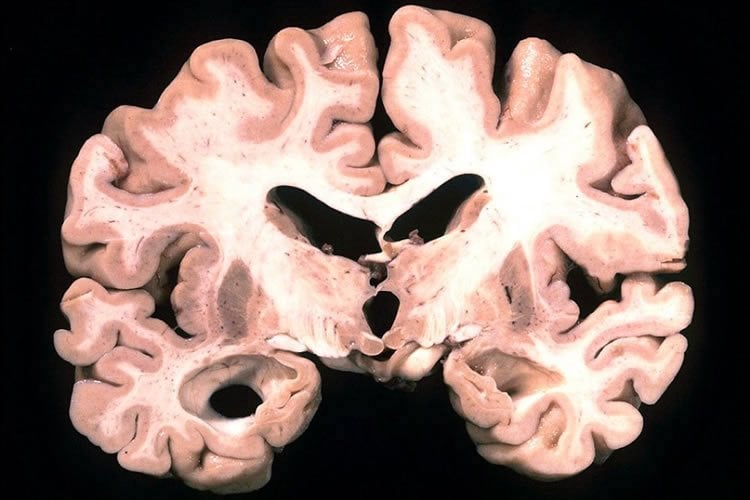
Researchers have found evidence of fungal infections in the brains of people with Alzheimer’s disease. The research was published in Nature’s Scientific Reports on 15 October 2015.
The team from Spain studied the brains of 11 people who had lived with Alzheimer’s disease and compared them to 11 healthy people who had died at a similar age. They investigated different regions of the brain, looking for evidence of fungal infection. They found evidence of fungal cells in nerve cells in several regions of the brain that become damaged in Alzheimer’s disease. They also found evidence of fungus in the cells that make up blood vessels, in people who had lived with Alzheimer’s disease, compared to those who did not have the disease.
Dr Laura Phipps, Science Communications Manager at Alzheimer’s Research UK, said:
“While this very small study suggests that fungal cells may be present in the brains of people with Alzheimer’s, we cannot conclude from this work that such infections cause or increase the risk of the disease. Without a corresponding medical history, we do not know whether the fungal infection occurred before or after the onset of Alzheimer’s disease, or whether this group of people had an increased risk of fungal infection due to other health complications. This study is a snapshot of the brain after death – we would need to see larger studies, following people with fungal infections for extended periods of time, to better understand whether there is a relationship between such infections and Alzheimer’s disease.
“Alzheimer’s Research UK is funding ongoing research investigating whether common infections could influence the progression of symptoms for people with Alzheimer’s. The best current evidence suggests that eating a healthy and balanced diet, not smoking, staying physically active and keeping weight and blood pressure in check can all help reduce the risk of dementia.”
Source: Alzheimer’s Research UK
Image Credit: The image is in the public domain
Original Research: Full open access research for “Different Brain Regions are Infected with Fungi in Alzheimer’s Disease” by Diana Pisa, Ruth Alonso, Alberto Rábano, Izaskun Rodal and Luis Carrasco in Scientific Reports. Published online October 15 2015 doi:10.1038/srep15015
Abstract
Different Brain Regions are Infected with Fungi in Alzheimer’s Disease
The possibility that Alzheimer’s disease (AD) has a microbial aetiology has been proposed by several researchers. Here, we provide evidence that tissue from the central nervous system (CNS) of AD patients contain fungal cells and hyphae. Fungal material can be detected both intra- and extracellularly using specific antibodies against several fungi. Different brain regions including external frontal cortex, cerebellar hemisphere, entorhinal cortex/hippocampus and choroid plexus contain fungal material, which is absent in brain tissue from control individuals. Analysis of brain sections from ten additional AD patients reveals that all are infected with fungi. Fungal infection is also observed in blood vessels, which may explain the vascular pathology frequently detected in AD patients. Sequencing of fungal DNA extracted from frozen CNS samples identifies several fungal species. Collectively, our findings provide compelling evidence for the existence of fungal infection in the CNS from AD patients, but not in control individuals.
“Different Brain Regions are Infected with Fungi in Alzheimer’s Disease” by Diana Pisa, Ruth Alonso, Alberto Rábano, Izaskun Rodal and Luis Carrasco in Scientific Reports. Published online October 15 2015 doi:10.1038/srep15015