provided a blueprint,” McClernon said. “If we can increase connectivity in smokers to look more like those who quit successfully, that would be a place to start. We also need more research to understand what it is exactly about greater connectivity between these regions that increases the odds of success.”
In addition to Addicott and McClernon, study authors include Maggie Sweitzer; Brett Froeliger; and Jed Rose.
Funding: The researchers received funding from the National Institute on Drug Abuse (R01 DA025876; K01 DA033347). McClernon is also a site principal investigator on an investigator-initiated grant (GRAND) from Pfizer, Inc.
Source: Samiha Khanna – Duke Medicine
Image Source: Image courtesy of Duke Medicine
Original Research: Abstract for “Increased Functional Connectivity in an Insula-Based Network is Associated with Improved Smoking Cessation Outcomes” by Merideth A Addicott, Maggie M Sweitzer, Brett Froeliger, Jed E Rose & Francis J McClernon in Neuropsychopharmacology. Published online April 21 2015 doi:10.1038/npp.2015.114
Abstract
Increased Functional Connectivity in an Insula-Based Network is Associated with Improved Smoking Cessation Outcomes
Little is known regarding the underlying neurobiology of smoking cessation. Neuroimaging studies indicate a role for the insula in connecting the interoceptive awareness of tobacco craving with a larger brain network that motivates smoking. We investigated differences in insula-based functional connectivity between smokers who did not relapse during a quit attempt vs those who relapsed. Smokers (n=85) underwent a resting-state functional connectivity scan and were then randomized into two groups (either smoking usual brand cigarettes or smoking very low nicotine cigarettes plus nicotine replacement therapy) for 30 days before their target quit date. Following the quit date, all participants received nicotine replacement therapy and their smoking behavior was observed for 10 weeks. Participants were subsequently classified as nonrelapsed (n=44) or relapsed (i.e., seven consecutive days of smoking greater than or equal to1 cigarette/day; n=41). The right and left insula, as well as insula subdivisions (posterior, ventroanterior, and dorsoanterior) were used as seed regions of interest in the connectivity analysis. Using the right and left whole-insula seed regions, the nonrelapsed group had greater functional connectivity than the relapsed group with the bilateral pre- and postcentral gyri. This effect was isolated to the right and left posterior insula seed regions. Our results suggest that relapse vulnerability is associated with weaker connectivity between the posterior insula and primary sensorimotor cortices. Perhaps greater connectivity in this network improves the ability to inhibit a motor response to cigarette cravings when those cravings conflict with a goal to remain abstinent. These results are consistent with recent studies demonstrating a positive relationship between insula-related functional connectivity and cessation likelihood among neurologically intact smokers.
“Increased Functional Connectivity in an Insula-Based Network is Associated with Improved Smoking Cessation Outcomes” by Merideth A Addicott, Maggie M Sweitzer, Brett Froeliger, Jed E Rose & Francis J McClernon in Neuropsychopharmacology. Published online April 21 2015 doi:10.1038/npp.2015.114