Summary: A new SPECT imaging study reveals those with treatment resistant depression have lower cerebral blood flow within the frontal, parietal and temporal lobes.
Source: IOS Press press release. The research paper will appear in The Journal of Alzheimer’s Disease Volume 63, Number 2.
Note: SPECT usage and Dr. Amen’s previous claims have been considered controversial by many, with claims of insufficient evidence being presented. If any reader has objection, or an informed opinion about this research, please comment below.
New research from the Amen Clinics shows that brain SPECT (single photon emission computed tomography) imaging, a study that measures blood flow and activity patterns, identifies who is likely to get better from depression and who is not. The study is published in the Journal of Alzheimer’s Disease, because depression is a highly treatable risk for cognitive decline and Alzheimer’s disease.
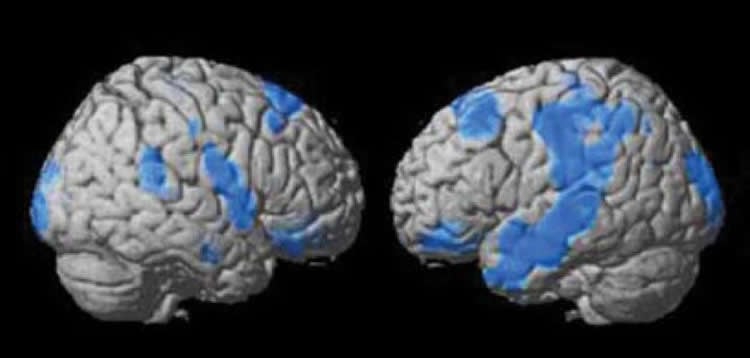
The researchers compared the SPECT scans of 507 depressed patients who responded to treatment to the scans of 106 patients who were considered non-responders. The study found that patients who did not respond to treatment had lower overall cerebral blood flow, especially in the frontal, temporal, and parietal lobes and in brain regions known to be affected by Alzheimer’s, including the right hippocampus and left precuneus.
Lead author psychiatrist Daniel G. Amen, MD says, “This is a critically important study. Knowing who is likely to get better from depression and who is not, will help treating physicians be sensitive to which patients are likely to need more help and need to be monitored more closely.” Treatment resistant depression is a major risk factor for suicide, divorce, and job loss. Dr. Amen also says, “This finding will also lead to more personalized treatment. For patients with low brain activity, stimulating the brain will be more important, than standard serotonin enhancing drugs that tend to lower brain activity.”
Source: Natalie Buchoz – IOS Press
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Amens Clinic.
Original Research: The study will appear in Journal of Alzheimer’s Disease. The abstract for “Deficits in Regional Cerebral Blood Flow on Brain SPECT Predict Treatment Resistant Depression” by Daniel G. Amen, Derek V. Taylor, Somayeh Meysami, Cyrus A. Raji is available at this Journal of Alzheimer’s Disease page. doi: 10.3233/JAD-170855.
[cbtabs][cbtab title=”MLA”]IOS Press “SPECT Imaging Predicts Outcomes For Those with Depression.” NeuroscienceNews. NeuroscienceNews, 20 March 2018.
<https://neurosciencenews.com/spect-depression-8673/>.[/cbtab][cbtab title=”APA”]IOS Press (2018, March 20). SPECT Imaging Predicts Outcomes For Those with Depression. NeuroscienceNews. Retrieved March 20, 2018 from https://neurosciencenews.com/spect-depression-8673/[/cbtab][cbtab title=”Chicago”]IOS Press “SPECT Imaging Predicts Outcomes For Those with Depression.” https://neurosciencenews.com/spect-depression-8673/ (accessed March 20, 2018).[/cbtab][/cbtabs]
Abstract:
Deficits in Regional Cerebral Blood Flow on Brain SPECT Predict Treatment Resistant Depression
Authors: Daniel G. Amen, Derek V. Taylor, Somayeh Meysami, Cyrus A. Raji
Background: Depression remains an important risk factor for Alzheimer’s disease, yet few neuroimaging biomarkers are available to identify treatment response in depression. Objective: To analyze and compare functional perfusion neuroimaging in persons with treatment resistant depression (TRD) compared to those experiencing full remission. Methods: A total of 951 subjects from a community psychiatry cohort were scanned with perfusion single photon emission computed tomography (SPECT) of the brain in both resting and task related settings. Of these, 78% experienced either full remission (n = 506) or partial remission (n = 237) and 11% were minimally responsive (n = 103) or non-responsive (11%, n=106). Severity of depression symptoms were used to define these groups with changes in the Beck Depression Inventory prior to and following treatment. Voxel-based analyses of brain SPECT images from full remission compared to the worsening group was conducted with the statistical parametric mapping software, version 8 (SPM 8). Multiple comparisons were accounted for with a false discovery rate (p < 0.001). Results: Persons with depression that worsened following treatment had reduced cerebral perfusion compared to full remission in the multiple regions including the bilateral frontal lobes, right hippocampus, left precuneus, and cerebellar vermis. Such differences were observed on both resting and concentration SPECT scans. Conclusion: Our findings identify imaging-based biomarkers in persons with depression related to treatment response. These findings have implications in understanding both depression to prognosis and its role as a risk factor for dementia.






