Summary: Propranolol, a beta-blocker commonly used to treat haemangioma in children and cardiovascular disease, can also be used to treat cerebral cavernous malformations, a condition characterized by misshapen neural blood vessels.
Source: Uppsala University
Propranolol, a drug that is efficacious against infantile haemangiomas (“strawberry naevi”, resembling birthmarks), can also be used to treat cerebral cavernous malformations, a condition characterised by misshapen blood vessels in the brain and elsewhere. This has been shown by researchers at Uppsala University in a new study published in the scientific journal Stroke.
“Up to now, there’s been no drug treatment for these patients, so our results may become hugely important for them,” says Peetra Magnusson of the University’s Department of Immunology, Genetics and Pathology, who headed the study.
Cerebral cavernous malformations (CCMs, also called cavernous angiomas or cavernomas) are vascular lesions on blood vessels in the brain and elsewhere, caused by genetic changes that may be hereditary or arise spontaneously. Today, an operation to remove these lesions is the only possible treatment. However, surgical interventions in the brain are highly risky. Since the vascular malformations, moreover, recur in the hereditary form of the condition, a drug treatment for CCMs is urgently required instead.
The uses of propranolol, a beta blocker, include treating cardiovascular diseases and conditions, such as high blood pressure. But it can also be used to treat a haemangioma (“strawberry naevus”), a common blood-vessel malformation in children. There are some indications that the preparation might work against CCMs as well.
The new study is a collaboration involving researchers at Uppsala University, the Swedish University of Agricultural Sciences and, in Italy, IFOM – The FIRC Institute of Molecular Oncology and the Mario Negri Institute of Pharmacological Research. The researchers have been investigating how propranolol affects the emergence of vascular lesions in the form of CCMs.
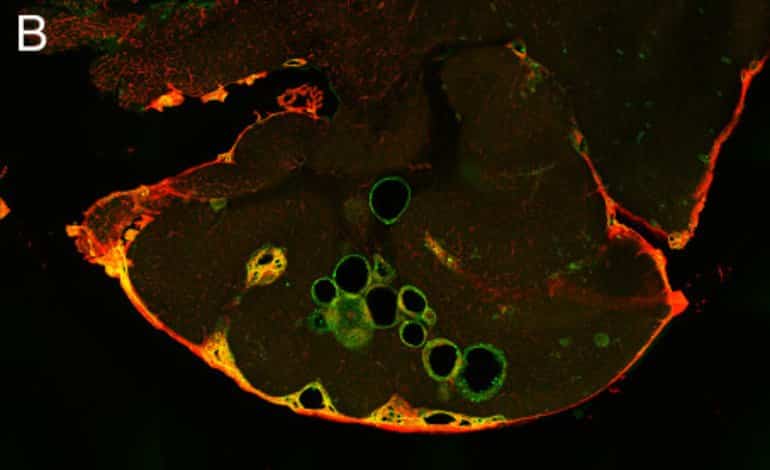
“We examined mice with vascular malformations in the brain – cavernomas or CCMs, as they’re called – that corresponded to the hereditary form of the condition in humans. The mice were given propranolol in their drinking water, and we were able to see that the cavernomas were becoming fewer and smaller. The blood vessels functioned better, too, with less leaking and improved contacts between their cells,” Magnusson says.
The propranolol dose administered to the animals was equivalent to the dose used to treat diseases in humans. Using an electron microscope, the researchers were able to study in detail how the drug affected the cavernomas.
The results show that propranolol can be used to shrink and stabilise vascular lesions, and may be a potential medicine for treating CCMs.
“What makes the study especially interesting is that right now, in Italy, a clinical study is under way in which CCM patients are to get two years’ treatment with propranolol. During this period, they’re being monitored by means of magnetic resonance imaging of the blood vessels, to see how the malformations are developing,” says Professor Elisabetta Dejana of Uppsala University’s Department of Immunology, Genetics and Pathology and IFOM in Italy.
Dejana heads the research group at Uppsala University that has been working on the new study, and is also taking part in the ongoing clinical study in Italy.
About this neuropharmacology research news
Source: Uppsala University
Contact: Peetra Magnusson – Uppsala University
Image: The image is credited to the researchers
Original Research: Closed access.
“Propranolol Reduces the Development of Lesions and Rescues Barrier Function in Cerebral Cavernous Malformations” by Oldenburg. J. et al. Stroke
Abstract
Propranolol Reduces the Development of Lesions and Rescues Barrier Function in Cerebral Cavernous Malformations
Background and Purpose:
Cerebral cavernous malformations (CCM) present as mulberry-like malformations of the microvasculature of the central nervous system. Current medical treatment of CCM lesions is limited to surgical removal of the vascular malformations. It is, therefore, important to identify therapeutic drug treatments for patients with CCM. Propranolol has shown great benefit in the treatment of infantile hemangioma. In addition, patients with CCM who receive propranolol have demonstrated a reduction of their lesions. Our investigation set out to provide preclinical data to support propranolol as a therapeutic treatment.
Methods:
An inducible endothelial-specific Ccm3 knockout murine model (CCM3iECKO) was used, with assessment of lesion quantity and size following oral treatment with propranolol. Scanning and transmission electron microscopy were used to characterize the CCM3iECKO lesions and the effects of propranolol on the disease. Immunofluorescent imaging was used to investigate pericyte coverage in the propranolol-treated CCM3iECKO mice.
Results:
With propranolol treatment, the lesion quantity, size, and volume decreased in both the brain and retina in the CCM3iECKO model. Novel characteristics of the CCM3iECKO lesions were discovered using electron microscopy, including plasmalemmal pits and thickening of the endothelial-pericyte basal membrane. These characteristics were absent with propranolol treatment. Pericyte coverage of the CCM3iECKO lesions increased after propranolol treatment, and vascular leakage was reduced.
Conclusions:
This study supports the concept that propranolol can be used to reduce and stabilize vascular lesions and can, therefore, be suggested as a pharmaceutical treatment for CCM.






